A diverse network of health care providers in the United States use public funding to provide free or reduced-fee contraceptive care to millions of people who might not otherwise be able to afford it, including adolescents and those living with low incomes. This network of providers is made up of publicly supported clinics (health departments, Planned Parenthood affiliates, hospitals, federally qualified health centers and other independent organizations), as well as private providers who serve Medicaid enrollees. In addition to contraception, publicly supported clinics frequently provide patients with primary care and a range of other essential reproductive health services, such as STI testing and treatment, screening for breast and cervical cancer, and care related to pregnancy.1
Funding Through Medicaid and Title X
Public funding for family planning services is allocated through federal, state or local channels, primarily as part of Medicaid or the Title X family planning program. Medicaid is a jointly funded federal-state health insurance program for people living with low incomes and has historically accounted for the majority of US public expenditures on domestic family planning.2 Individuals who qualify for Medicaid insurance can use this coverage for family planning services and providers are reimbursed by Medicaid for contraceptive and related services delivered to enrollees.
Title X is a federally funded program that subsidizes services for low-income individuals who do not have any health insurance, or who choose not to use insurance for family planning services, by providing grants to statewide and local public health agencies and nonprofit organizations. Although this program accounts for a much smaller proportion of public spending on domestic family planning than Medicaid, Title X funds are critical to maintaining a network of sites that serve people who might not otherwise have access to sexual and reproductive health care.
Need for Publicly Supported Family Planning Services
Information on who may need contraceptive services is critical for the design and implementation of programs and policies that support access to care. For decades, the Guttmacher Institute has made periodic estimates of the need for contraceptives in the United States using a conventional metric based on women’s assumed risk for unintended pregnancy as a proxy for contraceptive need.3
In partnership with Dr. Anu Manchukanti Gomez at the University of California–Berkeley, and informed by the input of external stakeholders and experts, Guttmacher researchers developed a new metric of self-defined need for contraceptive services that adopts a more person-centered approach. This metric is based on women’s own reports of use of contraception or contraceptive services or a desire to use contraception for any reason over a one-year period.4,5 Using the new metric, Guttmacher researchers estimated the number of women with a self-defined need for contraceptive services and those who likely needed publicly supported contraceptive care in 2023.
- In 2023, there were 75.9 million US women* of reproductive age (15–49). Out of that total, 51.9 million were estimated to have a self-defined need for contraceptive services and supplies. Among them, 21.5 million were considered to have a likely need for publicly supported contraceptive services because they either had an income below 250% of the federal poverty level or were younger than 20.4
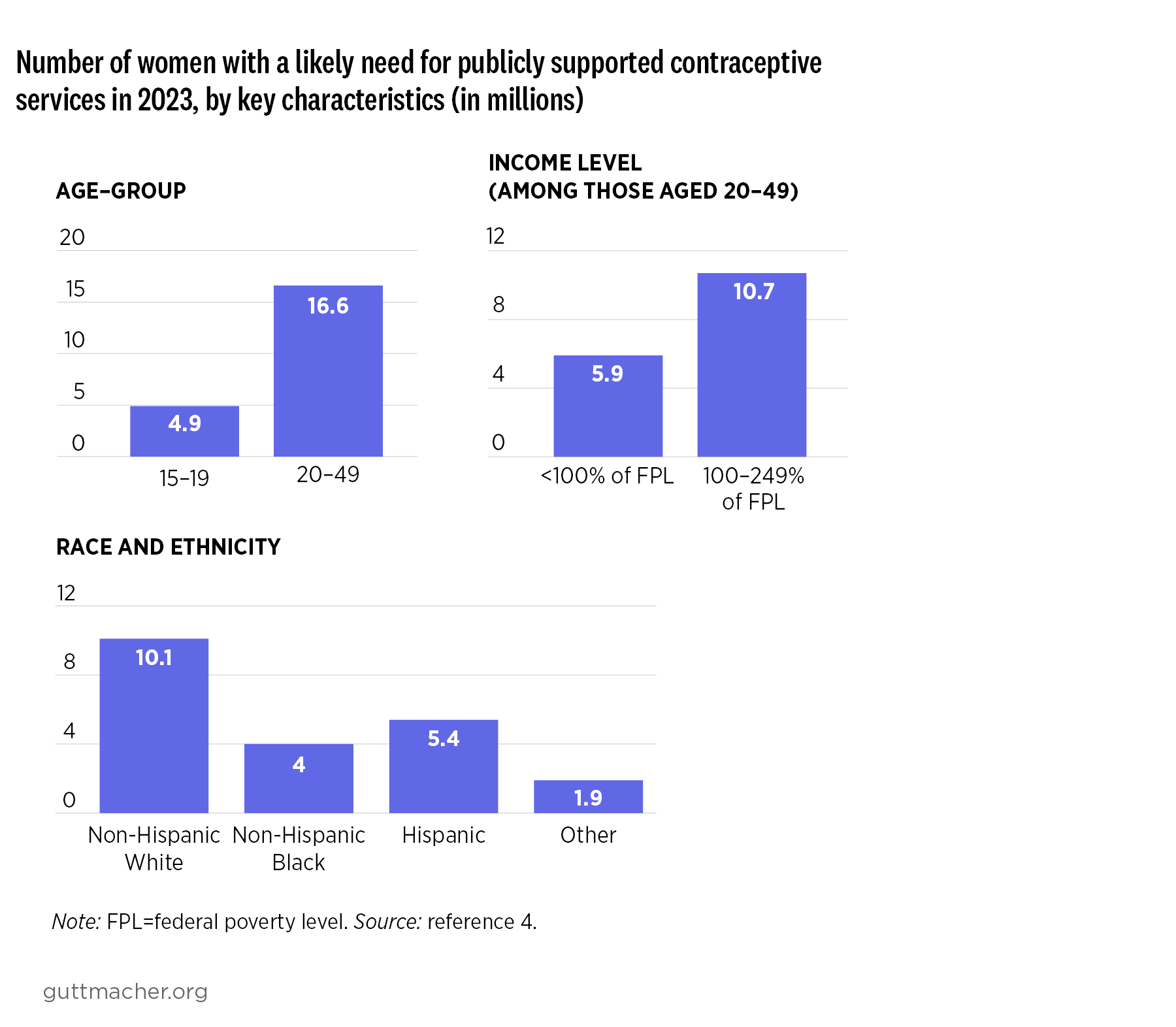
- Out of the 21.5 million women with a likely need for publicly funded family planning services, 77% (16.6 million) were adults with incomes below 250% of the federal poverty level and 23% (4.9 million) were younger than 20.4
Approximately 10.1 million of the women likely in need of publicly funded family planning services in 2023 were non-Hispanic White, 4.0 million were non-Hispanic Black, 5.4 million were Hispanic, and the remaining 1.9 million women reported being part of other or multiple racial and ethnic groups.4
Women Receiving Publicly Supported Family Planning Services
- In 2020 (most recent data available), 7.2 million women received publicly supported family planning services. Some 4.7 million got care from publicly supported clinics, and 2.5 million got care from private providers serving Medicaid enrollees.3
