Maternal mortality has declined considerably in Bangladesh over the past few decades. Some of that decline—though precisely how much cannot be quantified—is likely attributable to the country’s menstrual regulation program, which allows women to establish nonpregnancy safely after a missed period and thus avoid recourse to unsafe abortion.
Menstrual Regulation, Unsafe Abortion And Maternal Health in Bangladesh
Author(s)
Altaf Hossain, Isaac Maddow-Zimet, Susheela Singh and Lisa RemezReproductive rights are under attack. Will you help us fight back with facts?
Key Points
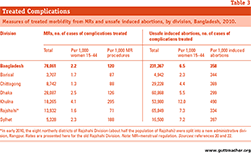
• Unsafe clandestine abortion persists in Bangladesh. In 2010, some 231,000 led to complications that were treated at health facilities, but another 341,000 cases were not. In all, 572,000 unsafe procedures led to complications that year.
• Recourse to unsafe abortion can be avoided by use of the safe, government sanctioned service of menstrual regulation (MR)—establishing nonpregnancy after a missed period, most often using manual vacuum aspiration. In 2010, an estimated 653,000 women obtained MRs, a rate of 18 per 1,000 women of reproductive age.
• The rate at which MRs result in complications that are treated in facilities is one-third that of the complications of induced abortions—120 per 1,000 MRs vs. 357 per 1,000 induced abortions.
• There is room for improvement in MR service provision, however. In 2010, 43% of the facilities that could potentially offer it did not. Moreover, one-third of rural primary health care facilities did not provide the service. These are staffed by Family Welfare Visitors, recognized to be the backbone of the MR program. In addition, one-quarter of all MR clients were denied the procedure.
• To assure that trends toward lower abortion-related morbidity and mortality continue, women need expanded access to the means of averting unsafe abortion. To that end, the government needs to address barriers to widespread, safe MR services, including women’s limited knowledge of their availability, the reasons why facilities do not provide MRs or reject women who seek one, and the often poor quality of care.
Bangladesh is making solid progress toward meeting the Millennium Development Goal of reducing maternal mortality by three-quarters between 1990 and 2015.1 According to a commonly used indicator, the maternal mortality ratio, maternal deaths fell by at least 60% from 1990 to 2010–2011 (Figure 1).2,3 The two official government studies of maternal mortality (known as Bangladesh Maternal Mortality and Health Care Services Surveys, or BMMS*), which were conducted in 20014 and 2010,5 offer further evidence of this steep decline: Their findings show a drop in maternal mortality of two-fifths in less than one decade.
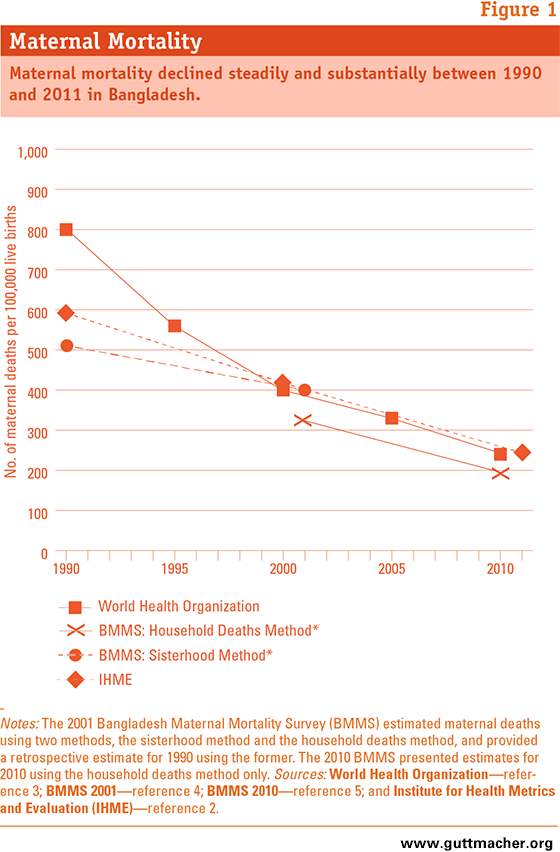
We know that the country has made great strides in reducing maternal mortality. But we know less well which factors, and in what combination, contributed to the decline. As in most countries that have made similar progress, evidence suggests that Bangladesh has succeeded in reducing deaths during pregnancy and childbirth by improving access to maternal health care and lowering fertility, especially births that pose above-average health risks (e.g., those to high-parity women). What makes the country unique, however, is the potential contribution of an authorized procedure—known as menstrual regulation, or MR—to "establish nonpregnancy" after a missed period.6
The unique contribution of MR to women’s health care in Bangladesh dates from the early 1970s. Bangladesh’s current penal code, which dates from 1860, when it was a British colony, outlaws all induced abortions except those needed to save the life of the pregnant woman.7 A legal ruling exempted MR from being regulated by the penal code, and subsequently, the procedure became part of the national family planning program in 1979.8
MRs are allowed up to 10 weeks after the last menstrual period (LMP) if performed by a physician.9 Family welfare visitors (FWVs) and paramedics such as sub- assistant community medical officers (SACMOs) are permitted to provide MR services up to eight weeks after the LMP. The predominantly female FWVs have a minimum of 10 years of schooling and receive at least 18 months’ training in reproductive and child health services, including training in how to perform MRs.10 (SACMOs have similar levels of general schooling as FWVs but take three years of basic courses in primary care and reproductive and child health services.) Given the limited number of physicians in the country, allowing FWVs to provide MRs not only expands access to an essential service but also costs less; having FWVs be the backbone of the program is a further plus in a predominantly Muslim culture such as Bangladesh where many women—and their husbands—feel most comfortable when women get care from other women.10 FWVs are posted at primary care facilities across the country, particularly at union health and family welfare centres (UH&FWCs). These facilities are located primarily in rural areas, where three-quarters of Bangladeshis live.11
