When hopes for large-scale health care reform were dashed in the early 1990s, Congress embarked on a series of more incremental—and, therefore, more politically feasible—moves to bring insurance coverage to at least some of the millions of Americans who lack it and to make existing coverage more comprehensive. Passage in 1997 of the State Children's Health Insurance Program (CHIP) was one of the boldest of these incremental moves. CHIP has at its disposal up to $40 billion in federal funds over 10 years to provide health coverage to many of the nation's estimated 12 million uninsured children and adolescents.
Although it was coverage of young children that provided the political momentum, CHIP is targeted at children up to age 19 in families with incomes below 200% of the federal poverty level. Included in that group are 1.3 million females and 1.4 million males—12% of all adolescents aged 13-18. According to the Guidelines for Adolescent Preventive Services issued by the American Medical Association (AMA), all of these adolescents need routine preventive care, including health guidance about sexual development and responsible sexual decisionmaking. At age 19, over three-fourths of females and 85% of males are sexually experienced; according to the AMA guidelines, sexually active teens also need screening for cervical cancer and sexually transmitted diseases, as well as access to family planning services and supplies.
Since the CHIP statute lays out broad outlines within which states may design and operate their own programs, states largely will determine the extent to which CHIP meets the reproductive health needs of enrolled adolescents. States determine age and income eligibility levels and often the benefits that will be provided.
According to a recent analysis by The Alan Guttmacher Institute (AGI) of the plans from all 50 states and the District of Columbia that have been approved by the Health Care Financing Administration (HCFA), 46 states plus the District of Columbia provide coverage to children up to age 19. Two states have lower age limits (16 years in Arkansas and 17 years in Oklahoma), but these states could still cover a significant number of adolescents. Two other states (Hawaii and Minnesota) cover only young children.
Twenty-eight states and the District of Columbia set an income ceiling between 151% and 200% of poverty (see table, page 8). Only 14 states cut off eligibility at 150% of poverty or below, while eight allow enrollees with incomes above 200% of poverty to qualify for coverage.
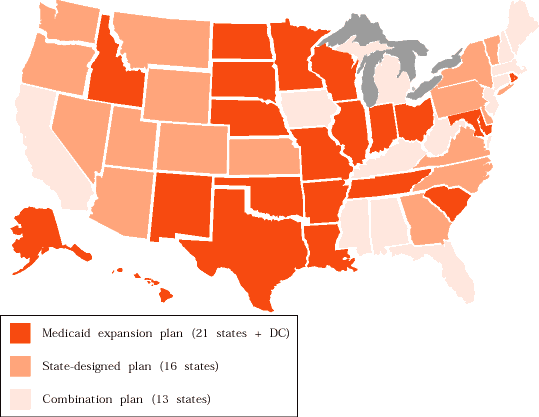
In addition, the federal statute allows states to determine overall program structure. Twenty-one states and the District of Columbia chose to expand eligibility for their Medicaid programs to cover children and adolescents eligible for CHIP. Sixteen states developed their own, separate programs. The 13 remaining states took a combination approach, typically providing Medicaid coverage to enrollees below a certain income level and state-designed (and often less-comprehensive) coverage to higher income enrollees (see map).
| How State CHIP Programs Are Structured |
 |
Coverage of Family Planning
The states' decisions on whether to expand Medicaid or create separate programs have important implications for the extent to which CHIP programs will offer covered adolescents access to family planning services and supplies. In the 22 jurisdictions with a Medicaid expansion, as well as in the Medicaid component of the 13 combination plans, enrollees are entitled to the full range of Medicaid-covered services, including maternity care and family planning services and supplies. (The federal Medicaid statute specifically mandates coverage of family planning services to "individuals of childbearing age," including "minors who can be considered to be sexually active.")
Medicaid offers other important protections to enrollees. Children enrolled in Medicaid—including those enrolled through CHIP—may not be made subject to any cost-sharing requirements, such as copayments or deductibles. (The statute also specifically prohibits cost-sharing for family planning services or supplies.) In addition, Medicaid recipients enrolled in managed care plans may obtain family planning services and supplies from the provider of their choice, even if that provider does not participate in their managed care network.
In contrast to the detailed requirements of Medicaid, states choosing to implement CHIP through a separate program have wide latitude to design their own benefit packages. The statute permits—but does not require—the package to include coverage of family planning services and supplies. Significantly, however, most of the states that have chosen to create an entirely state-designed CHIP program or a combination program with a state-designed component appear to be including coverage of family planning services.
