New research from The Alan Guttmacher Institute (AGI) shows that in 2002, nearly nine in 10 group health insurance plans purchased by employers typically covered the full range of prescription contraceptives. This level of coverage marks a dramatic improvement since 1993, when AGI conducted the first national study of private insurance coverage of reproductive health services. The new study also demonstrates that plans in states with contraceptive coverage mandates have significantly more extensive coverage than do plans designed specifically to provide coverage in states without such mandates—and that the state mandates have been particularly important in closing historic coverage gaps among the various individual contraceptive methods. As a result of these advances, large numbers of women with private health insurance should now be much more able to choose the contraceptive method they are most comfortable with and, therefore, are likely to use effectively. Although enormously encouraging, the study's overall findings to some extent mask considerable coverage gaps that still exist in important segments of the U.S. insurance market. In so doing, they highlight what is yet to be accomplished to ensure that contraceptive coverage extends to all U.S. women who need it and that coverage translates into real access for women.
Progress Duly Noted
In 2001 and 2002, AGI researchers surveyed insurance companies across the country, asking whether prescription contraceptives and other comparable drugs, devices and services were covered in the "typical" managed care plans of various types they wrote for employers. In effect, the study covers about half of the private-sector, employer-sponsored insurance market in the United States; it could not look at the coverage provided by employers who choose to "self-insure," paying directly for their employees' care.
The findings, published in the March/April 2004 issue of Perspectives on Sexual and Reproductive Health, show that contraceptive coverage in employer-purchased plans improved dramatically between 1993 and 2002. The proportion of typical plans covering the full range of reversible contraceptive methods tripled from 28% to 86%, and the proportion covering no method at all plummeted from 28% to 2%.
As a result of this dramatic overall shift, several major coverage disparities that had been so glaring in 1993 have all but disappeared for this type of insurance (see chart below). First, whereas coverage of prescription drugs in general was the industry norm in 1993, plans were far less likely to cover prescription contraceptives. Indeed, it was this disparity that sparked the charge that insurance plans were biased against women, covering men's prescription drug needs while ignoring a basic health care need of women. By 2002, only a small proportion of plans had a drug benefit that excluded prescription contraceptives.
| Closing the Gaps |
| By 2002, plans were about as likely to cover reversible contraceptives as to cover abortion, sterilization or prescription drugs generally, and variation among individual methods had largely disappeared. |
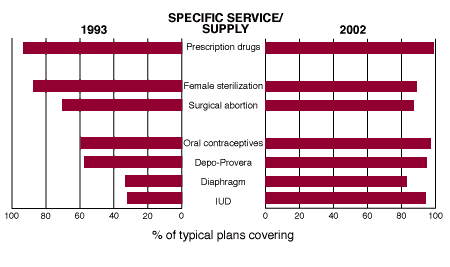 |
Source: Sonfield A, Gold RB, Frost JJ and Darroch JE, U.S. insurance coverage of contraceptives and the impact of contraceptive coverage mandates, 2002, Perspectives on Sexual and Reproductive Health, 2004, 36(2):72-79. |
Second, in contrast to their low levels of coverage for reversible contraception, insurance plans in 1993 routinely covered abortion and contraceptive sterilization. Critics attributed this to an industry-wide bias toward surgical services and against preventive care, particularly among more traditional, fee-for-service insurance plans. This disparity had been eliminated entirely by 2002.
A third disturbing finding in 1993 was the variation in patterns of contraceptive coverage among types of insurance plans. Coverage was lowest among fee-for-service ("indemnity") plans and preferred provider organizations (PPOs), the form of managed care that most resembles fee-for-service coverage; half of indemnity plans and PPOs covered no contraceptives at all in 1993. Coverage was highest among health maintenance organizations (HMOs), which had long encouraged preventive care as one of many cost-control tactics. By 2002, these variations had become largely negligible.
Finally, plans in 1993 displayed considerable variation in coverage among specific contraceptive methods. Most of these gaps had closed by 2002, and even methods that only recently had been brought to the U.S. market were widely covered; almost nine in 10 plans typically covered the one-month injectable, and more than nine in 10 covered emergency contraception.
The Impact of Mandates
The drive to enact state laws requiring employers to provide contraceptive coverage to their employees has been a key strategy in a decade-long, multipronged advocacy campaign to increase private-sector coverage overall (see related story, page 6). The AGI study demonstrates that these state mandates, 15 of which were in effect at the beginning of the study, have had a dramatic impact. In the plans affected by mandates, coverage among the various contraceptive methods has been virtually equalized.
The mandates have acted to increase coverage both directly and indirectly. First, plans in states with mandates were more likely than plans in states without mandates to cover a full range of contraceptives in 2002. Plans in states with mandates were also more likely to cover most individual methods.