MR procedures, which are officially provided by the government free of charge, are safe uterine evacuations that meet governmental criteria and, at least as of 2012, have been primarily done using manual vacuum aspiration (MVA). They are practiced widely throughout the country at all levels of the health system, from primary care clinics to tertiary care medical college hospitals and district hospitals. From the late 1970s through the mid-1990s, the government and international donors continuously supported the recruitment and training of FWVs to perform MRs.10 Recruitment was stopped in 199412 and has only recently resumed.13 Unfortunately, the interruption in recruiting has left the program playing catch-up in terms of having sufficient numbers of trained FWVs: As of the end of 2011, the total number of health professionals trained in MR stood at approximately 10,600 doctors and 7,200 paramedics, primarily FWVs (and among these, about 4,700 paramedics have received refresher training).14
If MRs were universally accessible in Bangladesh, they could greatly reduce the potential need for women to have an unsafe clandestine abortion. Currently, a lot of women who would like to get an MR face barriers to obtaining one; many of them resort to unsafe abortion as a result. Because induced abortions are highly legally restricted in Bangladesh, they are often practiced clandestinely in unhygienic settings, performed by untrained providers, or both. By averting unsafe abortions and their associated health complications, MRs could have a positive impact on women’s health and survival.
This issue brief examines the relationship between MR, unsafe abortion, and maternal mortality and morbidity in Bangladesh. Given the size and scope of the MR program, it makes sense to assess the relationship between MRs and unsafe abortions, at both the national and division levels. From existing data on maternal mortality, we also try to determine whether MRs have contributed to maternal health and survival. In addition, we discuss new findings on barriers to the provision of MR services in Bangladesh.
Incidence of MR
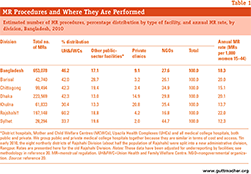
view fullsizeObtaining a current, accurate picture of the incidence of MRs in Bangladesh is important but challenging. Although MRs are officially authorized, efforts to systematically collect data on this service suffer from high levels of underreporting.15 Not surprisingly, for example, there are no records of procedures provided outside of official facilities—or of those that are performed in proper facilities but do not conform to government criteria regarding timing or the training of personel.16–19 Moreover, the last time the incidence of MRs was estimated at the national level was in 1995. To assess the incidence of these procedures as of 2010, we surveyed a nationally representative sample of 670 public and private facilities and collected incidence and related data (e.g., capacity to provide MR and indicators of access and barriers to provision; see Methods box). Records of MRs performed by the major nongovernmental organizations (NGOs) involved in the MR program† were also compiled from records supplied by their head offices.
Overall, health facilities in Bangladesh (including NGOs) performed an estimated 653,000 MR procedures in 2010, which translates into a rate of 18 MRs per 1,000 women aged 15–44 years (Table 1).*20 This rate is identical to the 18 MRs per 1,000 estimated in the mid-1990s.21 The absolute number of procedures, on the other hand, increased by 39%, largely because of growth in the population of women of reproductive age. However, different methodologies were used to estimate incidence, so trends should be interpreted with caution.
Nationwide, two-thirds (67%) of all facilities that are potential providers of MR excluding UH&FWCs had both functional MVA equipment and a staff member trained in MVA, the procedure generally used for MR (Table 2).22 Yet only 48% actually provided MRs in 2010. Moreover, the gap between being able to provide MRs and actually doing so is especially wide among private-sector clinics: Only about one-third of these facilities provided MRs in 2010, even though 60% have both the equipment and trained staff to do so. On the other hand, there is virtually no difference in capacity and actual performance in public-sector Mother and Child Welfare Centres (MCWCs) and Upazila Health Complexes (UHCs), as the same much-higher-than-average proportion (86–87%) were both capable of providing MRs and did so in 2010.
