- Abortion was legalized in Nepal in 2002. It is available up to 12 weeks’ gestation on request, up to 18 weeks’ gestation in cases of rape or incest, and at any time if the pregnancy poses a danger to the woman’s life or physical or mental health or if there is a fetal abnormality.1
- Abortion legalization has contributed to a sharp decline in maternal mortality, which fell from 580 maternal deaths per 100,000 live births in 1995 to 190 per 100,000 in 2013.2
- Many women in Nepal continue to face barriers to obtaining safe and legal procedures. Obstacles include lack of awareness of the legal status of abortion, lack of services, lack of transport to approved facilities, gender norms that hinder women’s decision-making autonomy, the often-prohibitive cost of the procedure and fear of abortion-related stigma.3,4,5
Abortion incidence
- An estimated 323,000 abortions were performed in Nepal in 2014. This number translates to a rate of 42 abortions per 1,000 women aged 15–49.
- Nepal’s 2014 annual abortion rate falls between the rates estimated for nearby Bangladesh (37 per 1,000) and Pakistan (50 per 1,000).
- Nationwide, fewer than half (42%) of all abortions were provided legally in government-approved facilities. The remainder (58%) were clandestine procedures provided by untrained or unapproved providers or induced by the pregnant woman herself.
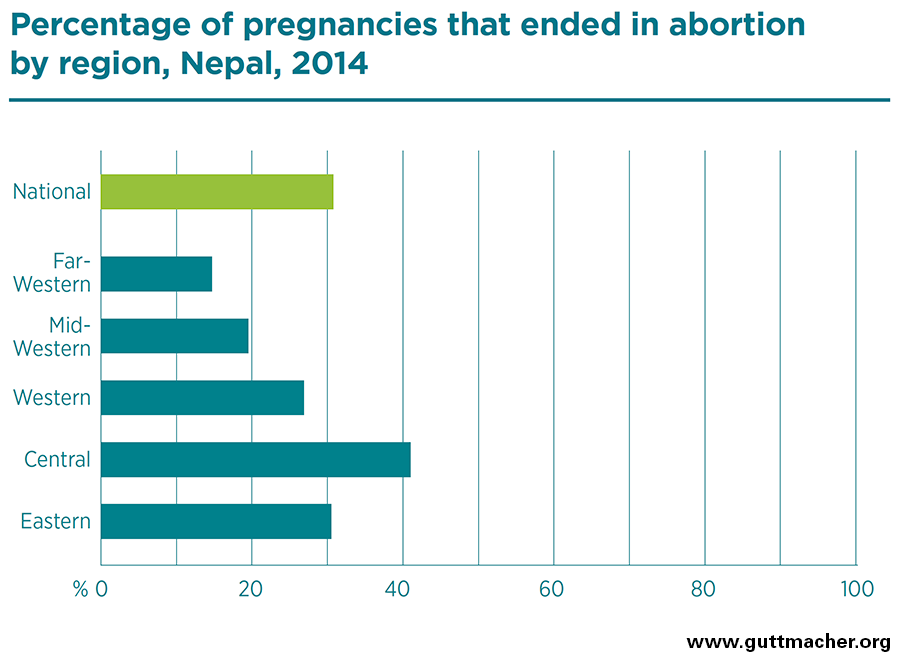
- Within Nepal, abortion rates for 2014 varied widely by development region, from 21 per 1,000 reproductive-age women in the Far-Western development region to 59 per 1,000 in the more urban Central development region, which includes the capital city of Kathmandu.
- Several factors may explain the high abortion rate in the Central region. Compared with women and couples in other regions, those in or near the capital may have a greater desire for smaller families, higher risk of unintended pregnancy (because of later marriage and greater occurrence of premarital sex) and better access to services. In addition, women from neighboring areas obtain services in the Central region.6,7
Provision of abortion and postabortion care
- Some 1,100 government-approved health facilities provided legal abortion, postabortion care or both in Nepal in 2014.
- Thirty-seven percent of the estimated 137,000 legal abortions were performed in public-sector facilities, 34% in NGO facilities and 29% in private-sector facilities.
- An estimated 80,000 women were treated in health facilities in 2014 for complications related to abortion and miscarriage. Sixty-eight percent of these women had complications that resulted from a clandestine abortion.
- Forty-four percent of women receiving postabortion care were treated in private facilities, 41% in public facilities and 15% in NGO facilities.
- Out of every 1,000 women of childbearing age in Nepal, eight were treated for complications of illegal or legal abortions in 2014. Pakistan had a higher treatment rate (14 per 1,000) and Bangladesh a slightly lower one (seven per 1,000).
