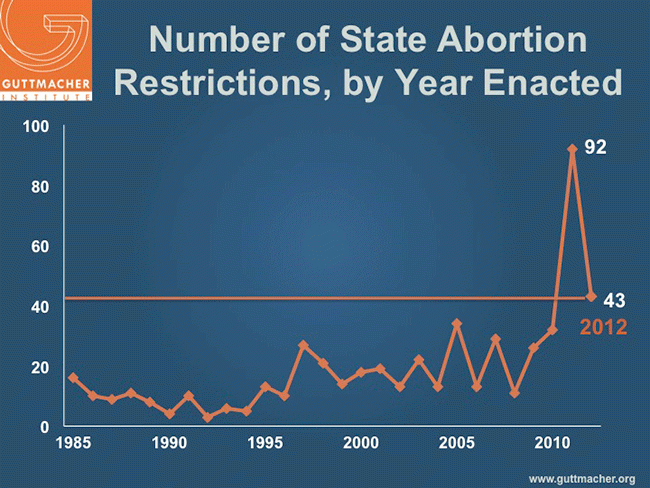
Reproductive health and rights was once again the subject of extensive debate in state capitols in 2012. Over the course of the year, 42 states and the District of Columbia enacted 122 provisions related to reproductive health and rights. One-third of these new provisions, 43 in 19 states, sought to restrict access to abortion services. Although this is a sharp decrease from the record-breaking 92 abortion restrictions enacted in 2011, it is the second highest annual number of new abortion restrictions.
(Note: This analysis refers to reproductive health and rights-related “provisions,” rather than bills or laws, since bills introduced and eventually enacted in the states contain multiple relevant provisions.)
Against the backdrop of a contentious presidential campaign in which abortion and even contraception were front-burner issues —to a degree unprecedented in recent memory—supporters of reproductive health and rights were able to block high-profile attacks on access to abortion in states as diverse as Alabama, Idaho, Minnesota, Pennsylvania and Virginia. Similarly, the number of attacks on state family planning funding was down sharply, and only two states disqualified family planning providers from funding in 2012, compared with seven in 2011. That said, no laws were enacted this year to facilitate or improve access to abortion, family planning or comprehensive sex education.
Abortion
Twenty-four of the 43 new abortion restrictions were enacted in just six states. Arizona led the way, enacting seven restrictions; Kansas, Louisiana, Oklahoma, South Dakota and Wisconsin each enacted at least three. Although some of the most high-profile debates occurred around legislation requiring that women seeking an abortion be required to first undergo an ultrasound or imposing strict regulations on abortion providers, most of the new restrictions enacted in 2012 concerned limits on later abortion, coverage in health exchanges or medication abortion.
Mandating Non-Medically Necessary Procedures Prior to Abortion
At the beginning of 2012, it appeared that a number of states were poised to require a woman seeking an abortion to first undergo an ultrasound. Mandatory ultrasound provisions are intended to convince a woman to continue her pregnancy to term and require a provider to perform an ultrasound even when one is not medically necessary. In fact, by March, ultrasound requirements were introduced in 10 states. However, in February, a firestorm erupted in Virginia when it became known that the proposed mandate would, in practice, necessitate performance of a transvaginal ultrasound. The controversy not only led to passage of a somewhat weaker requirement in Virginia but also is widely seen as having blunted efforts to mandate ultrasound in Alabama, Idaho and Pennsylvania. With the addition of Virginia, eight states require an ultrasound prior to receiving an abortion (see Requirements for Ultrasound).
The new law in Virginia also requires providers to give women the option to hear a fetal heartbeat in advance of having an abortion. In addition, laws adopted in Louisiana and Oklahoma require abortion providers to make the fetal heartbeat audible to the woman prior to an abortion.
Targeted Regulation of Abortion Providers (TRAP)
In 2012, Arizona, Michigan and Virginia took steps to establish stringent regulations that affect only surgical and medication abortion providers, but not other providers of outpatient surgical and medical care. A law enacted in Arizona requires the state health department to develop regulations that include rules on follow-up procedures after a medication abortion, requirements for reporting abortion complications and penalties for noncompliance. In Michigan, legislation enacted at the very end of the year directs the state health department to develop regulations that will require providers that perform at least 120 abortions per year to meet the same architectural and licensing requirements as ambulatory surgical facilities. In Virginia, Gov. Bob McDonnell approved regulations requiring all abortion clinics performing at least five procedures a month to meet the same architectural standards as hospitals; the panel had initially attempted to “grandfather in” existing clinics and apply the rules only to new clinics. The regulations now go to the Board of Health for final review.
