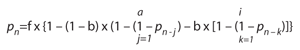California's family planning program, Family PACT (Planning, Access, Care and Treatment), was launched in 1997* and grew rapidly, serving 750,000 clients during its first year of operation and more than 1.5 million in 2003. It replaced a limited family planning program that had served approximately 500,000 women and men annually through state contracts with about 100 community and public clinics. Under the new program, all Medi-Cal (California's Medicaid program) providers in the state are eligible to participate, and provider reimbursement has been changed from a contractual arrangement to a fee-for-service system. By FY 2002–2003, nearly 3,000 providers, including private practitioners as well as providers at community and public health clinics, were participating in the program.1
Family PACT plays an important role in providing family planning services for low-income women and men in California. Many low-income women in the state do not have private insurance† and do not qualify for coverage for contraceptive services through other public programs. For example, Medi-Cal almost exclusively serves current and recent participants in the California welfare program,2 for which many low-income women are not eligible because they do not have a child, do not meet residency requirements, have incomes above the federal poverty level or have exceeded the program's time limits. California's Title X program provides general support for education, outreach and infrastructure to certain public and nonprofit family planning agencies, but it does not cover clinical services for individuals.††3 In contrast, any person whose income does not exceed 200% of the federal poverty level and who has no other public or private source of reproductive health care coverage is eligible for Family PACT services.
The program has several innovative features that have contributed to its rapid growth and client acceptability. Determination of client eligibility and enrollment are performed at each clinical site and are based on client self- report of family size and income; services are reimbursed on a fee-for-service basis; the service network includes both private- and public-sector providers; and clinic offices as well as pharmacies are able to distribute over-the-counter and prescription drugs. Family PACT provides all methods of contraception approved by the U.S. Food and Drug Administration, as well as male and female sterilization, HIV testing, screening and treatment for STDs, and limited cancer screening and infertility services.4
In 1999, after an initial evaluation of the program demonstrated adherence to standards of care and improvement in access to services, California received a federal Medicaid funding waiver† to help support Family PACT. The waiver funded the development of outreach and recruitment programs to improve access to family planning services for hard-to-reach populations (e.g., adolescents, men and residents of underserved counties) as well as an expansion in the scope of services provided under the program. As part of the initial evaluation, we estimated that more than 108,000 unintended pregnancies were averted through contraceptive services provided through Family PACT during the program's first year of operation (FY 1997–1998); these pregnancies would have resulted in an estimated 50,000 births, 41,000 induced abortions, 16,000 spontaneous abortions and 1,000 ectopic pregnancies.5
In the years that followed, several changes occurred that may have affected the number of pregnancies averted through the program. Most importantly, the number of clients served annually doubled.6 In addition, new contraceptive methods were introduced after the initial evaluation: Dedicated emergency contraception products were added to program benefits in 1999 and 2001, and the contraceptive patch and ring were added in 2002. In this analysis, we update our estimates of pregnancies averted using data from 2002, explore the range of possible estimates and examine the factors that have had the greatest effect on the number of pregnancies averted.
METHODS
We employed the same methodology that we established for the initial evaluation of Family PACT.7 Thus, we estimated the number of pregnancies averted through use of Family PACT services to be the difference between the number of pregnancies expected in the absence of the program (taking into account participants' contraceptive use before enrollment) and the number expected among women using the methods provided through the program.
To update these estimates for 2002, we used new data regarding the number and characteristics of clients served and the array of contraceptive methods dispensed. To estimate the probability that Family PACT clients would become pregnant if the program did not exist, we used clients' self-reports of contraceptive use prior to enrollment, determined from a review conducted in 2000–2001 of medical records from 868 women who were new to Family PACT and were not pregnant or seeking pregnancy.
Contraceptive Coverage
We estimated the number of months of contraceptive coverage provided under the Family PACT program on the basis of paid claims data on the quantity and type of contraceptives dispensed. The coverage for long-term methods (tubal ligations, IUDs and implants) was calculated as the number of months between the provision date and December 2003. We imposed this two-year cap to avoid predicting pregnancies far into the future; the number of women receiving long-term methods through the program was relatively small (just 2% of women receiving contraceptive methods), so excluding the full duration of contraceptive benefit did not have a large effect on our estimate of pregnancies averted.
