Telehealth is changing how people around the world access health-related information and services. In the United States, where access to abortion is highly politicized and varies from state to state, telehealth provision of abortion has improved access to care in some states. Yet federal and state restrictions limit whether and how patients can use this type of care. Lifting these restrictions could expand abortion access to new and underserved communities. It could also allow for the growth of additional telehealth models that offer increased convenience, flexibility and privacy.
What Is Telehealth?
While there is no single, all-encompassing definition, "telehealth" generally refers to the use of electronic information and telecommunication technologies to facilitate the delivery of health-related information, education and services. It is often associated with the provision of clinical health care across long distances or outside of traditional facilities, and it includes both provider-to-patient and provider-to-provider interactions. Examples include everything from exchanging information or services via text messages, email, specialized software applications or video conferencing to performing complicated surgeries using robotic instruments guided by a clinician at a remote location. "Telehealth" sometimes refers to a broader range of interactions and exchanges than "telemedicine," but the terms are often used interchangeably.
Telehealth has long been hailed as a promising way to expand health care, including highly specialized care, to rural and otherwise underserved communities. In 2005, the Institute of Medicine’s Committee on the Future of Rural Health Care noted that "appropriate use of [information and communications technology] can bridge distances by providing more immediate access to clinical knowledge, specialized expertise, and services not readily available in sparsely populated areas."1 As of December 2018, 79 million Americans in rural and urban areas lived in federally designated primary care Health Professional Shortage Areas.2
So far, various metrics confirm that telehealth is transforming the provision of health care in the United States. According to the American Hospital Association, more than half of U.S. hospitals use some form of telemedicine,3 and analyses of private insurance records suggest rapid patient uptake over the past decade.4,5 Nonetheless, it is evident that telehealth has not nearly reached its full potential: In 2016, just 15% of physicians worked in practices that used telemedicine for patient interactions and 11% worked in practices that used it for interactions with other health care professionals.6
Innovative telemedicine programs in states like Arkansas and South Carolina are helping connect pregnant patients with obstetrical and neonatal specialists, in coordination with their local health care providers.7 This use of telehealth can help address provider shortages: Half of U.S. counties lacked an obstetrician-gynecologist in 2017, and more than 10 million women lived in those predominantly rural counties.8 Examples from the maternal health arena demonstrate the potential of telehealth to expand access to a wide range of sexual and reproductive health care, including abortion care.
Telehealth Abortion Services
