In early April, a coalition led by the American Public Health Association celebrated National Public Health Week by raising awareness about the epidemic of overweight and obesity in the United States. The next month, the Department of Health and Human Services (DHHS) announced a new program of community grants to prevent several chronic health conditions, such as those caused by smoking and poor diet. And in June, Senate Majority Leader Bill Frist (R-TN), with bipartisan support, introduced a bill—one of many similar measures introduced this session—that would authorize new grants for obesity prevention.
These efforts are examples of a growing awareness in the United States about how lifestyle changes can positively impact public health. The antiobesity message, while simmering for many years, has recently come to prominence, helped in part by a December 2001 "Call to Action" by former Surgeon General David Satcher, as well as by the efforts of his successor, Richard H. Carmona. It parallels, in many ways, the more established antismoking message, which has been pushed by U.S. surgeons general since the 1960s and which has contributed to dramatic declines in smoking rates.
Two Epidemics
Such campaigns are pursued because smoking and obesity are two of the leading causes of preventable mortality and morbidity in the United States. Both are risk factors for a large number of critical health problems, such as heart disease, stroke and cancer.
According to a 2001 surgeon general report on women and smoking, three million U.S. women have died prematurely from smoking-related disease since 1980, and lung cancer is now the leading cause of female cancer death (surpassing breast cancer). Similarly, Satcher's 2001 report on obesity associated that condition with diabetes, heart disease, stroke, hypertension, cancer and a number of other problems. In an April 2002 report by the Centers for Disease Control and Prevention (CDC), researchers estimated that smoking cost $158 billion per year in the late 1990s, including medical care costs and productivity losses. Similar numbers were cited by the surgeon general for obesity—$117 billion in 2000.
The impact of neither epidemic is likely to fade anytime soon. Incidence of smoking has declined significantly among American adults, but the decline has slowed considerably, and rates are still dangerously high. According to the National Center for Health Statistics (NCHS), the incidence of smoking has dropped from 42% of adults in 1965, to 25% in 1990 and 23% in 2000. Smoking among high school students peaked at 36% in 1997, but 29% still smoked in 2001.
In contrast to the smoking epidemic, obesity is a rapidly increasing problem. NCHS reports that 31% of U.S. adults were obese in 1999-2000, up from 13% in 1960-1962 and 23% in 1988-1994. Although weight problems are less common among children than among adults, the proportion of children who are overweight has more than tripled since the 1960s. [Overweight for adults is defined as body mass index (BMI) at or above 25; obese, at or above 30; age-specific standards are used for children. BMI is defined as weight (in kilograms) divided by the square of height (in meters).]
Rates of smoking and obesity are particularly high for certain demographic groups, according to data from the surgeon general reports and NCHS. Smoking rates are twice as high for young white women as for young black or Hispanic women. Smoking is nearly three times as common among women without a high school diploma as among women who completed college. Weight is particularly problematic among black women, half of whom are obese; it is also strongly related to income: One study found that women at or below 130% of the federal poverty level were about 50% more likely to be obese than women above that income.
Reproductive Health Impacts
Smoking and obesity have a wide range of effects specific to reproductive health. One or both can be negatively linked to everything from puberty to breastfeeding to cervical cancer. For reproductive health care providers, the three areas in which smoking and obesity may have the most directly relevant impacts are pregnancy outcomes, fertility and contraceptive choice.
In terms of the impact on pregnancy, the surgeon general's report concludes that smoking is associated with stillbirth and neonatal death, and it may increase ectopic pregnancy and spontaneous abortion. Infants born to smokers tend to be low-birth-weight and small for their gestational age. The March of Dimes notes that obesity and diabetes are associated with maternal and fetal complications, including birth defects, miscarriage and stillbirth.
Despite the well-publicized consequences of maternal smoking, 12% of new mothers reported that they smoked while pregnant in 2001, and CDC considers these data to be a low estimate. The maternal smoking rates are twice or three times this overall rate for young white teens and women, and they differ immensely by education—43% among white women who attended but did not finish high school compared with 2% among college graduates. Although four in 10 smokers stop while they are pregnant, seven in 10 of those relapse within one year of delivery.
In terms of fertility, the surgeon general's report found that women who smoke find it more difficult to conceive than nonsmokers, that smoking is positively associated with infertility and that smoking may be detrimental to in vitro fertilization. Papers prepared for the American Society for Reproductive Medicine estimate that 13% of female infertility is caused by smoking and that 6% is caused by obesity; both factors may also impair male fertility.
