Over the last decade, Medicaid has undergone a metamorphosis from a program based on traditional fee-for-service payment to one dominated by managed care (see chart). Because Medicaid is the leading source of public funding for family planning services in the United States—in 1994, the most recent year for which data are available, it contributed nearly half of all public dollars spent on the delivery of family planning services and supplies—understanding and monitoring this transition is of the utmost importance to family planning supporters.
| Medicaid Managed Care |
|---|
| The percentage of Medicaid beneficiaries enrolled in managed care plans has skyrocketed in recent years. |
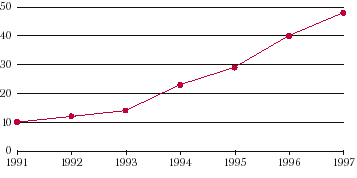 |
| Source: Kaiser Commission on Medicaid and the Uninsured. |
Originally enacted in 1965, Medicaid is a joint federal-state program under which the federal government sets broad program parameters—such as requiring that states provide a minimum package of mandated services, including family planning—while the individual states have control over program administration. Historically, states wishing to require Medicaid enrollees to obtain their care through managed care systems—a "violation" of one of the program's fundamental original premises, that recipients should be able to obtain medical care from a provider of their choice—needed to obtain special permission from the Department of Health and Human Services' Health Care Financing Administration (HCFA). This "waiver" process allowed HCFA to set independent requirements for each state's effort.
Recognizing that managed care over time had become a permanent part of most states' Medicaid programs, Congress, as part of the 1997 Balanced Budget Act, freed states from the need to obtain federal waivers. In return for this increased latitude, however, states would be required to adhere to uniform minimum national standards for Medicaid managed care. In September 1998, HCFA published proposed federal regulations to implement these uniform standards. Public input on the rule was solicited throughout the fall, and the agency is now making final policy decisions.
The Regulations
The proposed regulations address a range of issues with important implications for access to family planning services.
Freedom of Choice and Direct Access
Because some individual providers, and even some entire managed care plans, may not be willing to provide family planning, Congress since the mid-1980s has placed special requirements on most state managed care programs operating under federal waivers. These programs have been required to allow all Medicaid recipients to obtain family planning services from the provider of their choice, even if that provider is not affiliated with their managed care plan.
Although the Balanced Budget Act did away with the necessity for states to obtain waivers, it retained the provision allowing enrollees freedom of choice for family planning. This guarantee is reiterated in the proposed regulations; according to HCFA, the statute allows states to require that enrollees obtain all their care within their managed care plans, "but not with respect to family planning services."
The proposed rule is less clear, however, on a related issue aimed at giving enrollees the easiest access to providers within their plan's network. Here the question is whether enrollees will have "direct access"—that is, without having to first obtain a referral from a primary care provider—to in-plan family planning services. The proposed rule does guarantee enrollees some direct access, and it is expansive in describing the providers to whom a woman may have direct access (explicitly included are certified nurse midwives as well as gynecologists). However, it leaves undefined the types of care that are available on a direct-access basis, using only the vague phrase "routine and preventive health services." In order to ensure that enrollees have unimpeded access within their plans, it is important that the final rule clearly includes family planning services under this rubric.
Cost-Sharing
Family planning is one of the handful of health care services for which the Medicaid statute has long prohibited the imposition of any cost-sharing requirements, whether in the form of copayments or deductibles. While the Balanced Budget Act eliminated a long-standing prohibition on fees for other services obtained through managed care plans, it retained the prohibition on cost-sharing for family planning—a prohibition that is restated in the proposed rule.
This explicit statement is particularly important in light of the recent findings by The Alan Guttmacher Institute (AGI) that some Medicaid managed care plans are charging fees for family planning services, notwithstanding the clear federal ban on the practice (see box).
Family Planning Access in Managed Care Plans
A recent study by The Alan Guttmacher Institute examined access to family planning services in both commercial and Medicaid managed care plans in all or part of five states: California, Colorado, Florida, Massachusetts and Michigan.
Among the most significant findings of the study are the following:
• While more than one in four commercial plans did not cover the full range of FDA-approved contraceptive methods—and some covered no methods at all—Medicaid plans almost uniformly provided comprehensive contraceptive coverage. This is hardly surprising, considering that the federal Medicaid statute has long mandated coverage of family planning services and supplies.
• Despite a statutory prohibition on the imposition of any fees for family planning, almost one in 10 Medicaid managed care enrollees reported having been charged for contraceptive services, and two of the 27 plans surveyed themselves reported charging fees.