Abortion care in the United States has evolved as a primarily clinic-based service, segregated from the resources and infrastructure dedicated to other health care. As a result, there are huge gaps in access, including many areas of the country that are not served within a reasonable distance by a health center providing abortion care.9 One innovative, if partial, solution to these gaps is telehealth, which is increasingly being used to make medication abortion available in new areas.
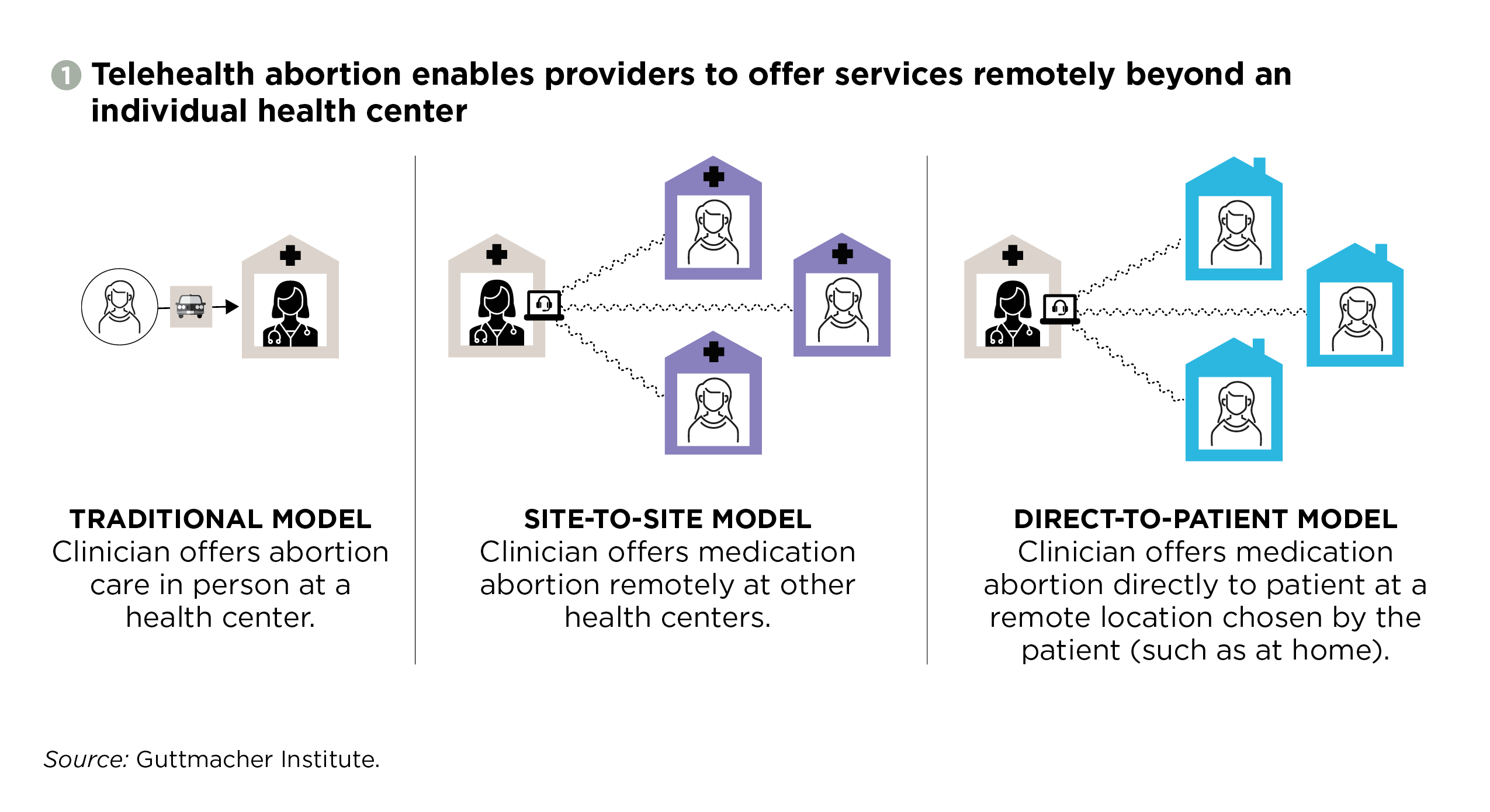
Under the traditional clinic-based model, a patient visits a health center and receives abortion care in person from an on-site clinician (see figure 1). In 2008, however, Planned Parenthood of the Heartland pioneered telehealth access to abortion when it began using telehealth at health centers in Iowa not regularly staffed by a clinician providing abortion care.10 Today, Planned Parenthood health centers offer medication abortion via telehealth in at least 10 states, and some independent abortion providers have also begun integrating telehealth.11,12 Under this site-to-site model, the process is similar to the in-person model in that a patient must still visit a health center for a consultation and screening with on-site staff.13 However, a patient who is eligible and opts for medication abortion is then connected to a clinician at another health center via videoconference. During this interaction, the clinician reviews the patient’s medical records, answers any questions and remotely authorizes the medication.
This model has been proven to be safe and effective, and qualitative research indicates both patients and providers find it to be a positive experience.14–17 In Alaska, where Planned Parenthood of the Greater Northwest and the Hawaiian Islands began offering telehealth abortion in 2011, providers indicated that use of this model not only increased patient choice, but also resulted in patients being seen sooner and closer to home.17 This is consistent with findings from Iowa, where the creation of the telehealth program was associated with improved access to medication abortion—particularly for patients who lived more than 50 miles from the nearest clinic offering surgical abortion—and increased odds of obtaining abortion care in the first trimester.10
Another telehealth abortion model is currently being piloted and studied by Gynuity Health Projects, with special approval from the U.S. Food and Drug Administration (FDA). The TelAbortion Study began in 2016 and is now open to participants in eight states.18,19 Under this direct-to-patient model, someone seeking abortion care does not need to visit a health center but instead consults with a clinician via videoconference from a location of her choosing, such as her own home. Any required tests, such as an ultrasound and blood work, are completed at a local laboratory or health care facility and the pills are mailed directly from the study clinician to the patient. After using the medication, the patient completes follow-up testing locally to ensure the pregnancy has terminated and has another video consultation with the abortion provider. Data from the first four pilot states (Hawaii, New York, Oregon and Washington) suggest this method is a feasible, safe and acceptable option for patients.20
Overcoming Challenges
Although telehealth offers one clear way to expand access to medication abortion, the politicization that isolates abortion from other types of health care also limits its reach and could stand in the way of further expansion and innovation. Overcoming the following obstacles is a necessary precursor to realizing the full potential of abortion provision using telehealth.