Smoking and obesity are also limiting factors in terms of women's contraceptive choice, and the evidence suggests that obesity may reduce contraceptive efficacy as well for at least some hormonal methods. The surgeon general's report concludes that women (especially older women) who smoke and use oral contraceptives have especially high risk for heart disease. The prescribing information for combined hormonal contraceptives warns explicitly of these problems and strongly advises women who use these methods not to smoke. Obesity contributes to hypertension, diabetes and other cardiovascular risk factors that may preclude the use of some hormonal contraceptives. Moreover, several studies have indicated that high body weight decreases the effectiveness of some hormonal contraceptives (by 60%, according to a study published in the May 2002 issue of Obstetrics & Gynecology).
Family Planning's Relevance
Given this long list of negative impacts, helping women to avoid smoking and obesity in the first place clearly would improve their reproductive health. And for those already affected by one or both conditions, smoking cessation and weight loss can reverse many of the risks associated with pregnancy, fertility and contraceptive use. The surgeon general's report on smoking, for instance, concludes that women who quit before or during pregnancy reduce their risk for infertility, low birth weight and several other adverse outcomes.
Reproductive health providers, and particularly the national network of some 7,000 family planning clinics across the country, are especially well suited to help. Together, these clinics reach out to 6.6 million women each year; eight in 10 of their clients are under age 30 and nine in 10 have low or marginal incomes (under 250% of the federal poverty level). In fact, according to a 2001 analysis by The Alan Guttmacher Institute (AGI), women who obtain their reproductive health care from family planning clinics are more likely than those who receive such care from private physicians or HMOs to be young, black or Hispanic, uninsured or on Medicaid, and to have not completed high school (see chart). Those groups of women have been cited as targets for antismoking and antiobesity activities because of their high or increasing rates of the two conditions.
| On Target |
| The clients of family planning clinics are especially likely to have characteristics that put them at high risk of smoking or obesity. |
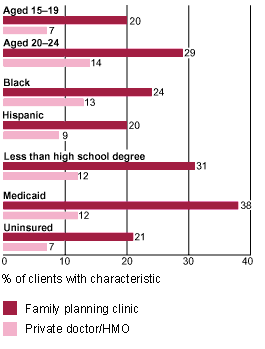 |
|
Source: Frost JJ, Public or private providers? U.S. women's use of reproductive health services, Family Planning Perspectives, 2001, 33(1):4-12. |
Furthermore, family planning providers—who have substantial experience and expertise providing counseling and education on healthy behaviors and behavior change—are interacting with these women at points in their life that may be especially opportune for antismoking and antiobesity messages. Young women in general are critical to reach, as lifestyle habits, including smoking, diet and exercise, are often formed early in life and may be difficult to change later. To the extent that these women are weighing their contraceptive options, information about the dangers of smoking and the importance of good nutrition are directly relevant. And because a central family planning service is preconception counseling and education, women in family planning clinics who are considering pregnancy can be encouraged, if necessary, to alter their behavior in advance of becoming pregnant so as to encourage the best possible health outcomes for themselves and their child.
What Is Being Done
Reducing smoking among pregnant women, in particular, has long been a goal shared by providers and advocates within and outside of the reproductive health community. For example, the American College of Obstetricians and Gynecologists (ACOG), in November 2002, published a provider guide for smoking cessation during pregnancy that focuses on a quick (5-15 minutes) and proven counseling method. They have disseminated such information and pursued other antismoking strategies in collaboration with Smoke-Free Families, a Robert Wood Johnson Foundation-funded program that is coordinating the National Partnership to Help Pregnant Smokers Quit.
Meanwhile, the program guidelines for Title X-funded family planning projects include a number of recommendations that are relevant to nutrition, exercise and smoking cessation. They note that at a patient's initial comprehensive clinical visit, a complete medical history must be obtained, which must address chronic or acute medical conditions and the use of tobacco and other substances. For female clients, a complete physical examination should also be performed, as "for many clients, family planning programs are their only continuing source of health information and clinical care." The guideline's recommendations for client education and counseling also include the topics of nutrition, exercise, smoking cessation and substance use and abuse.
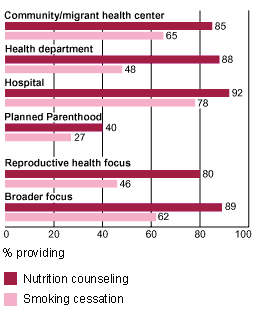
An AGI study, published in 2002, of health departments, hospitals, Planned Parenthood affiliates and other types of agencies that run publicly funded family planning clinics found that a large proportion of these agencies offer nutrition counseling and smoking cessation services. Not surprisingly, hospitals and agencies with more comprehensive health programs are more likely than more specialized reproductive health agencies to offer these services (see chart).
| Preventive Services |
| Agencies that administer family planning clinics are relatively more likely to provide nutrition counseling and smoking cessation services if they have a more comprehensive health care program. |
 |
|
Source: Finer LB, Darroch JE and Frost JJ, U.S. agencies providing publicly funded contraceptive services in 1999, Perspectives on Sexual and Reproductive Health, 2002, 34(1):15-24. |
This situation may be changing, particularly for smoking cessation. Planned Parenthood Federation of America (PPFA) is writing new standards and guidelines on smoking cessation in response to requests from its affiliates, according to Vanessa Cullins, vice president for medical affairs. PPFA is also exploring the idea of guidelines relating to weight loss and obesity. Cullins adds that a number of Planned Parenthood affiliates are already offering services such as smoking cessation. And, of course, Planned Parenthood providers (as well as other family planning providers) are guided in their client counseling and education by published medical evidence and expert authorities.