An attempt to adopt stringent regulations for abortion clinics in Minnesota failed when Gov. Mark Dayton vetoed a measure that would have imposed requirements on abortion providers’ facilities, but not other similar outpatient health care facilities.
Hospital Privileges
Legislation to require abortion providers to have hospital admitting privileges was introduced in five states and enacted in three; this provision is not mandated for other outpatient surgical and medical providers. In the most stringent of the new laws, the provision enacted in Mississippi requires abortion providers to have admitting privileges at a local hospital and to be certified in obstetrics and gynecology or eligible for certification. As soon as the restriction was signed into law, the state’s sole abortion clinic filed a legal challenge. In July, a U.S. district court judge ordered that the clinic be given time to apply for hospital privileges. By December, when all local hospitals had refused privileges to the clinic’s providers, the agency once again asked the court to enjoin enforcement so the clinic can remain open.
The provision adopted in Arizona requires providers of surgical abortion to have admitting privileges at a hospital within 30 miles and medication abortion providers to have privileges at a hospital within the state. The new restriction in Tennessee requires providers to have admitting privileges either within the county or in an adjacent county.
Later Abortion
Arizona, Georgia and Louisiana enacted measures to ban abortion prior to fetal viability in direct conflict with U.S. Supreme Court decisions. Moreover, the exceptions contained in these restrictions do not allow for an abortion when necessary to protect a woman’s health, as required by the Court. Of the three new provisions, only the Louisiana restriction is fully in effect. It bans abortion at 20 weeks postfertilization (22 weeks after the woman’s last menstrual period or LMP). The Georgia provision is partially in effect, a state court has ruled that the restriction can only be enforced on abortions after viability. Both allow exceptions to protect the woman’s life, avert substantial and irreversible” damage to the woman's physical health or terminate a pregnancy that has been diagnosed as “medically futile.” Arizona’s provision prohibits abortion at 18 weeks postfertilization (20 weeks LMP); enforcement of the restriction has, so far, been blocked by the ninth U.S. Circuit of Appeals. Aside from the disputed Arizona and Georgia provisions, seven states ban abortion at 20 weeks postfertilization (see State Policies on Later Abortions).
In addition, the New Hampshire legislature overrode Gov. John Lynch’s veto to approve a restriction on “partial-birth” abortion. The provision parallels the restrictive federal standard and bans the procedure before viability, even when the woman’s health is endangered. When the provision goes into effect in 2013, 19 states will have bans on “partial-birth” abortion (see Bans on “Partial-Birth” Abortion).
Abortion Coverage
Four states enacted provisions banning abortion coverage in the insurance exchanges being established under the Affordable Care Act. Provisions enacted in Alabama, South Carolina and Wisconsin permit coverage of an abortion in cases of life endangerment, rape or incest. Alabama also permits coverage in the case of ectopic pregnancy, and Wisconsin permits it when a woman’s physical health is at serious risk. South Dakota permits coverage only in cases of life endangerment and the risk of “substantial and irreversible impairment of a major bodily function.” At the very end of the year, Michigan Gov. Rick Snyder vetoed legislation that would have prohibited coverage of abortion in plans in the Exchange as well as all private health plans, except when the woman’s life is endangered. The addition of these four states brings to 20 the number of states restricting abortion coverage available through state insurance exchanges (see Restricting Insurance Coverage of Abortion). These restrictions limit a woman’s ability to obtain a health care plan that provides for her reproductive health care needs and treats abortion as separate from other health care services.
In addition, the Missouri legislature overrode Gov. Jay Nixon’s veto of a bill that allows any employer to refuse to cover abortion services. It also allows individuals to refuse to purchase coverage including abortion when offered by their employers. Existing state law permits abortion coverage only when a woman’s life is endangered.