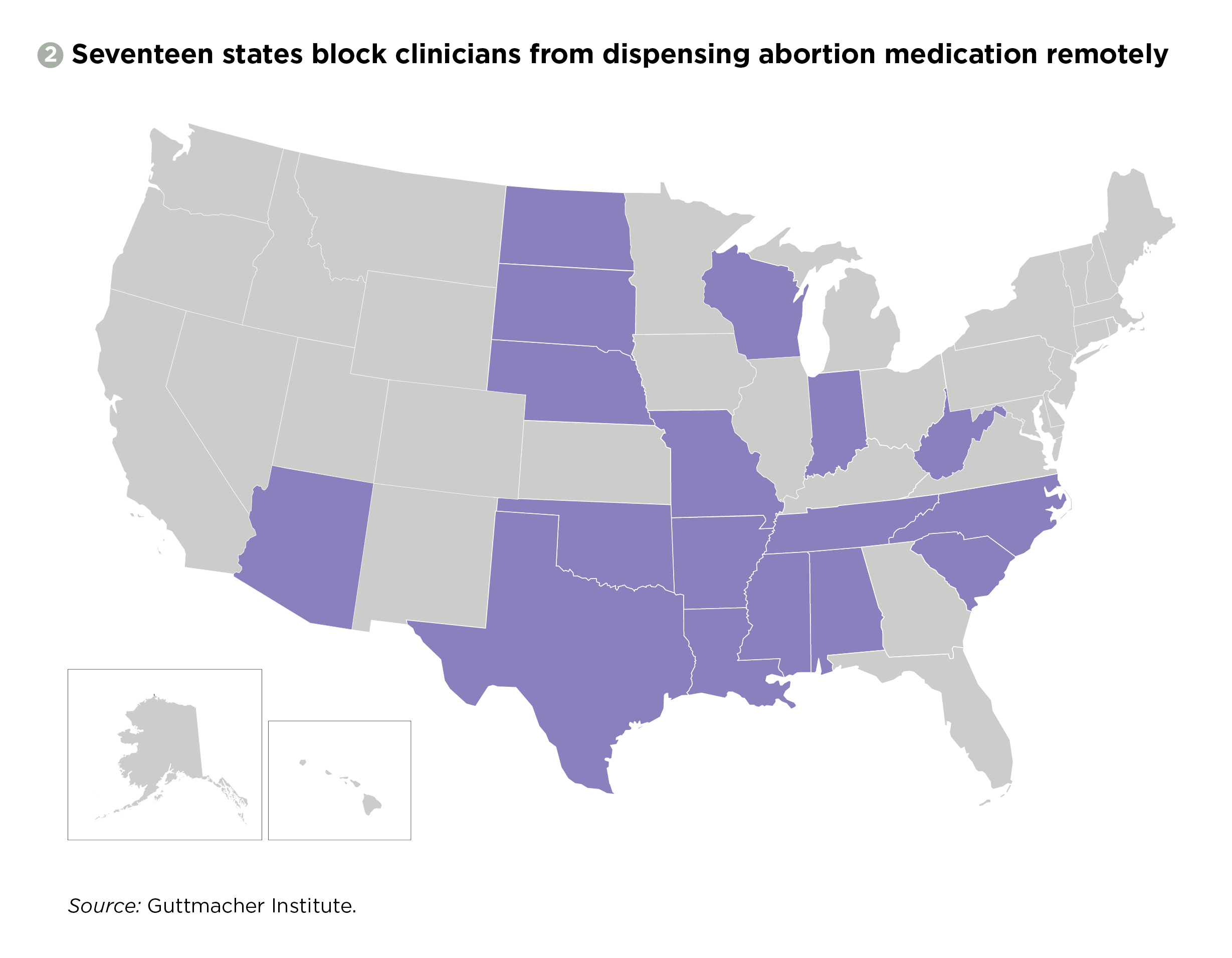
State telehealth abortion bans. Seventeen states currently require the prescribing clinician to be physically present when medication abortion is dispensed, effectively banning the use of telehealth (see figure 2).21 Removing these restrictions would allow providers to expand medication abortion services to patients in these states using the site-to-site model pioneered by Planned Parenthood, and it would be a necessary precondition to implementation of the direct-to-patient model used in the TelAbortion Study.
FDA restrictions. Mifepristone (one of the two drugs used in the FDA-approved medication abortion regimen) is subject to an FDA-imposed and medically unwarranted Risk Evaluation and Mitigation Strategy (REMS), which requires the medication to be dispensed only by certified prescribers and only in clinics, medical offices or hospitals.22 As a result, and unlike most other safe and effective medications, it cannot be sold at pharmacies.