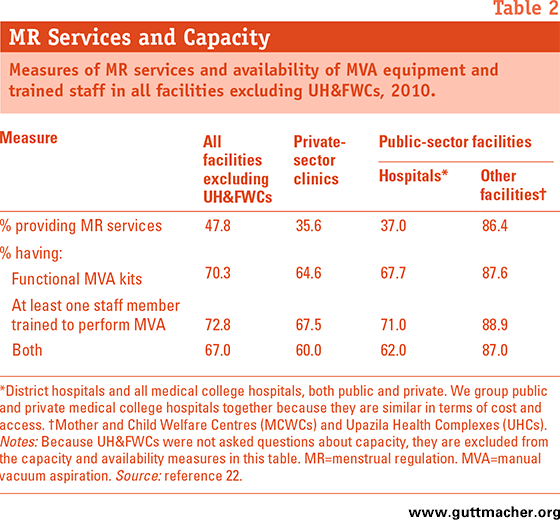
When we look at the specific types of facilities, all MCWCs provided the service, as did 83% of UHCs (not shown); both these facility types are staffed by doctors, nurses and paramedics. However, only about two-thirds of UH&FWCs—small public clinics staffed by FWVs, who are envisioned as the backbone of the MR program—provided MRs. Once we include these clinics, the proportion of all facilities providing MRs rises to 57%, and among all public sector facilities it is 66%.
Methods
This report draws on several data sources. Data on both MRs and unsafe induced abortions were collected through a study conducted by the Association for Prevention of Septic Abortion, Bangladesh (BAPSA) and the Guttmacher Institute. The study design and protocols were adapted to the specific situation in Bangladesh from a widely used methodology to indirectly estimate abortion incidence, the Abortion Incidence Complications Methodology (AICM). The study gathered data through two main sources and a few other ancillary sources, described below.
• Health Facilities Survey. We collected information on the number of MRs provided and the number of women treated for complications of unsafe abortion through a nationally representative survey of 670 public- and private-sector health facilities. Data on other variables, including quality of care, were also collected. The survey was fielded in May through November of 2010.
• MR service data from NGOs. As NGO facilities account for a large number of MR procedures and, to a lesser extent, postabortion care cases, we compiled data from the head offices of all the major NGOs that provide MR or postabortion care in Bangladesh. Each provided data, at the division level, on the number of MR procedures performed and the number of women treated for abortion complications in 2010 at all of their facilities.
• Other data sources. We relied on data from several Bangladesh Demographic and Health Surveys, including those conducted in 1999–2000, 2007 and 2011. We also used data from the 2010 Household Income and Expenditure Survey, which provides information on household and per capita income, and from the 2001 and 2010 BMMS, which provide information on maternal mortality and its causes in Bangladesh. The report also draws on the existing body of prior research carried out in Bangladesh.
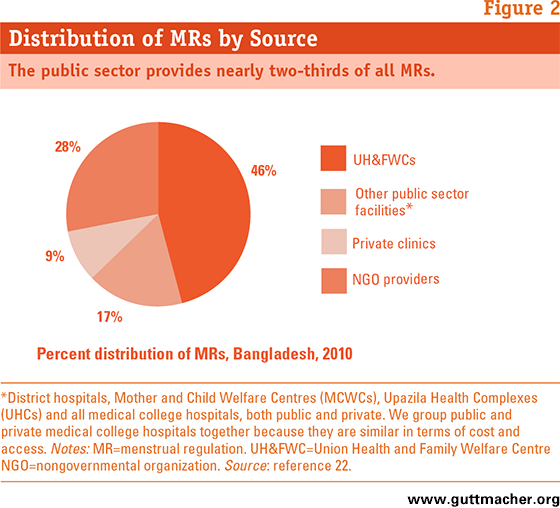
In terms of the sources of the country’s MRs, almost two-thirds are provided by the public sector (Figure 2). Making up this 63% are the most common single source, UH&FWCs (accounting for 46%), and other public-sector facilities such as district hospitals, MCWCs, UHCs and medical college hospitals (providing another 17%). Twenty-eight percent of MRs are obtained from NGO clinics and the remaining 9% from private clinics. The proportion of all MRs that each type of facility provides varies widely by administrative division (six at the time of the study but now seven; Table 1), likely reflecting variations in the availability of and access to UH&FWCs and the extent to which NGOs are actively working to increase access in underserved areas.
Possible impact of MRs on trends in abortion-related mortality
Given the widespread use of MRs—and the large increase in the absolute numbers of procedures in recent years—an important policy question is whether MR has helped to reduce maternal mortality in Bangladesh. We can infer the procedure’s impact on maternal deaths by assessing the extent to which it averts unsafe abortions. The available data suggest that sustained declines in abortion-related deaths were an important driver of the decline in maternal mortality over the past few decades.