• Only one-half of the commercial plans and one-third of the Medicaid plans provided enrollees with a list of covered contraceptive methods. Not surprisingly, therefore, seven in 10 women enrolled in both Medicaid and commercial plans reported that they did not receive written information about their plan's contraceptive coverage. Among Medicaid enrollees, 17% did not know whether their plan covered oral contraceptives, and between 43% and 60% were unsure about other methods.
• Almost one in three women enrolled in both commercial and Medicaid managed care reported difficulties obtaining covered contraceptive services. However, while the most commonly reported problem among commercial enrollees was a long wait for an appointment (up to four weeks), among Medicaid enrollees it was not being allowed to choose a contraceptive services provider, even though provider choice is important to them.
Informing Enrollees
As a way to empower managed care enrollees, the Balanced Budget Act requires that enrollees be fully informed of their rights as Medicaid recipients. To implement that provision, the proposed regulations require managed care plans to provide detailed information upon enrollment and, upon request, annually thereafter. This requirement includes information on the benefits available, procedures for obtaining services, any restrictions on the enrollee's freedom of choice among network providers, policies for referrals for specialty care and for other services not furnished by the enrollee's primary care provider and the extent to which enrollees may obtain services from out-of-network providers.
The recent AGI managed care study highlights the importance of requiring plans to provide this type of information: The study found that many plans do not provide information on their contraceptive coverage and that many enrollees seem to be unaware of their plan's coverage (see box).
Conscience Provisions
The Balanced Budget Act contained an extremely troubling provision allowing an entire Medicaid managed care plan, based on a religious or moral objection, to refuse to "provide, reimburse for, or provide coverage of a counseling or referral service." The proposed rule sets forth how such a restriction could be put into practice, and how such a limitation may co-exist with the legal entitlement of Medicaid enrollees to all Medicaid-covered services, including those to which an individual managed care plan may object.
In general, the proposed rule draws an important distinction between the right of an individual health care provider to provide patients with full and accurate information and the ability of a plan to refuse to pay for counseling. The preamble states, "While the new law precludes MCOs [managed care organizations] from interfering with enrollee-practitioner communications, it does not require MCOs to provide, reimburse for, or provide coverage of counseling or referral services for specific services, if the MCO objects to the service on moral or religious grounds." As a result, a plan may refuse to reimburse a provider for counseling services, but it may not prohibit the provider from actually providing the counseling.
Nonetheless, a restriction on payment—even if conversations between providers and patients are not themselves prohibited—is an obvious disincentive for providers, one that heightens the need for protections to ensure access to all Medicaid services for all enrollees. Such a framework is laid out in the proposed rule. The proposed regulations clearly gives state Medicaid agencies the obligation to ensure access to all covered services, either by including them in the contracts it signs with managed care plans, or through other means.
This is most easily accomplished for services that are covered under a plan's managed care contract. In this case, plans are obligated to demonstrate to states that they have adequate capacity—including an adequate provider network—to provide true access to the care. The problem is more complicated for services that are not included in an individual managed care contract—for example, if a plan refuses to provide family planning. In this case, the proposed regulations put the burden of ensuring access directly on the state: "The state must arrange for those services to be made available from other sources and instruct all enrollees on where and how to obtain them, including how transportation is provided."
Roadblocks Ahead
Assuming the regulations that ultimately are finalized closely resemble the regulations as proposed—and that several important details are addressed in the process—family planning services stand to fare well in this emerging Medicaid system. Whether that will be the case, of course, remains to be seen.
Ironically, the very clarity and detail with which the proposed regulations spell out the requirements for plans, and states, to ensure unfettered access to Medicaid-covered services may be their undoing. States had pushed for abandoning waivers in order to gain additional flexibility and the freedom to design their programs and to rid themselves of what they construed to be undue federal interference. Although Congress granted their wish and abolished the waiver requirement, in the process it established a strong set of protections for managed care enrollees; the proposed rule spells out how these protections are to be translated from legislative intent to actual practice.
Not surprisingly, some states are now alleging that the proposed regulations' requirements are too prescriptive and continue to deprive states of the flexibility they need. Thus far at least, the family planning-related provisions of the proposed rule are not at issue in this debate. However, if the concerns raised by the states lead HCFA to back down on some of the detail it built into the proposed rule, the accessibility of family planning services to Medicaid managed care enrollees—which at the moment looks so promising—could be seriously impaired.
