The Trump administration and social conservatives in Congress are engaged in broad-based attacks on sexual and reproductive health and rights in the United States and globally. In the international sphere, the administration has imposed and expanded the global gag rule and defunded the United Nations Population Fund (UNFPA), while calling for outright elimination of all U.S. international family planning aid during its first year in office (see "When Antiabortion Ideology Turns into Foreign Policy: How the Global Gag Rule Erodes Health, Ethics and Democracy," 2017, and "The Benefits of Investing in International Family Planning—and the Price of Slashing Funding," 2017). At the heart of these attacks is an extreme animus toward abortion rights. Advocates for women’s health fear that these attacks will roll back improvements in sexual and reproductive health services that were built over decades. This is especially true in developing regions where unsafe abortion is a serious public health issue and the limited progress to date is in jeopardy.
Almost all nations, including donor countries such as the United States, have pledged to financially support at least some measures to decrease the incidence and negative consequences of unsafe abortion through their commitments at the landmark International Conference on Population and Development in Cairo in 1994 and subsequent United Nations conferences.1,2 In the years since, researchers and health care practitioners have continued to compile evidence about the most effective means to decrease the impact of unsafe abortion globally and the obstacles to implementing these measures. This body of evidence provides a roadmap for policymakers to take concrete measures to protect the health, rights and lives of women worldwide.
Much of this evidence has been synthesized in a new study by the Guttmacher Institute on abortion around the world.3 This study found substantial changes over time in abortion incidence, legality and safety. Abortion is becoming safer worldwide as a result of slow but important improvements made to abortion policies, programs and practices in a number of countries. Yet, millions of women living in developing countries where abortion is highly restricted continue to experience the widespread and dangerous consequences of unsafe abortion.
Tracking Abortion Incidence and Safety
The Guttmacher report projects that the overall abortion rate declined slightly over the last 25 years. This global trend varied by development status: The rate in developing regions did not change, whereas the decline in developed regions was substantial. Specifically, an estimated 27 abortions per 1,000 women of reproductive age (aged 15–44) occurred each year in developed regions during 2010–2014, down from 46 per 1,000 during 1990–1994. By contrast, the rate in developing regions remained almost the same at 36–39 per 1,000 women.
Dramatically falling abortion rates in Eastern Europe largely drove the decreased abortion rate within developed regions. Not surprisingly, the underlying cause was a decline in unintended pregnancy due to increased access to and use of modern contraceptives in former Soviet Bloc states after they gained independence.4 The evidence is clear that the most effective way to reduce abortion rates is to prevent unintended pregnancies through modern contraceptives.
When it comes to abortion safety, the news is mixed. Globally, 56 million abortions occur each year and nearly half (25 million) are unsafe.5 Unsafe abortion is an important preventable cause of maternal death and disability, accounting for 8–11% of maternal mortality worldwide and claiming the lives of 22,800–31,000 women annually (depending on the data source).6–9 Unsafe abortions are almost exclusively concentrated (97%) in developing countries.5
Advancements in abortion provision and postabortion care have precipitated a substantial decrease in abortion-related deaths worldwide. The estimated annual number of deaths per 100,000 abortions fell by 42% from 1990 to 2015.3 Declines in abortion-related mortality and morbidity—particularly in countries where abortion is illegal and the replacement of unsafe methods by the drug misoprostol for medication abortion has increased—have spurred researchers to recognize the changing reality of abortion and reconceptualize the framework for measuring and classifying the safety of abortion. In particular, experts have moved away from a dichotomy of safe (and legal) abortions versus unsafe (and illegal) abortions to a spectrum of safety.
In this new framework, abortions fall into one of three categories: safe, less safe and least safe.5 The World Health Organization (WHO) defines an abortion as safe if it is provided both by an appropriately trained provider and using a recommended method. Less-safe abortions meet only one of these two criteria—for example, if provided by a trained health worker using an outdated method or self-induced by a woman using a safe method (such as the drug misoprostol) without adequate information or support from a trained individual. Least safe abortions meet neither criteria; they are provided by untrained people using dangerous methods, such as sharp objects or toxic substances. Worldwide, an estimated 55% of abortions can be categorized as safe, 31% as less safe and 14% as least safe.5
This new framework acknowledges the evolving profile of abortion safety and its related risks, yet due to a lack of sufficient data, it does not account for many situations of self-management of medication abortion outside formal health systems. The categorization of these situations as safe, less safe or least safe may depend on many factors, such as the availability of professional medical care if complications arise, the level of training of the provider, the accuracy of information and quality of counseling, and the legal environment and legal risks associated with abortion provision.