For example, during the 1970s and 1980s, before the widespread availability of MR, unsafe abortion was a major cause of maternal mortality in Bangladesh. A 1978–1979 study conducted in nearly 800 facilities throughout the country found that complications from unsafe abortion played a role in 26% of maternal deaths.23 The next most recent national-level estimates of abortion’s role in maternal mortality date from 1998–2001, the reference period for the first of the country’s two maternal mortality studies— the 2001 BMMS.4 That assessment indicated that just 5% of maternal deaths were related to induced abortion, a considerable decline from the 26% measured in 1978–1979—even though the latter study used a different, less rigorous methodology than was previously used. The 2010 BMMS shows a further drop in the proportion of maternal deaths related to abortion, to just 1% in 2008–2010.5 Of course, given that all surveys of maternal mortality—and of abortion-related mortality in particular—suffer from recall bias and high levels of under-reporting,3 these results should be interpreted with caution.
Despite this uncertainty, however, the large relative decline in abortion-related maternal deaths from 1978–1979 to 1998–2001 is likely indicative of real change. To what extent could MR have played a role? The 2001 BMMS notes anecdotal evidence supporting the "dramatic decline" in deaths from incomplete and septic abortion as "presumably due to the expanded provision of safer and more accessible MR services."4
The availability of longitudinal data from the well-studied Matlab area allows us to examine trends in abortion-related mortality, albeit not at the national level. The Matlab Demographic Surveillance System has been tracking the annual numbers of MRs and clandestine abortions since 1989 (with the exception of 2001) in both an area that receives enhanced family planning services and a comparison area that does not.24 These data allow us to chart the relationship of MRs to clandestine abortions over time in the comparison area, which does not receive enhanced family planning services and thus is the more likely of the two areas to be representative (or the "best estimate"10) of the country as a whole.
According to data for the Matlab comparison area, the ratio of clandestine abortions to MRs was roughly two to one in 1989.24 By 2008, however, for every clandestine abortion there were five MRs. This important increase in MRs relative to clandestine abortions over the years is likely contributing to the sustained declines in abortion-related maternal mortality in the same area: The proportion of maternal deaths related to induced abortion in the comparison Matlab area fell from 16% in 1986–1990 to 9% in 2001–2005.16,25,26
Even if the slightly different time periods prevent us from lining up the decline in abortion-related mortality to the increase in the ratio of MRs to clandestine abortions mentioned in the previous paragraph, the trends are robust enough to show a clear impact of MRs on declining mortality. Indeed, another study conducted in Matlab arrived at similar conclusions.27 That study cited as evidence of MR’s role in averting abortion-related deaths the paradoxical decline in the rate of abortion-related mortality even as the ratio of abortions (defined as both MRs and induced abortions) to live births increased over roughly the same period.
Persistence of unsafe abortion
Despite the documented decline in abortion-related maternal mortality and a decrease in the most dangerous methods of clandestinely inducing abortion, unsafe abortion remains widespread. Even if unsafe abortions do not result in death, they can cause injury and suffering that can have lifelong consequences. Unfortunately, morbidity from unsafe abortion remains common, despite the availability of safe MR services. As of 2010, Bangladeshi women risked their health by having clandestine abortions at a rate of 18 per 1,000 women each year.20 In that same year, an estimated 231,000 women received treatment at a health facility for complications of unsafe abortion. Moreover, according to the perceptions of respondents to our survey of health professionals in 2010 (see methodology in reference 20), only about 40% of all women who needed treatment for abortion complications actually received it. This means that an additional 341,000 women developed complications but did not obtain care, indicating that all told, an estimated 572,000 Bangladeshi women suffered complications from unsafe abortions in 2010.
That MRs are relatively safe, compared with unsafe abortions, is clear when we compare their outcomes. For example, the rate at which MR complications are treated in a health facility is just one-third that of clandestine abortion complications (2.2 vs. 6.5 cases treated per 1,000 women aged 15–44 years; Table 3). Moreover, whereas for every 1,000 MRs that are performed each year, roughly 120 result in complications that are treated in health facilities, the comparable ratio for clandestine abortions is about 360 per 1,000 abortions.
In addition to the health consequences of clandestine abortions, their monetary costs are also substantial. Experts interviewed in the 2010 Health Professionals Survey estimated that in rural areas, the safest clandestine abortions—those provided by medical doctors—cost 500–1,100 taka.28 To put this financial burden into perspective, the average monthly per capita income in rural regions of Bangladesh is roughly 2,000 taka.29 Prices for clandestine abortions are estimated to be even higher in urban areas, with a physician-provided abortion costing 900–2,100 taka in areas where the average monthly per capita income is 3,741 taka.29
Overcoming barriers to MR
Why do Bangladeshi women continue to unnecessarily risk their health and life by having a clandestine abortion when safe and affordable MR procedures are available? Below we examine some of the obstacles women may encounter when trying to obtain an MR. We also look at constraints within the program that may be limiting women’s access to, and timely use of, the service.
