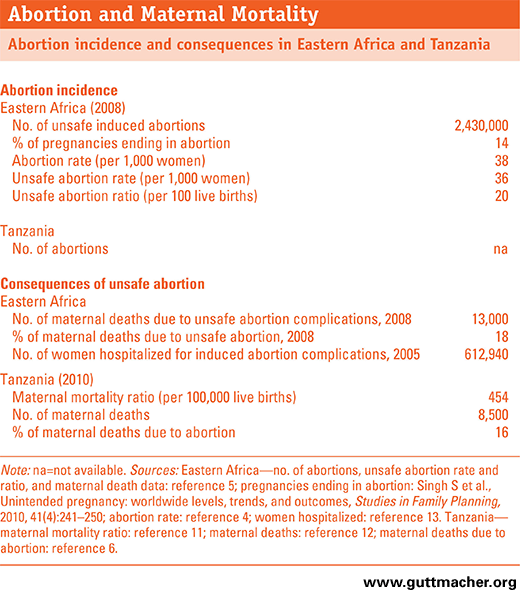
Although pregnancy termination is restricted by law in Tanzania, it is widely practiced and almost always unsafe, and contributes to the country’s high maternal morbidity and mortality. Yet the majority of abortion-related deaths are preventable, as are the unintended pregnancies associated with abortion. Better access to contraceptives, more comprehensive postabortion care and greater availability of safe abortion services within the current legal framework are critical to achieving the Millennium Development Goal 5 of reducing maternal mortality and ensuring universal access to reproductive health care by 2015.
This report summarizes the current evidence on induced abortion in Tanzania, clarifies existing law on the provision of abortion, and identifies key areas where government and program planners can take action to decrease levels of unintended pregnancy and unsafe abortion.