Because clients do not necessarily use all of the contraceptives they receive, the number of months of contraceptive coverage for short-term methods, such as condoms and oral contraceptives, was adjusted to account for method discontinuation. For oral contraceptives, we assumed that a woman who did not return for refills used half of the pills dispensed to her. We assumed that women who received one packet of emergency contraceptives used it; however, if women were given more than one packet (i.e., as advance provision), we assumed that 50% used the second packet.8 For condoms and other barrier methods, we assumed, given findings of the medical record review, that the supplies dispensed by the clinics provided two months of contraceptive coverage. The exact quantity of supplies dispensed by pharmacies was available, and we assumed a month of protection for every 12 condoms dispensed. Each depot medroxyprogesterone acetate injection was assumed to provide three months of contraceptive coverage.
Pregnancies
To estimate the number of pregnancies among clients (with or without Family PACT), we modeled the month-by-month experience of a woman who is at risk for pregnancy,§ beginning with the month when the contraceptive was dispensed and ending with the last month of contraceptive coverage. For each month, we calculated the probability that the woman would become pregnant, based on three factors: the failure rate of the method used (i.e., the proportion of users who experience a pregnancy in a year), age-specific fecundity and the estimated probability of pregnancy in previous months. Modeling pregnancies averted by month allowed us to use specific contraceptive dispensing data on months of coverage, rather than assuming a year of coverage for each client. It also allowed for repeat pregnancies within a year, which is a common outcome among women who use low-efficacy methods and terminate pregnancies in abortion.**
For this analysis, we made the same assumptions about contraceptive failure rates and pregnancy outcomes as we did in the original study (Table 1). The contraceptive patch and ring were assumed to have the same probability of failure as oral contraceptives. Failure rates for contraceptives were adapted from Trussell and colleagues.9
Because the outcomes of unintended pregnancies differ from those of intended pregnancies, the distribution of pregnancy outcomes used in this study was adapted from Henshaw.10 Thus, we estimated the number of miscarriages as 10% of abortions plus 20% of births, and then readjusted the distribution of pregnancy outcomes to sum to 100%. We assumed the number of ectopic pregnancies to be 1% of the number of unintended pregnancies.11 For women younger than 20, we estimated that 49% of pregnancies ended in birth, 36% in induced abortion, 14% in spontaneous abortion and 1% in ectopic pregnancy. For women 20 or older, we estimated that 45% of pregnancies resulted in birth, 39% in induced abortion, 15% in spontaneous abortion and 1% in ectopic pregnancy.
Sensitivity Analyses
We examined the sensitivity of our estimates to changes in our assumptions about contraceptive failure rates, contraceptive continuation and contraceptive use in the absence of the program. To examine the effects of inconsistent or ineffective contraceptive use on our estimates, we calculated how many pregnancies would be averted if women experienced contraceptive failure rates that were substantially higher than the national average—specifically, 175% of the rates in Table 1, for all methods that involve risk of user error or discontinuation.12 To model ideal contraceptive use, we estimated the number of pregnancies that would be averted if failure rates matched the "perfect-use" rates cited in Contraceptive Technology (we used the 1998 edition, for consistency with our previous evaluation).13
In addition, we examined the effect of our adjustment to account for method discontinuation by estimating the number of pregnancies that would be averted if women who did not return used all (rather than half) of the contraceptives they received. Finally, we estimated the number of pregnancies that would be averted in the absence of Family PACT in three less realistic scenarios: Women remain sexually active but use no method of contraception; half of women abstain from intercourse; and all contraceptive users switch to condoms because prescription methods are too expensive without subsidized services.
RESULTS
Methods Used Prior to Program Enrollment
Before receiving Family PACT contraceptive services, 27% of female clients were using no method of contraception, and 3% were using natural family planning methods, such as periodic abstinence and withdrawal (Table 2). Nearly four in 10 women (38%) were using condoms, and the remaining 32% were using hormonal methods or IUDs. Women aged 15–19 were more likely than women aged 20–44 to be using condoms and less likely to be using hormonal or intrauterine contraceptives.