South Carolina amended the long-standing requirement that the state employees’ health plan may cover abortion only when necessary to save the woman’s life or in cases of rape or incest. The new provision permits taxpayer dollars to be used to pay for abortions only in cases of life endangerment; the cost in cases of rape or incest must now be paid entirely from employees’ premiums.
Medication Abortion
In 2012, three states limited provision of medication abortion by prohibiting the use of telemedicine, which is becoming a routine part of health care, particularly in rural areas. Michigan, Oklahoma and Wisconsin enacted provisions requiring that the physician prescribing the medication for the abortion be in the same room as the patient, bringing to seven the number of states that prohibit the use of telemedicine (see Medication Abortion). A similar limitation was vetoed by Minnesota Gov. Mark Dayton.
In addition, Arizona enacted a provision that requires mifepristone to be provided in accordance with an outdated FDA protocol rather than a simpler, long-standing evidence-based protocol that is equally safe and effective with fewer side effects. Arizona joins Ohio in requiring use of the FDA protocol.
Tennessee enacted a provision that moves up the effective date of its telemedicine ban from January 2013 to July 2012. In addition, the Wisconsin restriction also explicitly limits the provision of medication abortion to physicians, a move that essentially restates existing law.
Mandatory Counseling and Waiting Periods
South Dakota and Arizona enacted provisions requiring a woman seeking an abortion to obtain counseling that includes inaccurate or irrelevant information. Arizona’s provision requires the state health department to develop counseling materials that include information on coerced abortion and the “possible detrimental psychological effects of abortion.” It also requires a woman seeking an abortion because of fetal impairment to receive counseling on living with those conditions and the availability of perinatal hospice care if the impairment will be fatal.
South Dakota amended counseling requirements that were enacted in 2011 but whose implementation was blocked by a legal challenge. The new provision requires abortion counseling to include information on any research showing that some women (based on their “physical, psychological, demographic or situational” characteristics) may be at higher risk of negative mental health outcomes associated with an abortion. Including the new requirements in South Dakota and Arizona, 18 states require that women seeking an abortion be given misleading information (see Counseling and Waiting Periods for Abortion).
The new provisions in South Dakota and Arizona also require abortion providers to assess whether women seeking an abortion have been subject to coercion. In addition, a new provision enacted in Wisconsin requires state-mandated abortion counseling materials to contain information on domestic violence. Including these three new provisions, 14 states require that information on coercion be part of abortion counseling
Finally, the new ultrasound mandate in Virginia also requires that women who live less than 100 miles from the clinic undergo the ultrasound 24 hours in advance of the abortion (see “Mandating Medical Procedures Prior to Abortion,” above). Although Virginia law already required a 24-hour waiting period, this new provision compels women to make two trips to the clinic before receiving an abortion. Including the new mandate in Virginia, 10 states now have laws that necessitate a woman to make two trips (see Counseling and Waiting Periods for Abortion). Also in 2012, Utah increased the length of its mandated waiting period from 24 to 72 hours.
Parental Involvement
Three states adopted requirements that either mandate parental involvement or make it more cumbersome for a minor to use the judicial bypass procedure to obtain an abortion in the absence of parental involvement. Voters in Montana approved a ballot initiative requiring the parents of a minor under 16 to be notified prior to an abortion; this measure replaces an existing state law that had been blocked in court. Additionally, New Hampshire enacted a provisions that extends the time a court may deliberate on a judicial bypass request from 48 hours to two business days and Ohio now limits the courts where a minor may seek a bypass of the parental consent requirement. Including Montana, New Hampshire and Ohio, 38 states require parental involvement in a minor’s decision to have an abortion (see Parental Involvement in Minor’s Abortions). Research has found that minors typically involve a parent when deciding to obtain an abortion and many of those who do not talk to their parents report they would experience physical violence or abuse if their parents knew.
A new provision enacted in Mississippi requires a physician performing an abortion on a minor younger than 14 to provide a tissue sample to the state bureau of investigation. It also includes criminal penalties for anyone assisting a minor in seeking an abortion in violation of the state’s parental consent requirement.