Limited provision
One-third of facilities that are potential providers of MR services cannot offer them because they lack either the basic equipment or trained staff, or both (Table 2). Perhaps even more troubling, many facilities that do have adequately trained staff and the requisite equipment are still not offering this government-sanctioned service. The persistence of such gaps greatly reduces women’s access, and gaps are especially wide in private-sector clinics.
The reasons behind this untapped potential were hinted at in the responses to a supplemental question asked of UH&FWCs only. Among staff surveyed at UH&FWCs that did not offer MR services, 43% cited religious or social reasons for not doing so, 37% mentioned that beliefs related to their own health prevent them from offering the service, and 24% simply said they do not like to perform the procedure. In addition, roughly 10% each pointed to inadequate MR training, insufficient MR supplies, lack of space and the absence of support staff. That roughly four in 10 FWCs—the facility type providing the highest percentage of all MRs—cited "social or religious" reasons or personal preference for not offering MRs is an important indication of the need to better understand and then directly address these reasons.
Rejection by MR providers
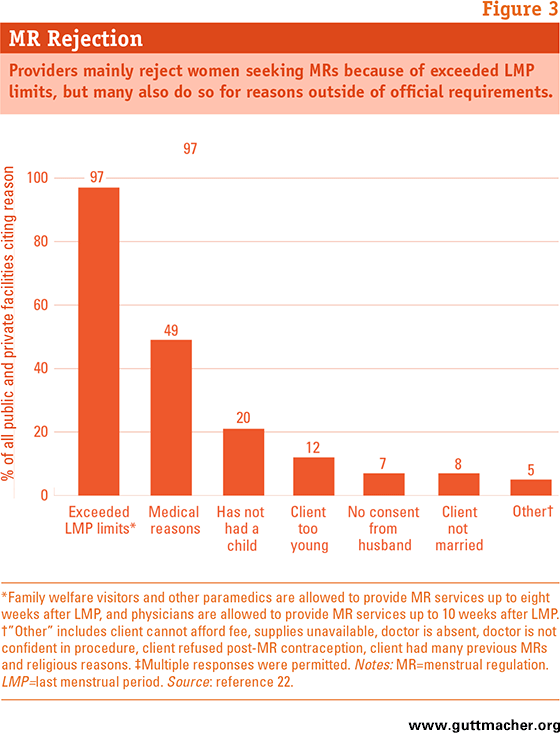
Many women are unable to obtain an MR because they are turned away for one. Our study found that more than one-quarter of all clients requesting an MR, or 166,000 women, were denied the procedure in 2010.20 When facilities were asked why they rejected requests for MRs, nearly all said that one of their reasons for doing so was because women were above the maximum permitted weeks since their LMP (Figure 3 ). This reason is understandable given regulations on LMP limits. Similarly, medical reasons (i.e., a client’s preexisting medical condition), cited by roughly half of facilities, may be understandable as well, although specifics are unavailable. Unfortunately, several other reasons for turning away MR clients, though cited by smaller proportions of facilities, are culture based and thus go beyond any guidelines or requirements. These include a woman not yet having any children (cited by 20%) and considering a woman to be too young (by 12%).
view fullsize
Poor quality of care
Despite the relative safety of the procedure, many MRs—78,000 in 2010—still lead to complications (Table 3), probably because of systemic flaws in MR service provision. Studies have found a number of shortcomings, including improper MVA technique, lack of sterilization of MVA equipment, unhygienic conditions, nonuse of pain relief during procedures and use of a single MVA syringe more than the recommended number of times.18,19
In addition, according to a nationwide 2002 assessment of the government’s MR program, unofficial payments are commonly made for a service that is supposed to be free.19 Indeed, in one of the few studies that collected information on payments for MR services (from the mid-1990s), one-third of the women who had an MR paid their provider, with the amount averaging 44 taka.30 Such charges—whose amounts are unknown until the woman arrives at a clinic—can be an important deterrent to getting needed services.18 In addition, evidence suggests that illicit brokers prey on women who have been rejected for an MR to steer them, for a fee, to unofficial providers who arbitrarily set a price according to such factors as weeks since their LMP and "adding" pain relievers to the procedure.16
Women’s limited knowledge
The MR program’s reach is constrained by the extent to which women know about it. As of 2007, nearly one-fifth of married Bangladeshi women had still never heard of MR;9 this proportion is higher among the least-educated and the poorest women (25–26%), compared with the most educated and the richest women (8–11%).31 Furthermore, very little is known regarding unmarried women’s knowledge about MR; these women have the most to lose should they become pregnant, given strong taboos against sex and childbearing outside of marriage.6
The information that many women do have is often inaccurate. Qualitative research from the mid-1990s demonstrates widespread confusion about the distinction between safe MR services and clandestine abortions.32 A 2012 qualitative study found that, even now, many women do not understand the difference between trained and untrained providers,18 which is unsurprising given the wide range of people providing MRs. For women who want to keep their MR a secret, nonmedical facility staff, including ayahs (female domestic workers), are often a preferred option because they perform the procedure discreetly after hours in the facility, or in their or the woman’s home. These nonprofessionals use MVA but are not properly trained in the technique, so their procedures have a high likelihood of complications, which is further increased by the unhygienic settings in which the procedures are often carried out.