Key Factors in Improving Abortion Safety and Health Outcomes
Many factors can influence the safety of abortion, including the method used, the qualifications of the person performing or assisting with the abortion, the accuracy of the information provided to the patient, the patient’s ability to access and pay for safe services, the health infrastructure of the country, and the cultural, social, legal and economic context where the abortion takes place. Over the last couple of decades, advancements in three particular areas have driven improvements in abortion safety and postabortion care.
First, the development and dissemination of clinical guidelines by WHO10–12 and national governments have steadily improved the quality of abortion provision.3 These technical standards have clarified the elements of comprehensive abortion care and improved service delivery in countries that permit abortions. Additionally, recommendations related to task-shifting service delivery from often-scarce doctors to a wider array of trained midlevel providers and from specialized to primary-care facilities have expanded the reach of abortion services.
Second, access to postabortion care to treat complications of unsafe abortion has also improved—again, fortified by WHO and national guidelines.3 Throughout the developing world (excluding Eastern Asia), an estimated 6.9 million women seek treatment every year for abortion complications.13 At the country level, providing these services can place a heavy burden on resource-strapped health systems. At the individual level, the consequences of unsafe abortion fall hardest on poor women, as they are more likely than more-affluent women to undergo unsafe procedures and are therefore exposed to a higher risk of postabortion complications. This risk is greater in clandestine settings, where abortion is illegal or where it occurs under secrecy outside of the formal health system even though it may be technically legal. Recognizing that untreated complications from clandestine and often-unsafe abortions can lead to hemorrhaging, sepsis and even death, national governments have agreed that postabortion care is a necessary component of maternal health care, including in countries where abortion is banned altogether. Indeed, almost all member states of the United Nations signed onto this consensus at the 1994 Cairo conference.1
Finally, a powerful trend in making abortion safer worldwide is women’s increasing access to safer methods of abortion in highly restricted environments—namely, medication abortion through the use of misoprostol, the second of two drugs in the combination medication protocol. Combination medication abortion consists of mifepristone plus misoprostol and is 95–98% effective in terminating pregnancies when used correctly.11 However, misoprostol is often used alone to induce abortions, especially in legally restrictive environments where mifepristone is unavailable. Misoprostol, which treats a range of medical conditions, is cheaper and more widely accessible on the market. Even though misoprostol alone is less effective than the combination protocol in completing an abortion (75–90% effective), it is recommended by WHO where mifepristone is unavailable because it is still far safer than invasive methods.11
Evidence, particularly from countries in Latin America and the Caribbean where legal abortion is highly restricted, suggests that misoprostol-only abortions are replacing dangerous methods and thereby reducing the severity of complications from clandestine abortions.3 Projections indicate that deaths from induced abortion would decline by two-thirds in developing regions if all women having unsafe abortions used misoprostol.14 Still, in many cases of misoprostol-induced abortion, women require medical care because they either experience an incomplete abortion after receiving insufficient or inaccurate information on how to use misoprostol correctly, or as part of the method’s expected failure rate. Lack of appropriate information on the normal process of an abortion with misoprostol and how to recognize expected symptoms may also result in some women seeking postabortion care who do not require medical intervention. All women who use misoprostol need accurate information about how it works and how to use it correctly. Even in regions where clandestine abortions regularly occur, efforts have shown that neutral counseling on abortion options followed by offering accurate information on misoprostol—without providing the drug itself—reduces health complications following abortion.15,16
Obstacles to Safe Abortion
Despite recent progress in improving abortion safety, many of the obstacles that stand in the way of eradicating unsafe abortion are entrenched and long-standing. Three of the most consequential barriers to further progress on reducing unsafe abortion relate to stigma, legality and high rates of unintended pregnancy, which can often result in unsafe abortion.
Stigma interferes with access to safe abortion in a number of ways. In societies throughout the world where sexual activity and childbearing outside of marriage are themselves highly stigmatized, the stigma associated with abortion forces women to prioritize secrecy over safety when seeking abortion procedures or other sexual and reproductive health services. Unmarried and young women in particular often face steep hurdles to obtaining contraceptive information and services, which places them at heightened risk of unintended pregnancy. Women who fear judgment by their families or health professionals and social sanction in their communities may avoid abortion and postabortion care in medical settings and seek clandestine abortion procedures instead. Even when these women seek safe and legal services, providers may be unwilling to offer them.
Stigma not only interferes with accessing abortion, but also with collecting data about it so that researchers can get an accurate picture of abortion practices and their full scope. Indeed, abortion data in many parts of the world are unreliable or incomplete. Often, women who fear stigma do not report their abortions; when seeking postabortion care for complications, many identify the outcome as a miscarriage rather than an abortion, particularly where having an abortion is criminalized. In turn, the lack of data makes it harder to devise effective and targeted proposals to overcome barriers to abortion care.