Other Restrictions
Eight states adopted other measures related to abortion, including provisions that:
- allow a medical professional in Arizona to withhold from a woman information about her pregnancy that could prompt her to obtain an abortion;
- prohibit state employees or state agencies in Kansas from participating in or facilitating abortion care;
- permit a woman in Oklahoma, or the parent or legal guardian of a minor in the state, to sue if there was a violation of the state’s abortion restrictions;
- require abortion providers in Georgia to report a diagnosis when an abortion is performed at or beyond 20 weeks’ gestation;
- continue existing restrictions on public funding for abortion in Iowa and Maryland;
- authorize the sale of “Choose Life” license plates in Alaska; and
- clarify long-standing policy in Louisiana limiting the performance of an abortion to physicians licensed in Louisiana.
Family Planning
Family Planning Funding
Family planning programs largely escaped steep budget cuts in 2012. Of the 19 states in which funding decisions were made through the legislative budget process, family planning funds were the subject of steep cuts only in Maine, where funding was slashed by 25%. This is in sharp contrast to 2011, when funds were cut by more than half in Montana, New Hampshire and Texas.
In New Jersey, however, family planning funds were cut drastically in 2010. Gov. Chris Christie vetoed a provision this year that would have reinstated $7.5 million in family planning funds and directed the state to expand Medicaid funding of family planning.
Restrictions on Family Planning Providers
Similarly, fewer states moved to disqualify certain family planning providers from eligibility for funding than in 2011. In 2011, seven states (Kansas, Wisconsin, North Carolina, New Hampshire, Tennessee, Indiana and Texas) moved to enact new restrictions on eligibility for family planning grant funds, often including both state funds and federal funds that flowed from the state treasury to providers (See Laws Affecting Reproductive Health and Rights: 2011 State Policy Review). Although most of these restrictions remain in effect, only two states added new restrictions in 2012.
Arizona and North Carolina effectively barred family planning clinics not operated by health agencies from being eligible for family planning grant funds; in practice, these restrictions affect only clinics operated by Planned Parenthood affiliates. The Arizona provision limits state family planning dollars to health departments, hospitals, federally qualified health centers and other primary care providers. In North Carolina, the legislature overrode Gov. Beverly Perdue’s veto of a provision directing all family planning funds to local health departments. These changes bring to nine the number of states that restrict access to family planning funds (see State Family Planning Funding Restrictions). (The Kansas budget bill continued a restriction, first adopted in 2011, that excludes family planning clinics from being able to receive any of the federal Title X funds that flow through the state; the provision is enjoined pending resolution of a court case.)
In addition, Arizona moved to bar organizations that provide abortion services, except in cases of life endangerment, rape or incest, from being able to participate in the state’s Medicaid program. The provision has been blocked by a federal district court, on the grounds that it conflicts with federal Medicaid requirements. In 2011, similar laws were enacted in Indiana and Texas. The Indiana law remains enjoined.. In the latest twist in a complicated legal battle, a federal judge on December 31, 2012 refused to block enforcement of the Texas restriction.
In a move closely related to Medicaid, a state court permanently enjoined a Montana statute prohibiting the state’s Children’s Health Insurance Program from covering contraceptives.
Insurance Coverage of Contraceptive Services
Provisions relating to contraceptive coverage mandates—and specifically which employers may refuse such coverage—were introduced in eight states and enacted in two. For several years, Arizona had allowed only churches to opt out of the state’s contraceptive coverage mandate; in 2012, it expanded the exemption to permit any employer or plan enrollee to opt out based on their religious belief. A Missouri law enacted over Gov. Jay Nixon’s veto reiterates long-standing policy allowing employers, insurers or enrollees to opt out of the state’s contraceptive coverage mandate because of a religious objection, but attempts to expand it by incorporating an exemption from the federal mandate included in the Affordable Care Act (ACA). At the tail end of the year a federal district court blocked enforcement of the provision citing potential conflict with the ACA. Including Arizona , eight states have an “expansive” exemption to their contraceptive coverage mandates (see Insurance Coverage of Contraceptives).
Adolescents and Sex Education
Between 2007 and 2010, seven states enacted legislation related to sex education, and all but one expanded access to comprehensive sex education or added requirements that the sex education provided be medically accurate. Over the past two years, however, five states enacted legislation, and all but one supported abstinence-only education.