Recommendations
Although much needs to be done to improve maternal health in Bangladesh—including making childbirth safer by increasing the number and proportion of deliveries attended by skilled personnel and expanding emergency obstetric services—more widespread use of the existing MR program has the potential to avert unsafe abortions and thus further reduce maternal morbidity and mortality. Below we offer a few strategies to achieve wider use of MR.
Educate women about MR’s availability
Given that the MR program has been in place for three decades, detailed knowledge about the service should be nearly universal by now. That many women are unable to clearly distinguish MR from unsafe abortion18 is indicative of the need for better information, especially since missing the opportunity for an MR can lead directly to having an unsafe abortion, which presents far higher health and monetary costs to women. The dangers of unsafe abortion need to be publicized so women clearly understand that an authorized, safe alternative is officially available and that it is free of charge. Efforts to engage fieldworkers who are already visiting households or community clinics33 to disseminate information about MR may prove effective, especially for reaching illiterate women and those who live in rural areas.34 FWVs’ encouraging women who have already had an MR to talk about their experience with others is another potentially effective strategy.30
Increase availability of MR services
Overall, 43% of the nation’s facilities that could potentially offer MR services did not provide them in 2010. MR services need to be made more widely available, especially in facilities that provide primary care and are most accessible to women living in rural communities, who likely live far from hospitals. Indeed, the finding that one-third of rural-based UH&FWCs were not even providing the service in 2010 is potentially troubling, given the program’s emphasis on their staff (FWVs) as essential MR providers. The country only recently reinitiated efforts to recruit new FWVs.10 Because many of these new recruits may lack confidence in their MR skills, on-site mentoring could be combined with supportive supervision to expand the number of competent providers of the procedure. Improved availability of MRs not only would benefit women’s health, but also would save money: In 2008, the hospital per-case cost of providing an MR was 27–40% of the hospital cost of treating moderate abortion complications, and 13% of the hospital per-case cost of treating severe abortion complications.17
Improve the quality of MR care
The level of complications from MR procedures suggests a great need to improve their safety. One avenue currently being studied is to offer MR performed with medication (mifepristone plus misoprostol), which is less invasive than MVA. A recent study showed that NGOs using this method found it to be acceptable and feasible in Bangladesh.35
To the extent that MRs are primarily still conducted using MVA, many shortcomings have been reported, the foremost being that one-third of the country’s facilities lack the equipment and staff trained to use it. Further problems cited in the literature include the inappropriate use of MVA equipment, repeated use of syringes meant to be discarded after 50 uses, and failure to adhere to proper equipment sterilization practices.16,18,19
Standards of patient care also were shown to be weak. Having to pay unauthorized fees can make MRs unaffordable to women—many of whom go on to have an unsafe abortion. This practice is especially egregious given that MR is supposed to be a free government service. Other aspects of poor care include inadequate pain relief, lack of privacy and being subjected to providers’ judgmental and punitive attitudes. To avoid these resolvable problems, increased supervision is needed along with improved basic training and repeat refresher training. Much of the inappropriate provider behavior and poor clinical practices could be addressed if the MR guidelines currently being developed by the government36 were to be finalized and broadly implemented.
Conclusions
Of course, the most direct way to safeguard women’s health and lower the number of unsafe abortions is to prevent unintended pregnancies. Bangladesh has made considerable progress in increasing use of modern contraceptive methods: Some 52% of married women currently use a modern method, according to the 2011 Demographic and Health Survey,33 whereas that proportion was 43% just one decade earlier.37 To enable Bangladeshi women to avoid becoming pregnant when they do not want to be, the current 12% who have an unmet need for contraception, plus the 9% who use less reliable traditional methods, must be able to choose freely from a wide range of effective methods. Further, evidence suggests that many of the unintended pregnancies in the country result from discontinuing method use because of side effects.18 This implies that providers need to both facilitate method-switching should women become dissatisfied with their current method and improve the quality of counseling on consistent and correct use. In addition, as part of comprehensive reproductive health care, contraceptive methods and counseling should be offered to women when they come into the system for postpartum visits, postabortion care and MR services.
