The October 2018 appointment of Justice Brett Kavanaugh to the U.S. Supreme Court has called into question the future of Roe v. Wade and abortion access in the United States. Just one month after Justice Kavanaugh took his seat on the bench, voters in Alabama and West Virginia approved state constitutional amendments intended to allow for additional abortion restrictions or even pave the way for outright bans on abortion in the event Roe is undermined or overturned.1
Although the changing composition of the Supreme Court has heightened the risks, efforts to restrict abortion are not new. Policymakers hostile to abortion have been working to undermine abortion care since Roe was decided. As a result, access to abortion already looks very different from state to state, and a person’s access to timely, affordable abortion care can be profoundly impacted by her race, socioeconomic status and available resources.
As the country looks ahead to a potential future in which the Supreme Court retracts federal protections, states can take stock of their existing policies and consider what is needed to protect or expand access to abortion care. Policymakers in some states have already made progress on this issue, and these examples can serve as a useful starting place—albeit not a sufficient end goal—for shoring up abortion access in supportive states.
Affirming and Protecting the Right to Abortion
In anticipation of diminished protections at the federal level, states can act to ensure that their own laws and policies affirm and protect the right to abortion. The most robust protection at the state level exists when the right to abortion is safeguarded by the state constitution. According to an analysis by the Center for Reproductive Rights, there are nine states in which the highest state court has interpreted its state constitution to protect the right to abortion (see figure 1).2 In many of these cases, state constitutional protections have served as greater protection for abortion than the federal constitutional standard.3 In most cases, however, inserting or establishing new rights under a state constitution is an arduous undertaking that may not be practical or possible.
Another option is to enact state statutory protections that—although not as secure as constitutional rights because statutes can be more easily repealed—could help preserve access to abortion in the event that federal protections are reduced. Eight states have adopted laws intended to reflect and affirm the standards established under Roe v. Wade and subsequent U.S. Supreme Court rulings, which protect the right to abortion up to viability and whenever a pregnancy threatens a woman’s life or health.4
More recently, efforts in a handful of states have shifted focus from the Roe viability framework to a broader model that seeks to prevent the government from interfering in an individual’s ability to access abortion care throughout pregnancy. Most notably, Oregon enacted a new law in 2017 that prohibits the state from interfering with or restricting "the choice of a consenting individual to terminate the individual’s pregnancy"; the law makes clear that this includes interference as a result of "the regulation or provision of benefits, facilities, services or information."5
Providing Abortion Coverage
Currently, affordability is one of the most significant barriers to obtaining abortion care in the United States. The average amount paid for an early medication abortion (up to 9 weeks’ gestation) was $535 in 2014, and abortion costs tend to increase as a pregnancy progresses.6 Associated expenses, such as time off from work, child care, travel and lodging, can add hundreds of dollars to this already formidable price tag. Insurance coverage can help people overcome some of these financial barriers, but the Hyde Amendment bars federal funds from paying for coverage of most abortion care under the Medicaid program and state-level restrictions deny insurance coverage of abortion to millions of people.
State lawmakers can greatly improve access to abortion by providing coverage to Medicaid enrollees using state dollars. In 2017, Republican Gov. Bruce Rauner of Illinois signed a bill lifting the state’s ban on Medicaid coverage of abortion, extending coverage to the half million women of reproductive age enrolled in the program.7 In total, 15 states currently cover abortion care under Medicaid.8
Policymakers can also follow the lead of California and, more recently, New York, Oregon and Washington, by requiring private insurers to include abortion as a covered service.9–11 Failing that, they can allow private plans to choose to cover abortion by lifting the bans that prevent it in the first place. Currently, 26 states restrict abortion coverage in private health insurance plans offered through the Affordable Care Act’s marketplaces, and 11 of these states also restrict abortion coverage in all or most other private insurance plans.12
Many people in the United States are denied access to public or private insurance coverage—for any service, not only abortion—often because of their immigration status. Oregon addressed this problem in 2017, when it established a program to reimburse individuals not otherwise eligible for medical assistance (such as people barred from Medicaid enrollment because of their immigration status) for reproductive health care, including abortion care.10
Ensuring Access to Information
A bedrock principle of medical practice and ethics is informed consent, a process meant to ensure that patients receive accurate and relevant information about medical conditions and possible treatments, including the risks, benefits and alternatives. This process is so important that it has been codified by the legislature or established by legal decision in every state.13 In the context of abortion, however, these principles have been perversely used as an excuse to require providers to give their patients misleading, irrelevant and erroneous information.
Thirty states require abortion counseling specifically designed to dissuade a patient from obtaining an abortion, such as information asserting that personhood begins at conception; unnecessarily detailed descriptions of fetal development; or scientifically inaccurate claims about the ability of the fetus to feel pain or that the patient’s mental health could be negatively impacted by an abortion.14 Several states impose specific abortion counseling requirements that reflect a more balanced approach in terms of content, but nonetheless single out abortion providers for unnecessary directives given that they are already bound by the principles of informed consent applicable to all members of the medical profession.
