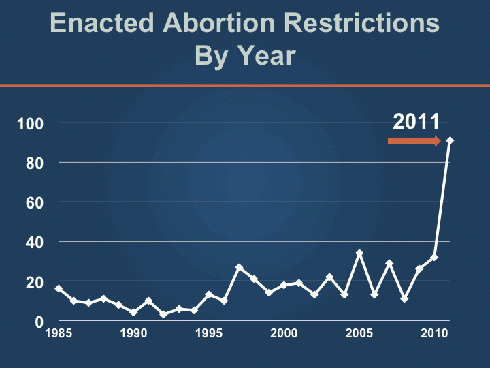
By almost any measure, 2011 saw unprecedented attention to issues related to reproductive health and rights at the state level. In all 50 states, legislators introduced more than 1,100 reproductive health and rights-related provisions, a sharp increase from the 950 introduced in 2010. By year’s end, 135 of these provisions had been enacted in 36 states, again an increase from the 89 enacted in 2010 and the 77 enacted in 2009. (Note: This analysis refers to reproductive health and rights-related “provisions,” rather than bills or laws, since bills introduced and eventually enacted in the states contain multiple relevant provisions.)
Fully 68% of these new provisions, 92 provisions in 24 states, restrict access to abortion services, a striking increase from last year, when 26% of new provisions restricted abortion. The 92 new abortion restrictions shattered the previous record of 34 abortion restrictions adopted in 2005. About the only bright spot for reproductive rights supporters was the defeat in Mississippi of a ballot initiative that would have sharply restricted women’s access not only to abortion but also to various contraceptive methods by defining a person under state law as “a human being from the moment of fertilization.” Other victories for supporters of reproductive health and rights were few and far between in 2011; two states expanded eligibility for family planning under their Medicaid programs and four states expanded access to STI prevention and treatment.
Abortion
The most high-profile state-level abortion debate of 2011 took place in Mississippi, where voters rejected the ballot initiative that would have legally defined a human embryo as a person “from the moment of fertilization,” setting the stage to ban all abortions and, potentially, most hormonal contraceptive methods in the state. Meanwhile, five states (AL, ID, IN, KS and OK) enacted provisions to ban abortion at or beyond 20 weeks’ gestation based on the spurious assertion that a fetus can feel pain at that point. These five states join Nebraska, which adopted a ban on abortions after 20 weeks in 2010 (see State Policies on Later Abortions). A similar limitation was vetoed by Minnesota Gov. Mark Dayton (D).
Later Abortion
Several other states took steps to restrict abortions later in pregnancy. Kansas, Missouri and Ohio enacted laws limiting abortions performed after viability to cases where the woman’s life or physical—but not mental—health is endangered. Kansas, along with Michigan, moved to further restrict “partial-birth” abortion by adopting the restrictive federal standard and banning the procedure even when the woman’s health is endangered. With the passage of these laws, 18 states now ban “partial-birth” abortion.
Counseling and Waiting Periods
Five states enacted provisions that require women seeking an abortion to obtain counseling that includes misinformation about the procedure, bringing to 16 the number of states that require that women be given misleading information prior to having an abortion (see Counseling and Waiting Periods for Abortion). Indiana and Kansas adopted provisions requiring that the woman be told that the fetus is a person from the moment of conception; the Kansas provision goes further by requiring providers to tell the woman that an abortion terminates fetal life. Indiana’s new requirement also mandates that a woman seeking an abortion be told that a fetus may be able to feel pain. A woman obtaining an abortion in North Dakota will be told that having an abortion would increase her risk of breast cancer, while the new requirement in North Carolina mandates that women be told that having an abortion can impair their future fertility and have lasting mental health consequences. Finally, a new provision in South Dakota would have required the woman to be told that some groups of women may be at higher risk of complications, because of their “physical, psychological, emotional, demographic or situational” characteristics; this provision was part of a broader state law that has been enjoined (see below).