Of the 29 states that have some state-designed component of their program, 16 specifically indicate in their plans that family planning services will be covered for enrolled adolescents, according to the AGI analysis (see table). Most of the remaining state-designed programs simply declare that the general category "prenatal care and prepregnancy family planning services" will be covered but do not provide any additional information on the coverage of either of these two services. The extent to which these state programs actually include a range of family planning services under that broad rubric is not known at this point. Only one state indicates that it does not intend to cover the general category.
All of the state-designed programs cover prescription drugs in general, and 16 states specify in their plans that prescription contraceptive drugs will be covered. Georgia prohibits coverage of all contraceptive devices, however, and Utah specifically excludes the contraceptive implant, Norplant.
The state plans do not provide information on whether enrollees will be required to pay a portion of the cost when obtaining family planning services. However, a recent study by the federal General Accounting Office (GAO) indicates that state-designed programs generally require cost-sharing in an attempt, according to the GAO, both to control utilization and to promote "personal responsibility" for enrollees and their families.
That so many of the state-designed programs appear to cover family planning services and supplies has important implications for CHIP's future. Many observers believe that state-designed programs are likely to dominate the CHIP landscape in the future because they accord states greater latitude to control both benefits and cost. GAO estimates that as many as 14 of the original Medicaid CHIP programs were really "placeholders," designed to allow states to get a program up and running quickly while developing a state-designed program for implementation later.
| Key Components of Approved State CHIP Plans | ||||
| State | Medicaid* | State-Designated Component | ||
| Income Ceiling | Income Ceiling | Inclusion of Family Planning Services | Inclusion of Contraceptive Drugs/Devices | |
| Alabama | 100% | 200% | Unspecified | Unspecified |
| Alaska | 200% | ----- | ----- | ----- |
| Arizona | ----- | 200% | Specified | Specified |
| Arkansas | 100% | ----- | ----- | ----- |
| California | 100% | 200% | Specified | Specified |
| Colorado | ----- | 185% | Unspecified | Specified |
| Connecticut | 185% | 300% | Specified | Specified |
| Delaware | ----- | 200% | Specified | Unspecified |
| District of Columbia | 200% | ----- | ----- | ----- |
| Florida | 100% | 200% | Unspecified | Unspecified |
| Georgia | ----- | 200% | Specified | Unspecified |
| Hawaii | 185% | ----- | ----- | ----- |
| Idaho | 150% | ----- | ----- | ----- |
| Illinois | 133% | ----- | ----- | ----- |
| Indiana | 150% | ----- | ----- | ----- |
| Iowa | 133% | 185% | Unspecified | Specified |
| Kansas | ----- | 200% | Specified | Unspecified |
| Kentucky | 100% | 200% | Specified | Specified |
| Louisiana | 150% | ----- | ----- | ----- |
| Maine | 150% | 185% | Unspecified | Unspecified |
| Maryland | 200% | ----- | ----- | ----- |
| Massachusetts | 150% | 200% | Specified | Specified |
| Michigan | 150% | 200% | Specified | Specified |
| Minnesota | 280% | ----- | ----- | ----- |
| Mississippi | 100% | 133% | Unspecified | Specified |
| Missouri | 200% | ----- | ----- | ----- |
| Montana | ----- | 150% | Specified | Specified |
| Nebraska | 185% | ----- | ----- | ----- |
| Nevada | ----- | 200% | Unspecified | Unspecified |
| New Hampshire | 300% | 300% | Unspecified | Specified |
| New Jersey | 133% | 350% | Specified | Specified |
| New Mexico | 235% | ----- | ----- | ----- |
| New York | ----- | 185% | Unspecified | Specified |
| North Carolina | ----- | 200% | Specified | Specified |
| North Dakota | 100% | ----- | ----- | ----- |
| Ohio | 150% | ----- | ----- | ----- |
| Oklahoma | 185% | ----- | ----- | ----- |
| Oregon | ----- | 170% | Specified | Unspecified |
| Pennsylvania | ----- | 200% | Not Covered§ | Unspecified |
| Rhode Island | 300% | ----- | ----- | ----- |
| South Carolina | 150% | ----- | ----- | ----- |
| South Dakota | 133% | ----- | ----- | ----- |
| Tennessee | 200% | ----- | ----- | ----- |
| Texas | 100% | ----- | ----- | ----- |
| Utah | ----- | 200% | Specified | Specified** |
| Vermont | ----- | 300% | Unspecified | Unspecified |
| Virginia | ----- | 185% | Specified | Unspecified |
| Washington | ----- | 250% | Unspecified | Unspecified |
| West Virginia | 150% | 150% | Unspecified | Specified |
| Wisconsin | 185% | ----- | ----- | ----- |
| Wyoming | ----- | 133% | Specified | Unspecified |
| *Medicaid enrollees are entitled to a benefit package that includes family planning services and supplies. Georgia specifically states that contraceptive devices are not covered. New Hampshire's income ceilings for both the Medicaid and state-designed components are 300%; Medicaid covers from birth to age one, and the state-designed component covers ages 1-18. §Pennsylvania does not cover the general category "prenatal and prepregnancy family planning." **Utah specifically excludes coverage for the contraceptive implant, Norplant. West Virginia's income ceilings for both the Medicaid and state-designed components are 150%; Medicaid covers ages 1-5, and the state-deigned component covers ages 6-18. | ||||
Outreach Efforts
Outreach has been an important aspect of CHIP from the very beginning. In fact, the authorizing statute requires state plans to include an outreach component. Outreach, however, is not a traditional activity for Medicaid and public welfare programs, which generally have viewed their role as being to limit services to those who meet rigorous eligibility criteria, rather than to reach out proactively so as to serve as many individuals as possible. "Outreach is a whole new concept for us, but one that is working and one that is helping Medicaid and CHIP," says Sally Richardson, the HCFA official who oversees both Medicaid and CHIP.
