CONTEXT
Sexually experienced women are at risk of cervical cancer, one of the most common female reproductive cancers. Nearly 20% of U.S. women aged 18–64 have a disability, and disability is associated with health care access; however, the relationship between disability and Pap smear receipt remains underexplored.
METHODS
Data on 20,907 women aged 21–64 from the 2000 and 2005 National Health Interview Surveys were used to investigate the relationship between disability and cervical cancer screening. Logistic regression analyses were conducted to assess the association between disability and both women's receipt of a Pap smear and their receipt of a doctor's recommendation for a Pap smear in the past year.
RESULTS
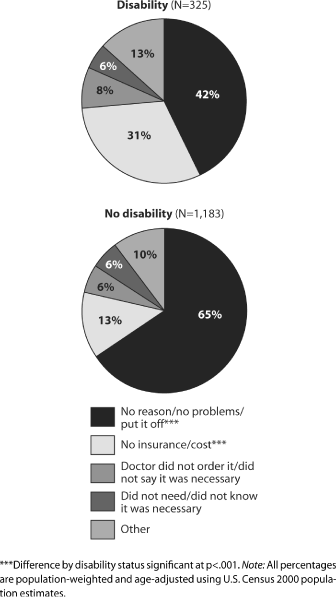
Having a disability was negatively associated with Pap smear receipt (odds ratio, 0.6). Compared with women with no disabilities, those with mobility limitations and those with other types of limitations had reduced odds of having received a Pap smear (0.5–0.7). Disability was positively associated with having received a recommendation for a Pap smear (1.2); however, among women who had received a recommendation, those with disabilities had reduced odds of having received a Pap smear (0.5). Among women who had not received a Pap smear, 31% of those with disabilities and 13% of others cited cost or lack of insurance as the primary reason.
CONCLUSIONS
The negative relationship between Pap smear receipt and multiple types of disability suggests barriers beyond the human-made physical features of the environment. Efforts to reduce inequalities in reproductive health care access should consider the needs of women with disabilities.