Three states adopted waiting period requirements for a woman seeking an abortion. In the most egregious of the waiting period provisions, a new South Dakota law would have required a woman to obtain pre-abortion counseling in person at the abortion facility at least 72 hours prior to the procedure; it would also have required her to visit a state-approved crisis pregnancy center during that 72-hour interval. The law was quickly enjoined in federal district court and is not in effect. A new provision in Texas requires that women who live less than 100 miles from an abortion provider obtain counseling in person at the facility at least 24 hours in advance. (Both states permit these requirements to be waived when there is a medical emergency.) Finally, new provisions in North Carolina require counseling at least 24 hours prior to the procedure. With the addition of the new requirements in Texas and North Carolina, 26 states mandate that a woman seeking an abortion must wait a prescribed period of time between the counseling and the procedure; nine of these states require that the counseling be provided in person, a provision that requires the woman to make two trips to the facility (see Counseling and Waiting Periods for Abortion).
Ultrasound
Five states adopted provisions mandating that a woman obtain an ultrasound prior to having an abortion. The two most stringent provisions were adopted in North Carolina and Texas and were immediately enjoined in federal district court. Both of these restrictions would have required the provider to show the image to the woman and describe it to her. The other three new provisions (in AZ, FL and KS), all of which are in effect, require the abortion provider to offer the woman the opportunity to view the image or listen to a verbal description of it. These new restrictions bring to six the number of states that mandate the performance of an ultrasound prior to an abortion (see Requirements for Ultrasound). Two additional new provisions in Indiana and Iowa require providers to offer the woman the opportunity to undergo an ultrasound, but do not make it mandatory.
Insurance Coverage and Public Funding
Kansas, Nebraska, Oklahoma and Utah adopted provisions prohibiting all insurance policies in the state from covering abortion except in cases of life endangerment; they all permit individuals to purchase additional coverage at their own expense. The Utah law also includes exceptions in cases of rape, incest or a possible “substantial and irreversible impairment” to the woman’s health. The Oklahoma restriction narrows an existing provision by ending coverage in cases of rape or incest. These new restrictions bring to eight the number of states limiting abortion coverage in all private insurance plans (see Restricting Insurance Coverage of Abortion).
These four provisions also apply to coverage purchased through the insurance exchanges that will be established as part of the implementation of health care reform. Five additional states (FL, ID, IN, OH and VA) adopted requirements that apply only to coverage purchased on the exchange. All of these states permit coverage of an abortion in cases of life endangerment, rape or incest; the Indiana law also permits coverage when there is a risk of “substantial and irreversible impairment of a major bodily function.” The addition of these nine states brings to 16 the number of states restricting abortion coverage available through state insurance exchanges. In a rare victory for supporters of abortion rights in 2011, Montana Gov. Brian Schweitzer (D) vetoed a similar restriction in April.
In two other developments related to insurance coverage of abortion, North Carolina moved to limit abortion coverage under the health plan offered to state employees to cases of life endangerment, rape and incest; this brings to15 the number of states restricting abortion coverage for state employees.
Iowa moved to further restrict coverage of abortion for Medicaid recipients in the state to only cases of life endangerment, rape and incest, and eliminated a long-standing provision in state law providing coverage in cases where there is a diagnosed fetal abnormality. With this change, 32 states and the District of Columbia match the federal requirements under the Hyde amendment by limiting coverage to life endangerment, rape and incest (see State Funding of Abortion Under Medicaid).
Clinic Regulations
Four states enacted provisions directing the state department of health to issue regulations governing facilities and physicians’ offices that provide abortion services. A new provision in Virginia requires a facility providing at least five abortions per month to meet the requirements for a hospital in the state. New requirements in Kansas, Pennsylvania and Utah direct the health agency to develop standards for abortion providers, including requirements for staffing, physical plant, equipment and emergency supplies; supporters of the measures made it clear that the goal was to set standards that would be difficult, if not impossible, for abortion providers to meet. Kansas and Indiana moved to require that abortion providers have admitting privileges at a local hospital, something that has proven difficult to obtain in other states, often because of antipathy toward abortion providers. Enforcement of the proposed Kansas regulations has been enjoined by a state court.
Medication Abortion
In 2011, states moved to limit provision of medication abortion for the first time by prohibiting the use of telemedicine. Seven states (AZ, KS, NE, ND, OK, SD and TN) adopted provisions requiring that the physician prescribing the medication be in the same room as the patient (see Medication Abortion). Three of these states, Kansas, North Dakota and Oklahoma, also require that mifepristone be provided in accordance with a long-standing FDA protocol rather than under a simpler evidence-based protocol that has been proven to be safe and effective. The provisions in North Dakota and Oklahoma were enjoined in federal district court and are not in effect. Also this year, a 2004 Ohio requirement mandating the use of the FDA protocol was upheld by a federal appeals court, making it the only state that enforces the requirement. Finally, Arkansas extended its regulations on abortion clinics to apply to physicians who provide only medication abortion.