- Regional treatment rates for complications ranged from 1.8 per 1,000 in the Far-Western region to 11.3 per 1,000 in the Central region.
Incidence of unintended pregnancy
- In 2011, 43% of married women in Nepal used a modern method of contraception. However, half of contraceptive users discontinued use within 12 months of starting.8
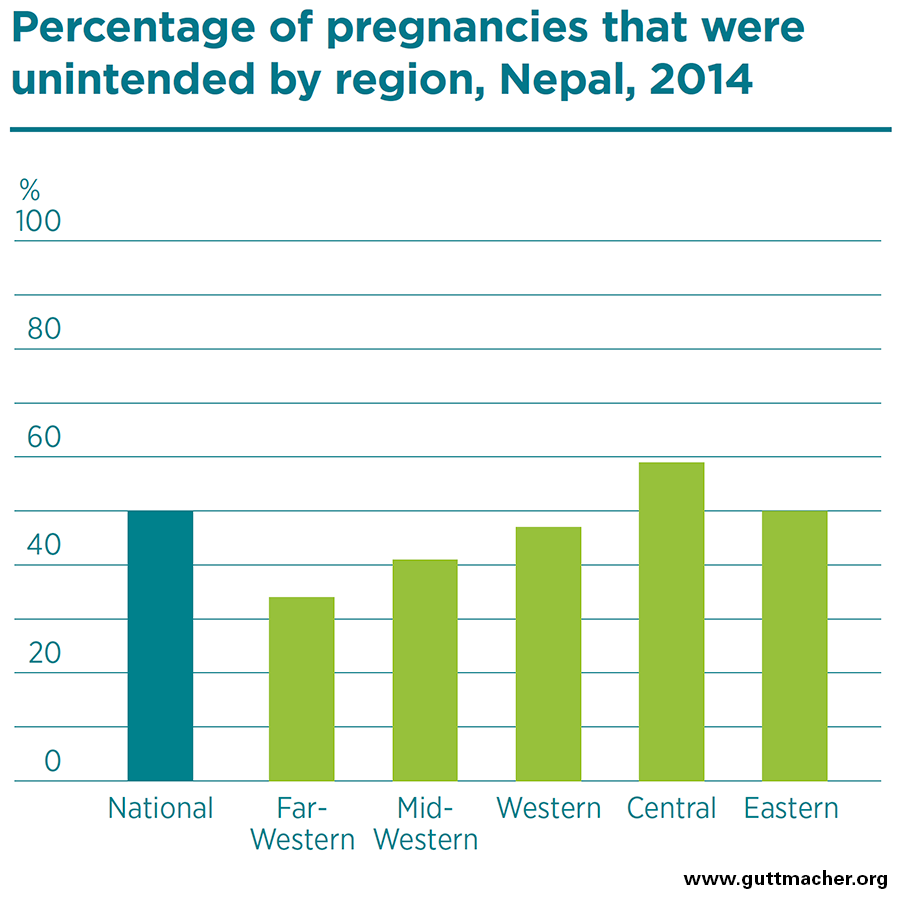
- The unintended pregnancy rate for Nepal was 68 per 1,000 women of reproductive age in 2014. It ranged from 47 per 1,000 women in the Far-Western region to 85 per 1,000 in the Central region.
- Half of pregnancies were unintended (either mistimed or unwanted), and close to one-third (31%) of all pregnancies ended in abortion.
Strategies for reducing unsafe abortions
- Reduce levels of unintended pregnancy and resulting abortions by increasing access to high-quality family planning services, including counseling and the provision of a range of methods.
- Expand free or low-cost abortion services, and ensure implementation of the government policy to provide free abortion services at public facilities.9
- Reduce women’s recourse to clandestine procedures by disseminating information about the legal status of abortion and where to obtain legal abortion services.
- Expand access to safe and legal abortion, especially in remote areas, by accrediting health posts, primary health centers, and private and NGO facilities, and equipping them with a provider trained in medication abortion.10,11
In 2014, the Center for Research on Environment Health and Population Activities (CREHPA) and the Guttmacher Institute conducted a study to generate the first national and regional estimates of abortion incidence in Nepal. This study adopted a modified version of the established Abortion Incidence Complications Methodology, which uses indirect estimation techniques to measure the number of abortions occurring each year, the abortion rate and the abortion ratio. The study, which produced most of the data in this fact sheet, consisted of a survey of a nationally representative sample of facilities that provide safe abortion or postabortion services, and a survey of experts on abortion in Nepal.