Second, the mandates had a sizable impact beyond state borders. This is because plans designed at the national level by insurance companies operating in states both with and without mandates provide coverage everywhere in accordance with the mandates. In 2002, almost six in 10 plans in states without mandates were plans of this type and provided nearly universal coverage; in their absence, overall coverage in the states without mandates would have been considerably worse. In fact, plans designed specifically to provide coverage in states without mandates (excluding those nationally determined plans) did have significantly less-extensive coverage in 2002. For example, fewer than half of the PPOs designed specifically in states without mandates covered all of the leading contraceptive methods (see chart below); more than one in 10 such PPOs had no contraceptive coverage at all.
| Mandates Matter |
| In 2002, plans of all types in states with contraceptive coverage mandates were more likely to cover all of the five leading contraceptive methods than were plans designed specifically for states without mandates. |
 |
See source, chart on page 4. |
Implications for Women
These new findings imply that millions of American women, at least theoretically, are significantly better off than they were a decade earlier. Increased coverage of contraception should translate into basic health care that is more affordable for women. Paid for out-of-pocket, oral contraceptives can cost between $15 and $45 each month, not counting the annual exam that physicians usually require before they will prescribe the method. Longer-acting methods, such as the IUD or Depo-Provera—which can be particularly effective at preventing unintended pregnancy, in part because they provide few opportunities for misuse—can require considerably greater up-front payments.
Because coverage in many more plans is now nearly universal across a broad range of contraceptive methods, women should be much more able to exercise true contraceptive choice, unencumbered by concerns about coverage and cost. This enhanced choice can be vital to efforts to prevent unintended pregnancy. Differences in coverage and price may block a woman from choosing the method that may be most appropriate for her health and lifestyle, and thus the method she is most likely to use consistently and correctly. Cost may lead women to use a method inconsistently—to delay refilling an oral contraceptive prescription or returning for a periodic injection—or to not use a method at all.
Such problems are not mere speculation. A 1998 poll commissioned by the Kaiser Family Foundation found that three-quarters of adult women cited coverage as influencing their choice of method. And a 2000-2001 AGI survey of women having an abortion found that among women who became pregnant despite using oral contraceptives, one in 10 reported using the method inconsistently because they had run out of supplies; almost one in 10 women who had not been using a contraceptive method in the month they became pregnant reported financial concerns as the reason.
Future Steps
Although the trends in contraceptive coverage are heartening, there is still a long way to go before coverage is universal. The AGI study demonstrates that coverage gaps are still glaring among employer-purchased plans unaffected by a state mandate—and 30 states, accounting for more than half of American women of reproductive age, do not have such a mandate. Moreover, self-insured plans are beyond the reach of state mandates (although not of federal law); because these plans, which cover about half of all Americans with employment-based coverage, were outside the scope of the AGI study, little is known about the extent of their coverage. Employees of small businesses, too, are a group to be concerned about. According to annual surveys of employers conducted by the Kaiser Family Foundation and the Health Research and Educational Trust (HRET), these employees have had particularly low levels of coverage; they are also particularly likely to have low incomes and, thus, be vulnerable to cost concerns.
Another important consideration is that coverage, in and of itself, may not be enough for many women. Insurance plans typically require copayments that may effectively render service use unaffordable. According to the Kaiser/HRET surveys, the average copayment in 2003 was $29 for a "non-preferred" drug (such as a brand-name drug that has generic substitutes), up from $17 just three years earlier. A study published in 2004 in the Journal of the American Medical Association found that doubling copayments was associated with reduced use of eight common types of prescription drugs. Contraceptive drugs were not included in the study, but it is notable that reductions in use were particularly high for drugs that had over-the-counter alternatives, a group that would include prescription contraceptives.
Women may also lack information about what their insurance covers or may experience insurance-related barriers to accessing care. A 1996-1997 AGI study of managed care plans in five states, for instance, found that only half of commercial plans routinely told enrollees which contraceptive methods were covered, and one-third of enrollees reported difficulties obtaining contraceptive services. In addition, we know little about whether plans are adequately covering the time providers need to provide contraceptive counseling services. These services can help ensure that women are choosing the best method for them and using it most effectively.
Finally, for the millions of Americans with no insurance coverage at all, the reality or even the promise of increased coverage for contraception is essentially irrelevant. These women must scrape together the necessary funds themselves or depend on services provided by family planning clinics subsidized by the government—clinics that are chronically under funded ("Preventing Unintended Pregnancy: The Need and the Means," TGR, December 2003, page 7). Until this situation is comprehensively addressed, universal access to the services and contraceptive methods women need to prevent unintended pregnancy will continue to be only a dream.