Tennessee enacted a provision requiring all sex education offered in the state to “exclusively and emphatically” teach abstinence. The education must include information on the consequences of “nonmarital” sex and may not promote any activity that could lead to “nonabstinent behavior.” In addition, instruction may discuss contraception only if it does not promote sex among unmarried students and informs them that contraception does not eliminate the risk of pregnancy and STIs.
An abstinence education provision enacted in Wisconsin effectively guts the state’s 2010 comprehensive sex education mandate. It removes requirements that information provided in sex education classes be medically accurate and that it include education on contraception. It also requires the instruction to stress the importance of abstinence before marriage.
An extreme provision that would have required school-based sex education to focus exclusively on abstinence and block the inclusion of information on contraceptives, sex outside of marriage or homosexuality was vetoed by Utah Gov. Gary Herbert. With these changes, 26 states stress abstinence in sex education (see Sex and HIV Education). A provision enacted in Oregon mandates that sex education provided in the state include information on teen dating violence prevention.
In a provision not related to sex education but to adolescents more broadly, Georgia enacted a provision expanding the list of individuals and organizations required to report suspected instances of statutory rape to include employees or volunteers of organizations that provide reproductive health services.
Sexually Transmitted Infections
In 2012, Arkansas and Idaho expanded access to treatment for STIs. Both states enacted provisions allowing medical providers to treat a patient’s partner for chlamydia and gonorrhea without having seen the partner. The Arkansas regulation limits such treatment to heterosexual partners. The addition of these two states brings to 26 the number of states that explicitly permit treatment of a patient’s partner (see Partner Treatment for STIs).
Pregnancy and Birth
Ten states and the District of Columbia enacted new provisions related to pregnancy and birth this year. Three of these states and the District of Columbia addressed issues related to substance abuse and pregnancy. Colorado adopted a provision prohibiting substance abuse discovered through prenatal care from being used in a criminal prosecution. Kentucky allocated $1.4 million for substance abuse prevention and treatment for pregnant women. The District of Columbia enacted a provision requiring a health care provider to report to child services when an infant is diagnosed with fetal alcohol spectrum disorder. Finally, Oklahoma mandated that if a newborn tests positive for controlled substances, an investigation must be conducted to determine whether child abuse or neglect has occurred. With these additions, 37 states and the District of Columbia have policies related to substance abuse and pregnancy (see Substance Abuse During Pregnancy).
Two states expanded HIV testing of pregnant women. A provision enacted in Delaware requires a health care provider to offer HIV testing to a pregnant woman whose HIV status is unknown when she enters the third trimester or during labor and delivery; the woman may refuse the test. A regulation adopted in West Virginia requires HIV screening of pregnant women in the routine panel of prenatal tests, unless the woman declines; it also allows an HIV test to be performed on an infant born to a mother who has not been tested for HIV.
Four additional states enacted provisions that:
- allow a certificate of stillbirth to be issued in Iowa to a parent in the case of a miscarriage that occurs after "20 completed weeks" of pregnancy;
- revise the Tennessee homicide statute to include an embryo or fetus at any point in gestation as a victim; and
- allow emergency services personnel in Minnesota to accept a relinquished infant who is seven days old or younger, and permit a parent relinquishing a newborn in Mississippi to remain anonymous.
Environmental Exposure to Reproductive Toxins
Six states and the District of Columbia enacted provisions related to reproductive health and exposure to harmful substances such as lead, mercury, Bisphenol-A (BPA) and pesticides. Provisions to protect children from lead exposure were enacted in Louisiana and Nebraska. In contrast, Vermont amended its law to no longer require testing for lead levels in food and vitamins.
Three states took steps to keep mercury out of the environment by requiring recycling of mercury-containing thermostats (Connecticut), prohibiting the sale of batteries commonly used in hearing aids and cameras (Illinois) and limiting the amount of mercury in fluorescent light bulbs (Oregon).
Finally, a new Illinois provision bans the use of BPA in reusable bottles and cups for young children, and the District of Columbia enacted a provision requiring the development of regulations prohibiting the use of pesticides near most schools and child-occupied facilities.