Incidence and trends
- During 2010–2014, an estimated 8.2 million induced abortions occurred each year in Africa. This number represents an increase from 4.6 million annually during 1990–1994, mainly because of an increase in the number of women of reproductive age.
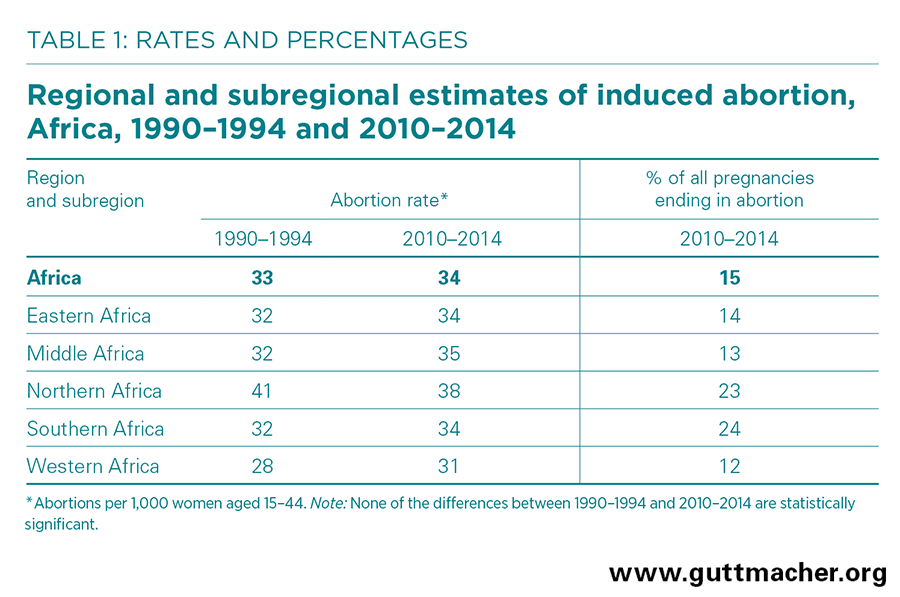
- The annual rate of abortion for the region is an estimated 34 per 1,000 women of reproductive age (15–44), and remained more or less constant between 1990–1994 and 2010–2014.
- The regional abortion rate is roughly 26 per 1,000 for married women and 36 per 1,000 for unmarried women.1
- As of 2010–2014, the annual abortion rate varies slightly by subregion, ranging from 31 per 1,000 women of reproductive age in Western Africa to 38 per 1,000 in Northern Africa; rates in Eastern, Middle and Southern Africa are close to the regional average of 34 per 1,000.
- The proportion of all pregnancies in Africa ending in abortion each year, estimated at 15% in 2010–2014, has changed little since 1990–1994.1
- The proportion of pregnancies ending in abortion ranges from 12% in Western Africa to 24% in Southern Africa; rates in Middle, Eastern and Northern Africa are 13%, 14% and 23%, respectively.
Legal status of abortion
- An estimated 93% of women of reproductive age in Africa live in countries with restrictive abortion laws (i.e., countries in the first four categories in Table 2). Even in countries where the law allows abortion under limited circumstances, it is likely that few women are able to obtain a safe, legal procedure.2
- Abortion is not permitted for any reason in 10 out of 54 African countries.
- Four countries in Africa have relatively liberal abortion laws: Zambia permits abortion for health and socioeconomic reasons, whereas Cape Verde, South Africa and Tunisia permit abortion without restriction as to reason, with gestational limits.
Unsafe abortion and its consequences
- Induced abortion is medically safe when WHO-recommended methods are used by trained persons, less safe when only one of those two criteria is met, and least safe when neither is met. Many women in Africa undergo unsafe (i.e., less safe or least safe) procedures that put their well-being at risk.
- During 2010–2014, an average of about one in four abortions in Africa were safe. Of those that were unsafe, the majority fell into the least-safe category.
- In 2012, nearly seven per 1,000 women of reproductive age in Africa were treated for complications from unsafe abortion. In all, about 1.6 million women in the region are treated for such complications each year.3
- Africa is the world region with the highest number of abortion-related deaths. In 2014, at least 9% of maternal deaths (or 16,000 deaths) in Africa were from unsafe abortion.4
- The most common complications from unsafe abortion are incomplete abortion, excessive blood loss and infection.
- The poorest women with the fewest resources are the most likely to experience complications from unsafe abortion.
- Unsafe abortion has negative consequences beyond its immediate effects on individual women’s health. Treating complications increases the economic burden on poor families and incurs considerable costs to already struggling public health systems.
- The extent to which misoprostol is used to induce abortions in Africa is not known; however, the sale of misoprostol has increased in some African countries in recent years.5
Unintended pregnancy and unmet need
- As of 2017, about 58 million women of reproductive age in Africa have an unmet need for modern contraception—that is, they want to avoid a pregnancy but are either not practicing contraception or are using traditional methods, which are less effective than modern methods.6
- Most women who have an abortion do so because they become pregnant when they do not intend to. As of 2010–2014, the unintended pregnancy rate in Africa as a whole is 89 per 1,000 women aged 15–44; in Eastern Africa, the rate is 112 per 1,000 women.
- An estimated 21.6 million unintended pregnancies occur each year in Africa; of these, nearly four in 10 (38%) end in abortion.
Recommendations
- Programs and policies that improve women’s and men’s knowledge of, access to and use of contraceptive methods must be implemented to reduce unintended pregnancies—and the abortions or unplanned births that often follow.
- The provision and quality of postabortion care should be improved and expanded to reduce illness and death from unsafe abortion.
- The grounds for legal abortion in the region should be broadened and access to safe abortion services improved to reduce the number of clandestine procedures and the negative consequences that often result.
- Liberal abortion laws alone do not ensure the safety of abortions. Service provision guidelines must be adopted and disseminated, providers must be trained, and governments must be committed to ensuring that safe abortions are available.