The FDA is authorized to design and impose a REMS "for certain medications with serious safety concerns to help ensure the benefits of the medication outweigh its risks."23 Given mifepristone’s extensive safety record since it was approved for use in the United States in 2000, the REMS restrictions are not justified, which is why leading medical organizations such as the American Medical Association and the American College of Obstetricians and Gynecologists support their removal.24,25
If the FDA removed the REMS, medication abortion providers could go beyond the site-to-site telehealth model and offer the direct-to-patient model currently being piloted through the TelAbortion Study. Patients could receive the medication by mail directly from the clinician (as they do under the current study) or receive a prescription after their telehealth consultation and fill that prescription at a local or online pharmacy, enhancing patient choice.
Telehealth across state lines. Realizing the full potential of telehealth requires figuring out how to make it work most effectively throughout the United States. But by and large, the regulation of medicine and medical practice is the purview of individual states. Laws and policies governing clinician licensing, prescribing authority, insurance reimbursement, malpractice and many patient protections differ among states in ways big and small, creating a complex patchwork for providers to navigate.26 Moreover, some state laws serve as explicit barriers to telehealth, such as rules that require an established physician-patient relationship or an in-person exam before a prescription can be furnished remotely.
As a result, the entire health care industry continues to grapple with how best to support and enhance telehealth systems that extend across state lines. For example, one response to the licensing issue is to enter into multistate compacts, which allow a provider licensed in one state to receive reciprocity or expedited licensing in the other states participating in the agreement.27 As policymakers devise solutions to these sorts of challenges to help telehealth realize its full potential, it is critical that abortion care is not excluded from the policies they put in place.
In this context, restrictive policies specific to abortion further complicate the extent to which clinicians can extend care into other states using telehealth. Lawmakers hostile to abortion have imposed a variety of onerous and unnecessary restrictions on abortion providers and patients over the decades,28 and the applicability of these policies must be assessed for every new state in which a clinician wishes to serve. In other words, telehealth is not an automatic work-around or solution to many state abortion restrictions, which must be lifted in order to expand access to abortion care, whether via telehealth or otherwise.
Funding. Of course, it takes money to incorporate new technologies and infrastructure and to change how entire systems operate and health care is delivered. Due to the segregation of abortion services from other health care, some of the standard ways health care providers access new funds and technology—such as through hospital networks or incentives from insurers—already exclude many abortion providers. In addition, a tactic frequently pursued by antiabortion policymakers is to exclude abortion providers and abortion care from public funding streams.
Ensuring that abortion providers can acquire the technology and build the infrastructure they need to provide telehealth services requires, at the very least, ensuring that they are not excluded from dedicated telehealth resources such as public grants. Larger changes that would help to ensure abortion providers have the resources and financial stability to incorporate innovations such as telehealth include reintegrating them into broader health care networks, reversing existing funding restrictions and defending against new encroachments.
Affordability. Cost is one of the biggest factors that make it difficult to obtain abortion care in the United States, and existing barriers to insurance coverage of abortion combined with emerging telehealth policies could exacerbate inequities in who can access telehealth abortion.29,30 Whether and how insurers cover telehealth services varies considerably and continues to evolve across state Medicaid programs, private insurance plans, and other federal and state health insurance programs.26 For example, some states encourage or mandate that insurance plans include telehealth services, but this does not necessarily mean that a telehealth service is reimbursed at the same rate as an in-person service.
Moreover, even if a health plan covers telehealth services generally, it may not cover telehealth abortion. The Hyde Amendment and similar federal policies block millions of people from having insurance coverage of abortion under Medicaid and other federal programs.30 Many states also bar private insurance coverage of abortion in the Affordable Care Act marketplaces or throughout the private insurance market.31 Realizing the full potential of telehealth abortion, especially for low-income and otherwise marginalized patients, requires eliminating existing financial barriers and ensuring that abortion is explicitly covered under and adequately reimbursed by public and private health insurance plans.
Looking Ahead
Challenges and limitations notwithstanding, telehealth abortion has the potential to greatly expand access for individuals and communities across the country. Fully realizing this potential requires overcoming multiple obstacles, some specific to abortion and others related more generally to telehealth. In addition, if the conservative majority in the U.S. Supreme Court takes action in coming years to undermine abortion rights and the state policy landscape becomes all the more polarized, telehealth would be a significant—perhaps vital—way to extend the capacity and reach of the abortion providers still operating. Both in preparation for that day and to expand abortion access now, policymakers must take action to remove existing restrictions and ensure that abortion is included in telehealth-related policies and funding opportunities.