Recently, to directly combat abortion counseling based on false and irrelevant information, legislators in Virginia and Wisconsin, among other states, proposed measures intended to affirm a patient’s right to medically accurate information.15,16 These proposals take one of two differing approaches. Virginia’s proposed legislation would allow abortion providers to ignore state laws that impose medically inaccurate or irrelevant requirements, such as misleading counseling mandates or waiting periods between an initial counseling appointment and having the procedure. Wisconsin’s proposal is a broader response to restrictions on medical providers’ speech; it would prohibit political interference in any kind of health care, including abortion.
Supporting Adolescents’ Access
Thirty-seven states require parental involvement before an adolescent obtains an abortion.17 These restrictions run contrary to the recommendations of numerous leading medical associations, which support allowing pregnant patients—including those younger than 18—to make the decision about whether to carry to term or end a pregnancy and to have agency over who else is involved in the process.18
A few states have adopted policies that affirm the rights of young people to obtain abortion care. The most protective of these is a District of Columbia regulation that explicitly establishes the right of patients younger than 18 to consent to abortion care without parental involvement.19 Connecticut also affirms adolescents’ right to consent without parental involvement, but it requires enhanced counseling from the abortion provider for adolescents younger than 16.20
Maine has more limited protections in place allowing patients younger than 18 to consent to having an abortion, but only after enhanced counseling and a determination from the provider that the adolescent has the ability to consent.21 There are also 11 states that are effectively silent on the question of adolescents’ right to consent to abortion, either because they had a parental involvement requirement that was struck down in court or because they have never enacted such a requirement.22 This silence in the law allows a medical professional to provide abortion services without parental involvement but could also result in a situation similar to that in Maine, in which the provider exercises sole discretion about whether or not to offer care without parental involvement.
In addition, education that includes information on abortion is key to ensuring that young people can exercise their rights. California, Vermont and DC require that information about abortion be included as part of comprehensive sex education received by students in middle and high school.23–25 However, most states do not mandate any sex education or require any instruction related to abortion when sex education is provided. In fact, several states go so far as to prohibit instruction on abortion.
Preventing Clinic Violence
Antiabortion zealotry has led to the murder of abortion providers and clinic staff as well as to other serious forms of violence and harassment, including bombings, arson, vandalism, and violent or disruptive protests and blockades. According to the National Abortion Federation, hostile, threatening and harassing behavior directed at clinics and clinic staff escalated in 2017: In addition to the first attempted abortion facility bombing in many years, "trespassing more than tripled, death threats/threats of harm nearly doubled, and incidents of obstruction rose from 580 in 2016 to more than 1,700 in 2017."26 Moreover, online platforms and social media sites are now routinely used to harass providers.
In 1994, the federal government enacted the Freedom of Access to Clinic Entrances (FACE) Act, which prohibits intentional property damage and the use of "force or threat of force or…physical obstruction" to "injure, intimidate or interfere with" someone entering a health care facility.27 In addition, 14 states and DC have established their own protections for clinic access.28 These laws are often similar to the FACE Act and can be an important tool for ensuring that state resources are committed to and utilized for enforcement. This may be especially important at times like the present, when a federal administration hostile to abortion is unlikely to dedicate resources to robust enforcement of the FACE Act.
States can also protect the confidentiality of clinic staff and volunteers by limiting access to personal information, such as home addresses and telephone numbers. For example, California allows staff and volunteers at reproductive health facilities to use an alternate address for communication with the state and makes it a crime to post residential information online with the intent to threaten or incite harm to clinic staff or volunteers.29
Expanding the Pool of Abortion Providers
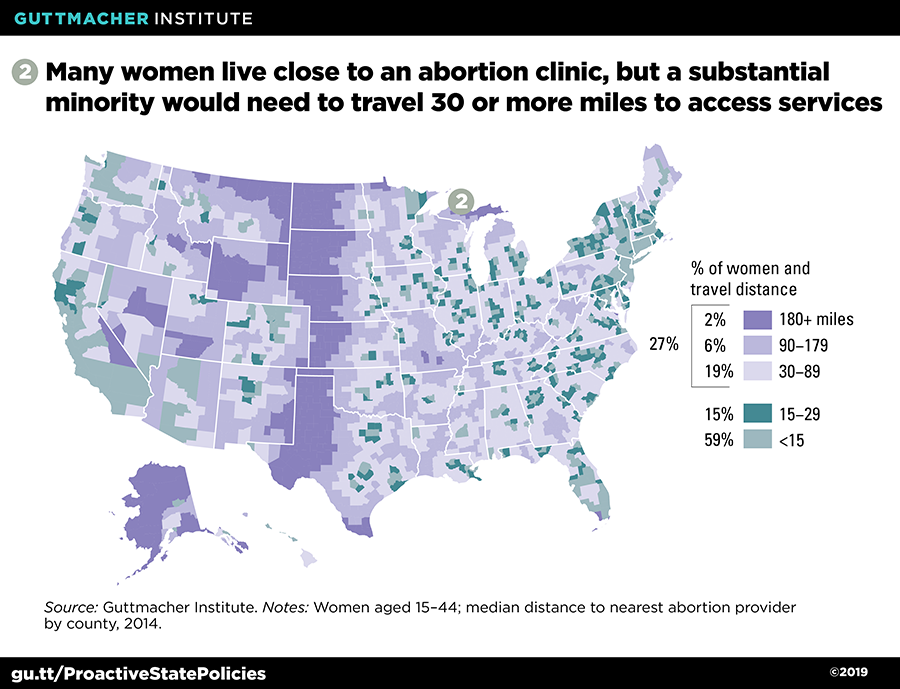
In the decades since Roe v. Wade, abortion care has evolved as a primarily clinic-based service, segregated from the resources and infrastructure dedicated to other health care. There are huge gaps in access to clinic-based care, including distance: One-quarter of women of reproductive age would need to travel at least 30 miles to reach the nearest abortion clinic (see figure 2).30 One way to address gaps in abortion care is to expand the pool of providers offering that care.