Parental Involvement
Six states adopted requirements that either mandate parental involvement or make it more cumbersome for a minor to use the judicial bypass procedure. Kansas and Nebraska, which both had required that a minor’s parents be notified, enacted measures requiring the parents to consent before the procedure is performed; this brings to 26 the number of states requiring parental consent before a minor has an abortion (see Parental Involvement in Minors’ Abortions). Both states require that the parents’ consent be notarized, a requirement in place in five other states. The new Kansas provision requires the consent of both parents in most cases, a requirement also in place in Mississippi and North Dakota. Four states (KS, NE, ND and OH) that require parental consent moved in 2011to make it more difficult for a minor to obtain a judicial waiver of the requirement; these states now require judges to find that there is “clear and convincing evidence” that the minor is sufficiently mature to make the decision on her own, a higher standard than that generally used in civil cases.
New Hampshire enacted provisions requiring that the parents of a minor be notified prior to an abortion; it replaces an existing state law that had been the subject of prolonged litigation. Florida, a state that already required parental notification, enacted legislation similar to that adopted in Kansas, Nebraska, North Dakota and Ohio to make it more difficult for a minor to obtain a judicial bypass. In Montana, meanwhile, Gov. Schweitzer vetoed a parental notification requirement, although the issue is set to go before voters in the state as part of a ballot initiative in 2012.
Reporting Requirements
Eight states enacted or amended abortion reporting requirements in 2011. Six of these states (AL, ID, IN, KS, MO and OK), all of which adopted restrictions on abortions performed later in pregnancy (see above), moved to require abortion providers to report a diagnosis when an abortion is performed at or beyond 20 weeks’ gestation. North Dakota also moved to require that providers report complications resulting from a medication abortion.
States also adopted a handful of other measures related to abortion:
- North Carolina, Texas and Utah enacted provisions authorizing the sale of “Choose Life” license plates; proceeds are designated to support alternatives to abortion services. The North Carolina provision has been enjoined in federal district court.
- Louisiana and North Carolina adopted provisions related to coercion. The Louisiana requirement mandates that abortion facilities post signs informing women that they cannot be coerced into having an abortion. The North Carolina provision requires abortion providers who believe that a woman might be the victim of domestic violence to provide her with information about available social services.
- Arizona enacted four provisions related to abortion. The first prohibits physician assistants and nurses from performing abortions; these provisions have been enjoined by a state court. The second bans abortion for purposes of race or sex selection. The third prohibits the use of public funds to train abortion providers at state universities. Finally, the state enacted a measure prohibiting residents from seeking a state tax deduction for donations made to an organization that provides, promotes or makes referrals for abortion services. This last provision has been enjoined by a U.S. District Court.
- Utah expanded its refusal clause to allow public and secular hospitals to refuse to provide abortion services; it also permits any employee of a health care facility to refuse to participate in an abortion procedure.
Family Planning
Family planning services and providers were especially hard-pressed in 2011, facing significant cuts to funding levels as well as attempts to disqualify some providers for funding because of their association with abortion. Considering the historic fiscal crises facing many states, it is significant that family planning escaped major reductions in nine of the 18 states (CO, CT, DE, IL, KS, MA, ME, NY and PA) where the budget has a specific line-item for family planning. The story, however, was different in the remaining nine states. In six (FL, GA, MI, MN, WA and WI), family planning programs sustained deep cuts, although generally in line with decreases adopted for other health programs. In the other three states, however, the cuts to family planning funding were disproportionate to those to other health programs: Montana eliminated the family planning line item, and New Hampshire and Texas cut funding by 57% and 66%, respectively.
Six states, meanwhile, moved to disqualify or otherwise bar certain types of providers from the receipt of family planning funds, taking three distinct approaches:
- Two states moved to restrict eligibility for family planning funds for providers that have any association with abortion. Indiana enacted legislation prohibiting agencies that provide abortion from receiving any funding through the state, including Medicaid; the provision is not being enforced due to a legal challenge. Wisconsin adopted a provision barring agencies that provide abortion services or referrals from receiving funding through the state. (Neither state is a Title X grantee, so Title X funds are not affected by the restriction.) Planned Parenthood is the only agency that would be affected in either state.