The profile of method use prior to program enrollment has changed in the years since the initial evaluation of Family PACT services. Most notably, condom use has increased among teenagers. Fifty-two percent of women aged 15–19 entering the program were using condoms in 2000, compared with 31% at the earlier evaluation. Condom use also increased, although to a lesser degree (from 25% to 34%), among women aged 20–44. This shift toward condom use was the result of reductions in the proportions of women who were using no method of contraception or hormonal methods. As a result of the substantial reduction in the use of no method among women aged 15–19, the estimated annual pregnancy rate in this group (assuming the failure rates shown in Table 1) declined from 55% to 47% between 1997–1998 and 2002 (not shown). The estimated pregnancy rate among women aged 20–44 remained stable (43%) during this time period.
Contraceptive Dispensing in 2002
Nearly a million women received contraceptive methods through Family PACT in 2002 (Table 3)—202,000 women aged 15–19 and 724,000 women aged 20–44. Claims included payment for oral contraceptives for about 478,000 clients, condoms and other barrier methods for 412,000, injectable contraceptives for 187,000 and long-term methods for 21,000. Emergency contraception was dispensed without any other method to 27,000 clients. About 7,000 women received the new contraceptive patch, and 300 received the contraceptive ring. Many women received more than one type of method, either for dual use or because they switched methods during the year.
The claims paid for female clients during 2002 provided each woman with an average of 6.9 months of contraceptive coverage. Women aged 15–19 received 0.7 fewer months of contraceptive coverage than women aged 20–44 (6.4 vs. 7.1). Part of this difference can be attributed to younger women's greater reliance on short-acting methods. However, even among clients receiving short-acting methods, younger women received slightly less contraceptive coverage: two weeks less of oral and injectable contraceptive coverage and one week less of barrier method supplies.
Overall, nearly 6.4 million woman-months of contraception were dispensed through Family PACT during 2002. Oral contraceptives accounted for the majority (57%) of the woman-months of contraception dispensed, followed by barrier methods (19%), the injectable (18%) and long-term methods (6%). Coverage from long-term methods is underestimated because of the two-year cap. The contraceptive patch and ring were not covered by the program until November 2002 and thus accounted for a negligible proportion of the methods dispensed during the year; together, the patch, the ring and emergency contraceptives provided less than 1% of woman-months of protection.
The proportion of contraceptive protection provided by barrier methods in 2002 (19%) represented a substantial increase from the proportion in FY 1997–1998 (12%).14 The proportion provided by oral contraceptives declined from 63% to 57%.
Pregnancies Averted
On the basis of the quantity and type of contraceptive methods dispensed, we estimate that because of method failure and noncompliance, women participating in Family PACT experienced almost 25,000 pregnancies during the time they were using contraceptives (Table 4, page 130). If these women had been using the same method array as women new to the program had been using prior to enrollment, they would have experienced 230,000 pregnancies. The difference, 205,000 pregnancies, is an estimate of the number of pregnancies averted through Family PACT services in 2002. Among women aged 15–19, an estimated 43,600 pregnancies were averted; these pregnancies would have led to 21,400 births, 15,700 abortions, 6,100 spontaneous abortions and 400 ectopic pregnancies. Among women aged 20–44, the program prevented an estimated 161,300 pregnancies, which would have resulted in 72,600 unintended births, 62,900 abortions, 24,200 spontaneous abortions and 1,600 ectopic pregnancies. The number of pregnancies averted through contraceptive services in 2002 was nearly twice the figure from 1997–1998, when 108,000 pregnancies (including 41,500 induced abortions and 49,600 unintended births) were averted.
We examined the extent to which several reasonable alternative scenarios affected our estimates of pregnancies averted. The impact of these alternative scenarios ranged from a 3% decrease in our estimates to a 21% increase (Table 5, page 130). First, if women who used methods subject to user error were to experience failure rates 175% of those in our base scenario, the Family PACT program would avert an additional 28,400 pregnancies (14% more than we estimated), primarily because in the absence of the program, women would become more likely to rely on methods that require user intervention. If women were to attain perfect-use contraceptive failure rates, the number of pregnancies averted would be 3% less than in our base scenario. If women in the program achieved these lower contraceptive failure rates, perhaps through education and counseling provided by the program, but women outside the program did not, then the number of pregnancies averted would be 10% above the base estimate. Finally, if women used all of the contraceptive supplies provided to them during the year, then an additional 42,000 pregnancies would be averted, 21% more than in our base case.