Stigma is closely related to the second long-standing obstacle to ending unsafe abortion: legal barriers to abortion access. As of 2017, 42% of women of reproductive age lived in the 125 countries where abortion is highly restricted—that is, prohibited altogether or permitted only to save a woman’s life or protect her physical or mental health.3 Almost all of these countries (93%) are in developing regions, whereas most of Europe, North America and several countries in Asia have broadly liberal abortion laws.
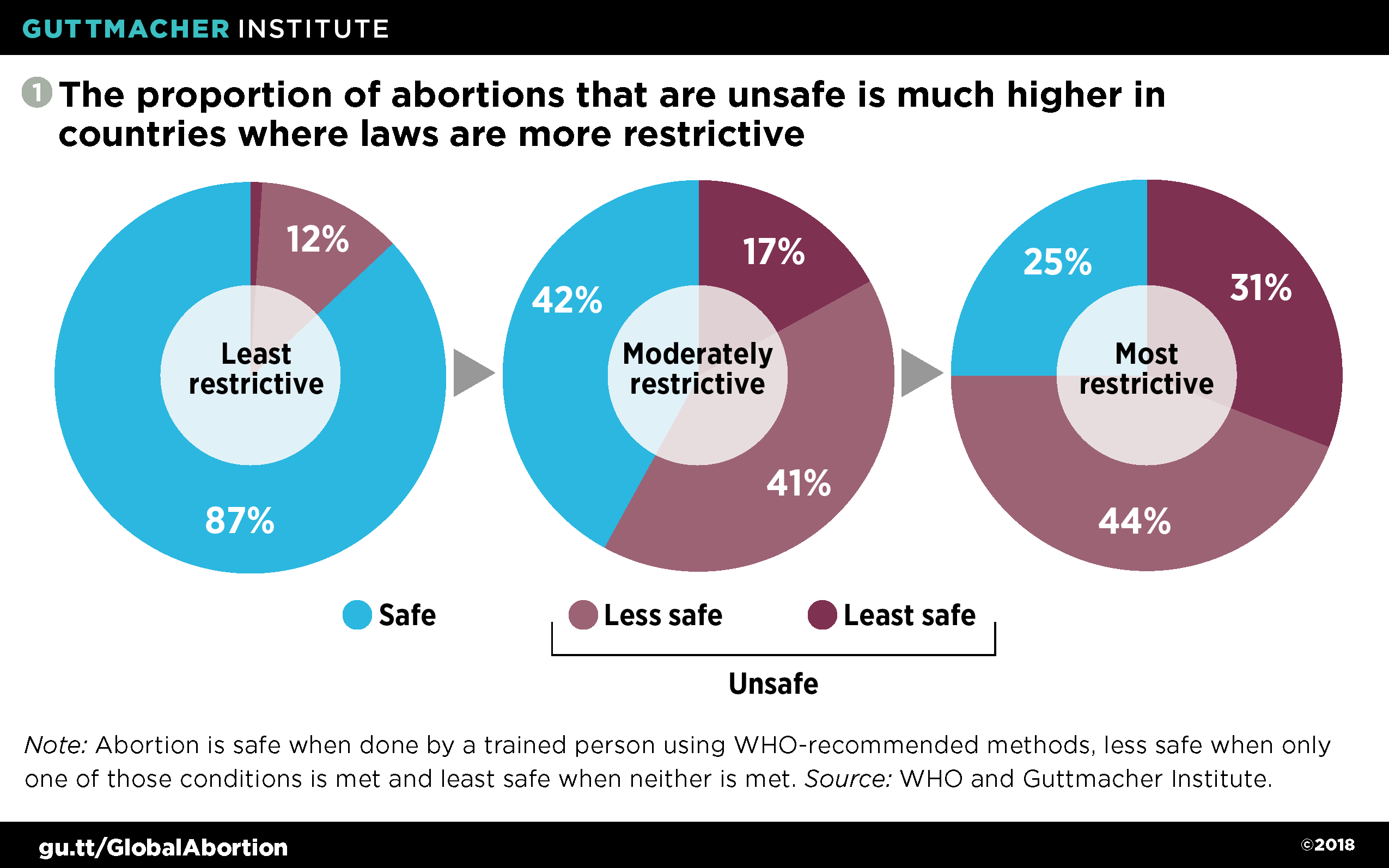
Notably, abortions occur just as frequently in countries with the most legal restrictions as in those with the fewest restrictions—37 versus 34 per 1,000 women.3 Nevertheless, a clear relationship exists between legality and safety. Abortion is least safe where it is most restricted: In countries where abortion is highly restricted, only 25% of abortions are safe; in countries where abortion is legal on all grounds, 87% of abortions are safe (see figure 1).5
Importantly, the slow but steady trend on legality has mostly moved toward liberalization of restrictive abortion laws. Between 2000 and 2017, 27 countries have expanded the grounds for abortion based on health or socioeconomic reasons, or removed restrictions based on specific reasons altogether; a total of 24 have allowed abortions for cases of rape, incest or fetal anomaly.3 Just one country, Nicaragua, changed its law to restrict access, prohibiting abortion under all circumstances.