Specialized abortion providers are often the target of regulations known as TRAP ("targeted regulation of abortion providers") laws, which single out abortion clinics and providers with onerous restrictions intended to shutter their doors and make abortion more difficult for patients to access.31 States interested in expanding the pool of abortion providers can start by ensuring they do not subject clinics and providers to unnecessary regulations that have nothing to do with ensuring patient health or safety.
More generally, abortion is not well integrated into primary care in the United States, and even among obstetrician-gynecologists, there is a shortage of providers offering abortion care.32,33 One barrier these potential providers face is a basic lack of training. Since 1996, the Accreditation Council for Graduate Medical Education (ACGME) has required obstetrics and gynecology residency programs to include training on abortion.34 Yet a recent survey found that many of these residency programs only provide this training on a separate, opt-in basis or do not provide training at all.35 One possible way to address this lack of training is to mandate it in state law: California enacted a law in 2002 that mirrors the ACGME accreditation requirements.36 States could go further by requiring training in abortion care for a wider range of physicians, such as family medicine and internal medicine doctors.
Another way to expand the pool of abortion providers is to allow advanced practice clinicians (APCs) to provide medication and surgical abortion care in the first trimester. California enacted a law in 2013 that expands provision to nurse practitioners, certified nurse-midwives and physician assistants.37 The law was enacted after a five-year pilot program determined that APCs provide high-quality and safe abortion services comparable with physicians.38 Litigation may also be a useful tool in some states; for example, cases challenging physician-only abortion provision laws are pending in Maine and Montana.
Expanding Online and Telehealth Access
People in the United States are increasingly accessing health care products and services in new ways, including online pharmacies, virtual telehealth consultations and apps that help users manage a variety of health issues. As states invest more broadly in these emerging models and as more consumers use them, it is essential to make sure abortion is not left out.
Telemedicine is a safe and effective way of expanding access to medication abortion and is already available in at least 10 states.39,40 However, 17 states effectively or explicitly ban provision of medication abortion by a clinician who is not physically present with the patient.41 By lifting these restrictions and supporting telemedicine practices, state lawmakers can facilitate access to underserved communities, expand access to other groups of patients and fill gaps created by an increasingly hostile policy environment. In order to ensure full and equitable access to this model of care, policymakers must also mandate that Medicaid and private insurance plans not only cover abortion care, but also cover telehealth services to the same extent as in-person care.
Creating a Safe Policy Environment for Self-Managed Care
Another way to preserve and expand access to abortion is to promote policies and practices that support individuals who self-manage their abortions (see "Self-Managed Medication Abortion: Expanding the Available Options for U.S. Abortion Care," 2018). Evidence suggests that medication abortion can be safely and effectively self-managed, and data indicate that some women in the United States have opted to self-manage their abortions. This trend will likely increase in the years to come, both as a response to diminishing access and because safe and effective self-management offers enhanced privacy and autonomy for many people.
Although health and safety risks appear to be minimal with self-managed medication abortion, the risk of criminalization remains significant, particularly among groups who are already disproportionately criminalized, such as people of color. According to the SIA Legal Team, "there are 7 states with laws directly criminalizing self-induced abortions, 10 states with laws criminalizing harm to fetuses that lack adequate exemptions for the pregnant person, and 14 states with criminal abortion laws that have been and could be misapplied to people who self-induce."42 To help create a safe policy environment, states can remove or amend these laws to prevent their use against individuals who self-manage abortion. Legislation could include provisions to educate stakeholders—including health care providers and law enforcement personnel—about self-managed abortion to encourage supportive rather than punitive community responses.
Ultimately, with such uncertainty surrounding the future of Roe v. Wade, it is tempting to focus on the standards and protections that abortion rights supporters do not want to lose. But with this uncertainty comes a real opportunity to envision rights that go beyond those established by Roe and imagine a future of expanded, accessible and affordable abortion care without stigma.