ACOG, too, is looking to expand its antismoking efforts beyond its traditional focus on pregnancy. With support from DHHS, ACOG is helping to set up state-level partnerships among maternal and child health-related providers, and smoking has been a top priority. The group has also worked with the Women's Tobacco Prevention Network, formed at the behest of CDC in 2001 to target women as a priority for prevention. On the obesity front, ACOG released in July a new monograph about weight control that provides doctors with a detailed overview of how obesity comes about and of options for screening, counseling and treatment.
Barriers for Providers
Many of these new efforts are aimed at provider education and mobilization, reflecting a belief that providers' lack of knowledge, training or—for whatever reason—motivation can be barriers to patients' care. Jeanne Mahoney, director of ACOG's provider's partnership project, for example, believes that family planning providers are already feeling overwhelmed and that it may seem to them that even a short counseling intervention is too long to add into a family planning visit. Nevertheless, she believes in the "drop-in-the-bucket theory"—that small actions by a provider (e.g., a referral or a small amount of counseling) add up over time, particularly as multiple providers add to the message.
Another concern for some providers is that a poorly tailored message has the potential to alienate or even harm their patients. Kathleen Baldwin, vice president for education and training at Planned Parenthood of Greater Indiana, is working with a coalition on obesity in Indianapolis. One of her objectives, she says, is to keep the coalition conscious of an antiobesity message's possible impact on body image, including the danger of eating disorders and of increased smoking, which is sometimes used as a tool for staying slim.
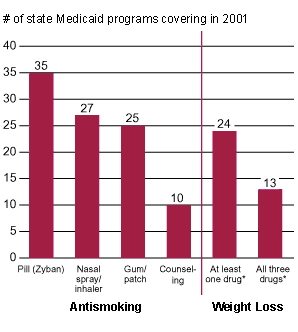
Lack of reimbursement may be the most serious barrier, however. A report by the Partnership for Prevention found that in 1997, only about one-quarter of employer-sponsored health plans covered smoking cessation devices and drugs or counseling for either smoking cessation or nutrition and physical activity. Medicaid coverage for smoking cessation is also scanty, according to a May CDC report; perhaps most striking is the small proportion of state Medicaid programs that provide reimbursement for counseling. Similarly, state Medicaid programs typically exclude coverage for obesity, including drugs for weight loss, according to the American Obesity Association (see chart). The barrier may be psychological as well as practical: ACOG's Mahoney suggests that by failing to reimburse providers even a little, insurers send the message that these efforts are not valued.
| Medicaid Gaps |
| Many states have chosen not to cover treatment for smoking and obesity. |
 |
|
Source: *Without restriction to a narrow list of conditions. Sources: Halpin HA, et al., State Medicaid coverage for tobacco-dependence treatments—United States, 1994-2001, Morbidity and Mortality Weekly Report, 2003, 52(21):496-500; American Obesity Association, Medicaid reimbursement for prescription weight-loss drugs, <http://www.obesity.org/treatment/medicaid.shtml>, accessed June 11, 2003. |
Providers of subsidized family planning services are already operating under severe financial constraints ("Nowhere But Up: Rising Costs for Title X Clinics," TGR, December 2002, page 6). Those seeking to expand or augment their antismoking and antiobesity activities may be heartened by the potential availability of new sources of federal support in these areas. The DHHS community-grant program announced in May, for instance, is allocating nearly $14 million for FY 2003 to prevent diabetes, asthma and obesity through such measures as improving nutrition, increasing physical activity and reducing tobacco use. The administration's budget for FY 2004 asks for a major increase, to $125 million. The Frist legislative proposal would allocate $60 million per year for provider training, community-based programs and government research relating to improved nutrition, increased physical activity and obesity prevention. These grants would add to federal funding already provided to state health agencies, including $100 million from CDC for tobacco use prevention and $34 million for nutrition, physical activity and obesity.
The extent to which the proposed new funding actually will materialize remains to be seen. What also remains to be seen is the extent to which family planning clinics will be able to gain access to new and existing funds for their antismoking and antiobesity programs. It would certainly appear, however, that policymakers are making smoking cessation, obesity prevention and other lifestyle changes a priority. And there is little doubt that family planning providers are well equipped to make valuable contributions to those efforts.