The third main obstacle that relates to reducing unsafe abortion is unintended pregnancy, particularly where abortion is highly restricted. In developing regions, there is a nearly universal preference for smaller families and an increasing desire to control the timing and spacing of having children. The number of women of reproductive age in developing regions worldwide who have an unmet need for modern contraception—that is, they want to avoid pregnancy but are not using a modern contraceptive method—has declined in recent years but remains high at 214 million women.17 These women account for 84% of all unintended pregnancies in developing regions.
Unintended pregnancy is the main reason for almost all abortions. The highest unintended pregnancy rates are in Latin America and the Caribbean (96 per 1,000 women aged 15–44) and Africa (89 per 1,000)—well above the rate in developed regions (45 per 1,000).4 The regions of the world with the highest rates of unintended pregnancy are also those dominated by the strictest abortion laws. Therefore, women in those countries are forced to seek out illegal and often-unsafe methods to obtain an abortion. By satisfying unmet need for modern contraception, the numbers of unintended pregnancies, unplanned births and abortions would all drop by almost three-fourths from current levels.17
Taking Action on Safe Abortion
To further advance the progress that has been made around the world on reducing unsafe abortion, governments, donors, providers and advocates must engage in a concerted effort to overcome a number of challenges (see figure 2). Action must be taken to ensure the adoption and implementation of clinical guidelines and WHO standards on comprehensive abortion care, to continue the trend of task-shifting abortion provision to a wider range of medical personnel and to promote the correct use of medication abortion. Also critical is the provision of postabortion care, training for a range of providers, and procurement of recommended equipment and supplies to manage complications. Taking these actions is not just a matter of public health, but is cost-effective as well. Studies estimate that the annual cost of postabortion care in developing countries is $232 million; by contrast, it would cost $20 million to provide all abortions safely.17
Many of these steps are impeded by restrictive abortion laws that outright prohibit abortion or create a chilling effect that hinders women’s ability to access safe abortion services. Until abortion is legal for all women, clandestine and frequently unsafe abortions will continue to be a public health issue, often concentrated among poor women who do not have the resources to locate, travel to and afford trained providers. Policymakers and civil society actors alike must prioritize abortion law reform as a necessary precondition for addressing unsafe abortion. In legally restrictive settings, public health officials must do a better job of disseminating information about permitted indications for abortion and ensuring that women can obtain an abortion that meets the specified criteria in a timely manner. In settings where misoprostol is increasingly used, women must have better access to information on its correct use and anticipated side effects.
Whether abortion is legal or illegal, much more needs to be done to reduce stigma through public education campaigns and provider training on nonjudgmental care and treatment. Combatting stigma is especially important for younger women and unmarried women, who may face higher barriers to accessing sexual and reproductive health services than their older and married counterparts. Finally, governments, donors and providers must work on the main driver of abortion by increasing access to information, counseling and contraceptive services to help more women prevent unintended pregnancies.
Until recently, the United States recognized the importance of supporting family planning programs in its foreign aid as the world’s leading donor for overseas family planning assistance. Under the Trump administration, however, that leadership has been eviscerated and replaced by a hostile and destructive agenda to undermine sexual and reproductive health and rights. Building on long-standing policies such as the Helms Amendment, which restricts U.S. foreign aid for abortion, the Trump administration has gone further—defunding UNFPA and imposing an expanded global gag rule that prohibits U.S. global health funds from going to any foreign nongovernmental organizations that use their own funds to advocate for or provide abortion services. Going beyond any previous conservative administration, the Trump administration proposed in its fiscal year 2018 budget to completely eliminate funding for international family planning—the very thing that would help prevent abortions in the first place—and to slash it by half in its fiscal year 2019 budget.
These steps will affect millions of women in developing countries. Poor women, who are most at risk of unintended pregnancies and unsafe abortions, will be the ones who suffer the most. At this critical time when hard-fought gains to women’s health are in peril, it is more important than ever for other donors, governments and civil society actors to rally around abortion rights and commit to an evidence-based and human rights–oriented approach to protecting women’s health—including by working to prevent unsafe abortion.