- The 7.2 million women who received publicly supported family planning services in 2020 represent 39% of those with a likely need for such services that year. Among the remaining 61% of women estimated to have a likely need for these services, some may have paid out of pocket or used private health insurance to cover care from sources that do not receive public support, such as pharmacies or private providers.3
- In 2020, 836,000 adolescent women younger than 20 received family planning services from publicly supported clinics.3
Types of Clinics Providing Publicly Supported Family Planning Services
- In 2020, 9,388 publicly supported clinics provided subsidized family planning services—5,429 (58%) were federally qualified health centers, 1,876 (20%) were health departments, 649 (7%) were hospital outpatient facilities, 600 (6%) were Planned Parenthood sites and 834 (9%) were other independent clinics.3
- Of the 4.7 million women who obtained contraceptive care from publicly supported clinics in 2020, 38% received services from federally qualified health centers, 33% from Planned Parenthood sites, 13% from health departments, 9% from hospital outpatient facilities and 7% from other independent clinics.3
Family Planning Services Offered
- In 2022–2023, about three-quarters of publicly supported clinics providing contraceptive care (73%) reported offering patients at least 10 of 14 reversible contraceptive methods.1
- Oral contraceptives, injectables (such as Depo-Provera) and condoms were offered by more than nine in 10 publicly supported clinics, and 79% offered emergency contraceptive pills.1
- Some publicly supported clinics focus primarily on reproductive health, and in 2022–2023, these clinics offered a greater range of contraceptive methods on-site and were more likely to have protocols to help patients initiate and continue using methods, compared with publicly supported clinics focused on primary care.1
- In 2022–2023, 25% of publicly supported clinics that provide family planning offered same-day appointments for an initial contraceptive visit (compared with 52% in 2015), and 39% of clinics offered some extended hours in the evenings or on weekends (compared with 42% in 2015).1
- Among all publicly supported clinics that offer contraception, in 2022–2023, the average wait for an appointment was six days, twice as long as the average wait time in 2015.1
- Virtually all (98%) publicly supported clinics offering family planning provided pregnancy testing in 2022–2023, and the vast majority offered HIV testing (94%), testing for chlamydia or gonorrhea (98%), STI treatment (97%) and HPV vaccinations (92%).1
Role of the Title X Program
Within the larger context of publicly supported family planning services, the Title X program serves as a cornerstone, ensuring that millions of individuals receive essential sexual and reproductive health care and education. Title X is the only federal initiative in the United States dedicated to providing affordable family planning services. By improving access to a wide range of affordable services, including contraceptive methods, pregnancy testing and STI testing, the program plays a vital role in advancing public health and health equity.
Additional Guttmacher resources discuss Title X’s features and benefits, as well as challenges to the program.
- In 2023, there were more than 3,800 Title X–funded clinics. In total, they served 2.4 million female and 419,000 male family planning patients.6
- In 2023, Title X–funded clinics provided chlamydia testing for 1.3 million female and male patients. They also provided 1.6 million gonorrhea tests, 735,000 syphilis tests and 984,000 HIV tests.6
- In addition, in 2023, Title X clinics provided about 461,000 cervical cancer screenings (Pap tests) to nearly 434,000 patients.6
- The most recent year for which data are available on the distribution of Title X clinics and patients by provider type is 2020. Far fewer patients received Title X services in 2020 than in previous years, due to the domestic gag rule and the COVID pandemic. There were also far fewer clinics, including virtually no Planned Parenthood clinics, in the Title X network because of the gag rule.3
- In 20203:
- Public health departments accounted for 52% of Title X–funded family planning clinics and served 37% of female contraceptive patients.
- Federally qualified health centers accounted for 33% of Title X clinics and served 43% of female patients.
- Hospital outpatient sites accounted for 5% of Title X clinics and served 7% of female patients.
- Other independent clinics accounted for 9% of Title X clinics and served 11% of female patients.