We also created three additional but less likely scenarios of what would happen in the absence of Family PACT. First, if women used no method at all in the absence of the program but continued to be sexually active, the number of pregnancies averted would increase by almost 200% over the base case, to 582,000. If half of the women abstained from intercourse in the absence of contraceptive services, the number of pregnancies averted would be reduced to 90,000, less than half of the base estimate. Finally, if women who were using a prescription method when they entered the program switched to condoms in the absence of the program, the number of pregnancies averted would be 12,400 (6%) higher than the base estimate.
DISCUSSION
The growth of the Family PACT program has been substantial. The number of women served annually doubled during the program's first five years, and the Medicaid waiver that was granted in 1999 allowed for the expansion of services. This study indicates that the increase in the number of women using contraceptive services resulted in a significant reduction in unintended pregnancy.
This reexamination of the program's impact on fertility has yielded new insight into what makes a family planning program effective at reducing the incidence of unintended pregnancy. Because all contraceptive methods substantially reduce the risk of pregnancy, the ability of a program to prevent pregnancy lies primarily in its provision of contraceptive methods to women who would otherwise not use them. Enabling women to switch from methods with relatively high failure rates (such as condoms) to more effective methods is also an important, albeit less powerful, factor. Evidence for these conclusions is provided by the scenarios that produced the extreme estimates of pregnancies averted. Were all female clients to use no contraceptive method in the absence of Family PACT, almost 582,000 pregnancies would have been averted by the program. If half of the women in the program ceased having sexual intercourse without Family PACT services, the program would have averted only 90,000 pregnancies. And if the women who entered the program using a prescription method of contraception switched to over-the-counter methods in the absence of subsidized services, the effect on the estimated number of pregnancies averted would be relatively small—a 6% increase.
Our estimate of 205,000 pregnancies averted appears to be robust to assumptions about failure rates. The estimate would increase by as much as 14% if women were to experience very high contraceptive failure rates or decrease by 3% if women were to experience perfect-use failure rates. Our efforts to account for method discontinuation by assuming that women who do not return for subsequent visits use only half of the short-term methods dispensed reduced the estimate by 21%.
For this study, it was our intention to provide a conservative estimate of pregnancies averted. Because Family PACT does not cover abortion services or prenatal care, the claims data do not provide precise information about pregnancies and pregnancy outcomes experienced by program participants. To be conservative, we estimated pregnancies only for months in which contraceptive coverage was provided through the program, allowing for method discontinuation and capping the duration of coverage at two years. In addition, we did not estimate pregnancies averted through contraceptive distribution to males, who make up about 10% of the program's clients.15
Our sensitivity analyses indicate that the most pronounced effects on our estimate come from altering assumptions about what women would do in the absence of Family PACT. In our models, we assumed that women's method use in the absence of the program would be similar to that of Family PACT clients at the time of their first visit. We chose this scenario because it is more conservative and realistic than assuming that women would use no method of contraception in the absence of the program. It also reflects clients' increased reliance on condoms prior to their initial Family PACT visit: During the program's first five years, the proportion of new female clients who had been using condoms grew substantially; the increase was particularly large (from 31% to 52%) among women younger than 20. In both age-groups, most of the increase in condom use prior to enrollment was due to a decline in the use of more effective methods of contraception, although the proportion of women using no method decreased as well, particularly among younger women. The net effect of these changes is that the estimated annual probability of pregnancy among women younger than 20 in the absence of Family PACT has declined from 55% to 47%, thus approaching the 43% pregnancy rate seen among women 20 or older.
Whether women would continue using a method in the absence of Family PACT depends on their ability to pay for contraceptives or to find other low-cost sources of supplies. Some women might stop using their prior method altogether because they could no longer afford to pay for contraceptives out of pocket. Others might stop having intercourse in the absence of family planning services, although we suspect that this response would not be widespread, given the high rates of pregnancy and abortion experienced by this client population. According to our review of Family PACT medical records, three-quarters of women—including more than a third of those younger than 20—had had at least one pregnancy, and almost one in five had had at least one abortion.
Unintended pregnancy is a widespread problem that can have serious consequences. It is associated with significant, negative public health outcomes and social burdens as well as personal costs.16 Averting 205,000 pregnancies would save federal, state and local governments an estimated $1.1 billion over two years, or $2.76 for every dollar expended on family planning services.17 Thus, preventing these pregnancies brings not only personal and social benefits but significant public-sector savings on health care, social services and education for women and their children.