The better able Bangladeshi women are to avoid unintended pregnancy and the need to resort to unsafe abortion, the lower the burden of abortion-related maternal illness and death. Making safe MRs more widely accessible will further reduce complications related to unsafe MRs and avert unsafe abortions and their negative impact on women’s health.
REFERENCES
1. United Nations, 2015 Millennium Development Goals: a gateway to the UN system’s work on the MDGs, no date, <http://www.un.org/millenniumgoals/>, accessed Apr. 4, 2012.
2. Institute for Health Metrics and Evaluation (IHME), Maternal mortality estimates and MDG 5 attainment by country, 1990–2011, Sept. 23, 2011, <http://www.healthmetricsandevaluation.org/ghdx/record/maternal-mortalit… -mdg-5-attainment-country-1990-2011>, accessed Apr. 21, 2012.
3. World Health Organization (WHO) et al., Trends in Maternal Mortality: 1990 to 2010, WHO, UNICEF, UNFPA and the World Bank Estimates, Geneva: WHO, 2012.
4. National Institute of Population Research and Training (NIPORT) et al., Bangladesh Maternal Health Services and Mortality Survey 2001, Dhaka, Bangladesh: NIPORT; and Calverton, MD, USA: ORC Macro, 2003.
5. NIPORT, Bangladesh Maternal Mortality and Health Care Survey 2010, Summary of Key Findings and Implications, Dhaka, Bangladesh: NIPORT, 2011.
6. Akhter H, Abortion in Bangladesh, in: Sachdev P, ed., International Handbook on Abortion, New York: Greenwood Press, 1988.
7. Penal Code, 1860, as adopted by the Bangladesh Laws Revision and Declaration Act of 1973.
8. Government of the People’s Republic of Bangladesh, Memo No. 5-14/MCH-FP/Trg.79, Dhaka, Bangladesh: Population Control and Family Planning Division, 1979.
9. NIPORT, Mitra and Associates and Macro International, Bangladesh Demographic and Health Survey, 2007, Dhaka, Bangladesh: NIPORT and Mitra and Associates; and Calverton, MD, USA: Macro International, 2009.
10. Johnston H et al., Scaled up and marginalized: a review of Bangladesh’s menstrual regulation programme and its impact, in: Blas E, Sommerfeld J and Karup A, eds., Social Determinants Approaches to Public Health: From Concept to Practice, Geneva: WHO, 2011, pp. 9–24.
11 Department of Economic and Social Affairs, United Nations, World Urbanization Prospects, the 2011 revision, no date, <http://esa.un.org/unpd/wup/CD-ROM/Urban-Rural-Population.htm>, accessed Apr. 10, 2012.
12. Mridha M, Anwar I and Koblinsky M, Public-sector maternal health programmes and services for rural Bangladesh, Journal of Health, Population and Nutrition, 2009, 27(2):124–138.
13. 4200 FWAs, FWVs to be recruited to safe motherhood programme, The Financial Express, July 1, 2012, <http://www.thefinancialexpress-bd.com/more.php?date=2012-07-01&news_id=135072>, accessed July 13, 2012.
14. MR services: performance statistics, in: Health and Rights, Dhaka: Bangladesh, Sexual and Reproductive Health and Rights (SRHR) Consortium, No. 4, Issue 4, 2011, p. 4.
15. Bangladesh Association for the Prevention of Septic Abortion (BAPSA), M.R. training and services status, M.R. Newsletter: Working Together to Improve Women’s Lives, Dhaka, Bangladesh: BAPSA, Twenty-first year, No. 2, 2005, p. 3.
16. Oliveras E et al., Situation Analysis of Unsafe Abortion and Menstrual Regulation in Bangladesh, Dhaka, Bangladesh: International Centre for Diarrhoeal Disease Research, Bangladesh (ICDDR,B), 2008.
17. Johnston H et al., Health system costs of menstrual regulation and care for abortion complications in Bangladesh, International Perspectives on Sexual and Reproductive Health, 2010, 36(4):197–204.
18. Hashemi A, Rashid S and Rashid M, Where do women go and why? Understanding the barriers to safe MR services in Bangladesh, unpublished manuscript, Dhaka, Bangladesh: James P. Grant School of Public Health, BRAC University, 2012.
19. Chowdhury SN and Moni D, A situation analysis of the menstrual regulation programme in Bangladesh, Reproductive Health Matters, 2004, 12(24 Suppl.):95–104.
20. Singh S et al., The incidence of menstrual regulation procedures and abortion in Bangladesh, International Perspectives on Sexual and Reproductive Health, 2012 (forthcoming).