In addition, CHIP must overcome the stigma associated with its connection to Medicaid—eligibility for which until 1996 was linked to eligibility for welfare. The Medicaid-welfare connection also was a problem in the late 1980s, when Medicaid was expanded to cover pregnant women and infants in families with incomes above traditional Medicaid-income ceilings. This was the first time Medicaid aggressively moved to enroll a population that had no connection to welfare, and states found a widespread hesitancy on the part of individuals to enroll, because doing so often necessitated application in person at a welfare office. Some states responded with a range of innovative strategies designed to separate their Medicaid expansion programs from welfare—including the actual enrollment process—as much as possible.
Now facing similar issues with CHIP, states are taking steps to streamline the process to allow individuals to enroll in the program without having to apply at a welfare office. These include "presumptive eligibility," through which health care providers can grant provisional eligibility while a formal application is being processed, and "outstationing," through which eligibility workers who can make formal eligibility determinations are placed directly in health care sites. Many states also distribute applications widely and allow applicants to submit them by mail rather than in person.
States are moving to differentiate CHIP programs from Medicaid in other ways as well. For example, several states are using different names for their CHIP program, such as MIChild in Michigan or Healthy Kids in Florida. In addition, several states are using identification cards that more closely resemble private insurance cards than Medicaid cards.
Notably, however, the CHIP statute includes a cap on expenditures for outreach by states choosing to establish a state-designed program, rather than a Medicaid expansion. The statute limits the outreach funds that may be spent by these states to 10% of the total amount spent by the state on services. Unfortunately, this restricts outreach expenditures in the start-up phases of the program, just when these activities should be at their zenith. Such a cap is particularly ironic, in the view of many observers, since separate state-designed programs may be more attractive to potential enrollees because of the stigma associated with Medicaid-based efforts.
Next Steps
So far, at least, outreach efforts appear to have fallen short of their goals. During a press conference in late July, President Bill Clinton said he was "disappointed" that enrollment in CHIP is "a little slow." Commenting on recent data showing that program enrollment has recently reached the one million mark, Clinton said, "I would have thought by now we'd have almost three million...and we're well behind that."
A few days later, Clinton unveiled a multifaceted effort to boost CHIP enrollment. According to Clinton, the Department of Education is sending letters to school administrators nationwide asking that they take part in the effort. Educators are being asked to make CHIP enrollment part of the school registration process, distribute information at school functions and use applications for reduced-price school lunches to screen for CHIP enrollment. Other federal agencies are expected to become involved as well. The Department of Health and Human Services is developing a nationwide radio campaign to promote awareness of the program. And federal investigators will be sent to states to determine whether applicants have been unfairly denied coverage under CHIP—or Medicaid, enrollment in which has been falling since the enactment of welfare reform in 1996.
Beyond that, as the federal and state governments move to develop more extensive, and aggressive, outreach efforts around CHIP, it is vital that some outreach efforts be aimed at reaching the millions of uninsured adolescents who might be eligible. This could mean targeting printed materials to adolescents, making information available at places frequented by adolescents, conducting media campaigns aimed at adolescents and permitting eligibility determinations at service sites—such as family planning clinics—that see large numbers of young people. In addition, it means that materials developed for parents need to make clear that all their children—adolescents as well as younger children—finally may have a source of affordable insurance coverage.
