Meeting adolescents’ needs for contraceptive services is a critical health and development goal and helps enable adolescents to control whether and when they become pregnant and have children. About half of pregnancies among adolescent women (defined as those aged 15–19) in developing regions are unintended, and more than half of these end in an induced, and often unsafe, abortion.
- In 2017, about nine in 10 adolescent women using modern contraceptives* in developing regions relied on short-acting methods. Fewer than one in 10 used long-acting, reversible contraceptives (LARCs), although usage varied by subregion. As adolescent women increasingly attain more schooling and delay the start of childbearing, there is potential for more demand for LARCs.
- This fact sheet presents four scenarios of adolescent contraceptive use through 2030, the target year of the United Nations Sustainable Development Goals and the Global Strategy for Women’s, Children’s and Adolescents’ Health. These scenarios highlight the potential impact and costs associated with overall increased contraceptive use among adolescent women and an increased use of LARCs, specifically.
- All four scenarios account for projected changes in the number of adolescent women, the number who are married or cohabiting, and the number of adolescent women using modern contraception.
Scenario 1 uses the most likely level of modern contraceptive method use to be reached or surpassed in a particular year (2020, 2025 or 2030). It assumes that the current 2017 mix of modern contraceptive methods used by adolescent women would remain the same over time.
Scenario 2 uses the same level of projected growth in modern contraceptive use as scenario 1, but assumes 20% of users of short-acting methods would shift to using LARCs, compared with the method mix in 2017.
Scenario 3 assumes that 50% of the number of adolescent women using traditional methods and 50% of the number of adolescent women who want to avoid pregnancy and are not using any form of contraception would instead use modern contraceptive methods. It also assumes that the current 2017 mix of modern contraceptive methods used by adolescent women would remain the same over time.
Scenario 4 uses the accelerated growth in modern contraceptive method use outlined in scenario 3, but assumes a 20% shift away from short-acting methods to LARCs, compared with the method mix in 2017.
LIKELY FUTURE GROWTH
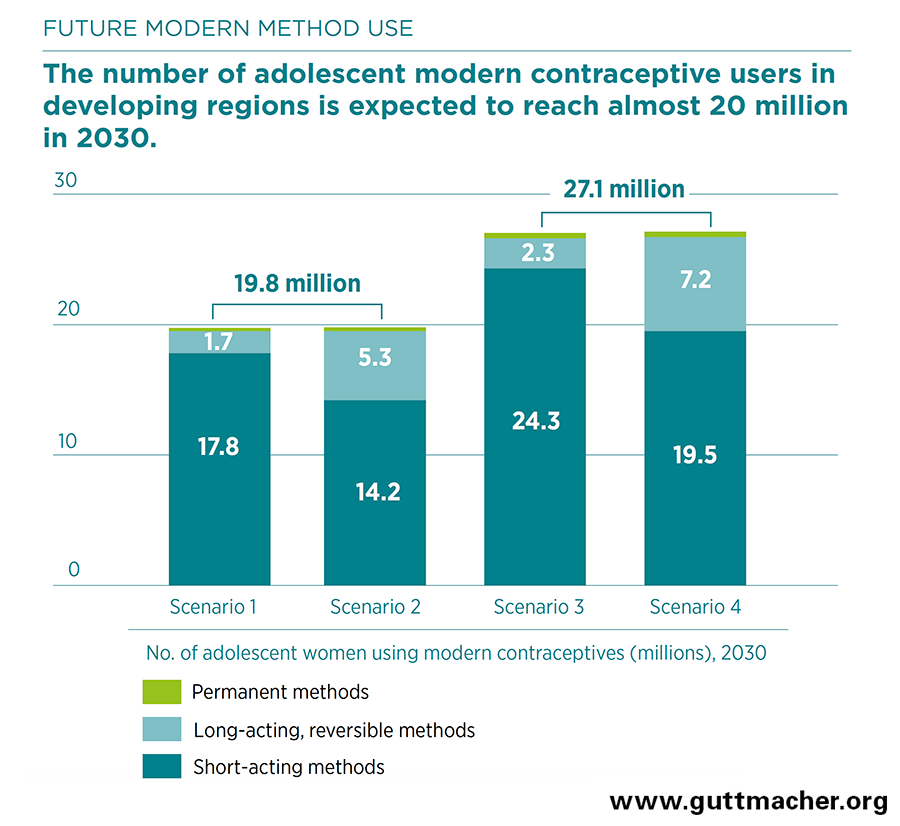
- Scenarios 1 and 2 project that the number of adolescent women using modern contraceptives in developing regions would increase from an estimated 17.0 million in 2020 to 18.3 million in 2025 and to 19.8 million in 2030.
- In scenario 1, the mix of modern contraceptive methods would be the same as in 2017, and there would be 17.8 million adolescents in developing regions using short-acting methods and 1.7 million using LARCs in 2030. If 20% of adolescent women using short-acting methods were to choose LARCs instead (scenario 2), LARC users would number more than five million in 2030.
- Under these scenarios, about 57% of adolescent women in developing regions in 2030 would have their need for modern contraception met—52% in Africa, 59% in Asia, and 67% in Latin America and the Caribbean.
- For scenario 1, the total annual cost of services for the projected 19.8 million adolescent women who would be using modern contraceptives in developing regions in 2030 would be an estimated $310 million.† The cost would be lower, at $275 million, under scenario 2’s assumption of increased LARC use.
- By 2030, scenario 1 would result in an estimated 7.1 million unintended pregnancies averted per year. Because LARCs are highly effective, scenario 2 would result in the prevention of an additional 300,000 unintended pregnancies.
- Even with the levels of growth in modern method use projected in these scenarios, nearly 15 million adolescent women in developing regions would have an unmet need for modern contraception in 2030. Women with an unmet need for modern contraception are those who want to avoid pregnancy but are not using a modern contraceptive method.
ACCELERATED GROWTH
- Scenarios 3 and 4 assume accelerated growth in modern contraceptive use among adolescent women in developing regions: The number of users would reach 27.1 million in 2030—7.3 million more than in the first two scenarios.
- The proportion of adolescent women in developing regions whose need for modern contraception would be met would rise to 79% in developing regions (76% in Africa, 80% in Asia, and 84% in Latin America and the Caribbean).
- Under scenario 3, services for 27.1 million modern method users in 2030 would cost an estimated $412 million. The cost would be $365 million under scenario 4’s assumption of increased LARC use.
- Scenario 3 would result in an estimated 9.6 million unintended pregnancies averted, and scenario 4 would avert an additional 400,000.
MOVING FORWARD
- Understanding future trends in adolescent contraceptive use can help governments anticipate pressures on domestic budgets, donors plan future investments, and policymakers and program managers keep pace with adolescents’ needs.
- Contraceptive services must be structured in such a way as to ensure that adolescents can make free and informed choices from among a wide range of contraceptive options, including highly effective LARC methods. They must also have access to services for removing these methods when they choose.
- The scenarios of future contraceptive use presented here make a robust case for investing in contraceptive services for adolescents now.