21. Singh S et al., Estimating the level of abortion in the Philippines and Bangladesh, International Family Planning Perspectives, 1997, 23(3):100–107 & 144.
22. Unpublished data from the Health Facilities Survey, Bangladesh, 2010.
23. Rochat RW et al., Maternal and abortion related deaths in Bangladesh, 1978–1979, International Journal of Gynaecology & Obstetrics, 1981, 19(2):155–164.
24. DaVanzo J and Rahman M, Safe vs. unsafe pregnancy termination in Matlab Bangladesh: trends and correlates, paper presented at the annual meeting of the Population Association of America, San Francisco, CA, USA, May 3–5, 2012.
25. Chowdhury ME et al., Determinants of reduction in maternal mortality in Matlab, Bangladesh: a 30-year cohort study, Lancet, 2007, 370(9595):1320–1328.
26. Chowdhury ME et al., Causes of maternal mortality decline in Matlab, Bangladesh, Journal of Health, Population and Nutrition, 2009, 27(2):108–123.
27. ICDDR,B, Increasing levels of abortion and decreasing abortion-related mortality, Health and Science Bulletin, 2007, 9(2):1–6.
28. Unpublished data from the Health Professionals Survey, Bangladesh, 2010.
29. Bangladesh Bureau of Statistics (BBS), Report of the Household Income and Expenditure Survey, 2010, Dhaka, Bangladesh: BBS, 2012.
30. Akhter H et al., A Study to Assess the Determinants and Consequences of Abortion in Bangladesh, Dhaka, Bangladesh: Development Assistance Council and Bangladesh Institute of Research for Promotion of Essential & Reproductive Health and Technologies (BIRPERHT), 1998.
31. Special tabulations of data from the 2007 Bangladesh Demographic and Health Survey.
32. Caldwell B et al., Pregnancy termination in a rural subdistrict of Bangladesh: a microstudy, International Family Planning Perspectives, 1999, 25(1):34–37 & 43.
33. NIPORT, Mitra and Associates, and Measure DHS, ICF International, Bangladesh Demographic and Health Survey, 2011: Preliminary Report, Dhaka, Bangladesh: NIPORT and Mitra and Associates; and Calverton, MD, USA: Measure DHS, 2012.
34. Islam M, Rob U and Chakraborty N, Menstrual regulation practices in Bangladesh: an unrecognized form of contraception, Asia-Pacific Population Journal, 2004, 19(4): 75–99.
35. ICDDR,B and Maternal Health Task Force, Menstrual Regulation Using Medication Is Acceptable and Feasible in NGO Settings in Bangladesh, Dhaka, Bangladesh: Center for Reproductive Health, 2011.
36. Bhuiyan HU, BAPSA, Dhaka, Bangladesh, personal communication, July 13, 2012.
37. NIPORT, Mitra and Associates, and ORC Macro, Bangladesh Demographic and Health Survey, 1999–2000, Dhaka, Bangladesh: NIPORT and Mitra and Associates; and Calverton, MD, USA: ORC Macro, 2001.
CREDITS
This In Brief was written by Altaf Hossain, Association for Prevention of Septic Abortion, Bangladesh (BAPSA); Isaac Maddow-Zimet and Susheela Singh, both of the Guttmacher Institute; and Lisa Remez, independent consultant. It was edited by Susan London, independent consultant. The authors are grateful for comments on drafts provided by Saifuddin Ahmed, Johns Hopkins Bloomberg School of Public Health; Ahmed Al-Sabir, freelance consultant and former director of research, NIPORT; Ferdousi Begum, Associate Professor of Obstetrics and Gynecology and former secretary general, Obstetrical and Gynaecological Society of Bangladesh; Halida Hanum Akhter and Elizabeth Oliveras, both at Pathfinder International; Mohammed Sharif, Director, Maternal and Child Health Services and Line Director, Maternal, Child, Reproductive and Adolescent Health (MCRAH); Heidi Bart Johnston, Swiss Tropical and Public Health Institute and University of Basel; Reena Yasmin, Marie Stopes Bangladesh;
*The name of this survey has changed over time. In 2001, it was Bangladesh Maternal Health Services and Mortality Survey; in 2010, it was Bangladesh Maternal Mortality and Health Care Survey. However, the acronym has remained the same.
† The major NGOs in 2010 were the Reproductive Health Services Training and Education Program (RHSTEP), Association for Prevention of Septic Abortion, Bangladesh (BAPSA), the Bangladesh Women’s Health Coalition (BWHC), the Family Planning Association of Bangladesh (FPAB), the Urban Primary Health Care Project (UPHCP), Marie Stopes Bangladesh and BRAC Bangladesh.
Suggested Citation
Suggested citation: Hossain A et al., Menstrual regulation, unsafe abortion and maternal health in Bangladesh, In Brief, New York: Guttmacher Institute, 2012, No. 3.