- These new requirements join long-standing provisions in three other states (CO, OH and TX) requiring agencies that receive funding— either state family planning funds or federal block grant allotments— through a state agency to be separate from agencies that provide abortion services (see State Family Planning Funding Restrictions).
- Two states moved to bar funding specifically for Planned Parenthood affiliates. North Carolina adopted a budgetary provision that explicitly bans Planned Parenthood from obtaining funding, including Medicaid, through the state. Since North Carolina is a Title X grantee, the measure blocks Planned Parenthood affiliates in the state from receiving Title X funds. This restriction is blocked from enforcement pending resolution of a legal challenge.
- New Hampshire decided not to renew its contract through which the Planned Parenthood affiliate in the state received Title X funds. The Office of Population Affairs, the federal agency that administers the Title X program, determined that the state would not have the ability to provide services in the absence of the sites operated by Planned Parenthood and provided funds to Planned Parenthood directly, rather than requiring it to be a subrecipient of the state.
- Two additional states took aim at agencies that provide mostly family planning services, regardless of whether they have any connection to abortion. Kansas enacted a provision that limits the distribution of Title X funds to health departments, hospitals and community health centers; other types of family planning providers are not eligible; the law is blocked from enforcement as part of a court case. Texas, meanwhile, adopted a provision that gives priority to health departments, community health centers and hospitals in the distribution of family planning funds, including Title X funds; other family planning providers could receive funding should any remain.
Given the difficult fiscal and political climate in states in 2011, it is especially noteworthy that three states expanded Medicaid eligibility for family planning:
- The Maryland legislature directed the state to extend coverage to individuals with an income of up to 200% of the federal poverty level; the state currently has a more limited expansion that extends coverage only to women following a Medicaid-funded delivery. The state’s request was approved by the Centers for Medicare and Medicaid Services (CMS), the federal agency that administers Medicaid, and will go into effect in 2012.
- The legislature in Washington directed the state to raise eligibility under the program from 200% to 250% of the federal poverty level, reversing an earlier attempt by the state agency, as part of a larger effort to cut state expenditures, to discontinue its existing Medicaid family planning expansion.
- Finally, CMS approved Ohio’s request to expand eligibility for family planning to individuals with an income of up to 200% of the federal poverty level. This move is particularly significant because Ohio is the first totally new state to utilize the authority under health care reform to expand Medicaid eligibility for family planning; all the other states that have done so had previously expanded eligibility by obtaining a federal waiver.
With the approval of Ohio’s program, 24 states have expanded eligibility for family planning under Medicaid based solely on income; seven have utilized the new authority under health care reform (see Medicaid Family Planning Eligibility Expansions).
Adolescents
Unlike in recent years when states had moved to expand access to comprehensive, medically accurate sex education, the only relevant measures enacted in 2011 expanded abstinence education. Mississippi, which had long mandated abstinence education, adopted provisions that make it more difficult for a school district to include other subjects, such as contraception, in order to offer a more comprehensive curriculum. A district will now need to get specific permission from the state department of education. A new requirement enacted in North Dakota mandates that the health education provided in the state include information on the benefits of abstinence “before and outside of marriage.” Including North Dakota, 37 states now mandate abstinence in sex education (see Sex and HIV Education).
Two states expanded the list of individuals and organizations required to report suspected instances of statutory rape. Illinois enacted a provision requiring health care professionals providing either abortion or family planning services to report suspected child abuse and neglect. Kansas adopted a requirement mandating that employees or volunteers of organizations that provide services to pregnant teenagers report suspected child abuse.
Sexually Transmitted Infections
Over the course of 2011, four states took positive steps to expand access to STI prevention and treatment. Three states adopted provisions permitting a health care provider to prescribe STI treatment to the partner of patient, even if he or she has not been seen by the provider. Connecticut and Indiana permit treatment for chlamydia or gonorrhea, and in Massachusetts, providers may offer treatment for chlamydia only. Including these three, 24 states explicitly allow treatment for a patient’s partner (see Partner Treatment for STIs).
California, meanwhile, enacted requirements permitting minors older than 11 to consent to services for STI prevention, including vaccines for HPV and Hepatitis B; previous state law had only permitted minors to consent to the diagnosis and treatment of STIs. Moving in the other direction, Utah adopted a provision requiring most minors to obtain parental consent to obtain vaccination for HPV.
Pregnancy and Birth
States enacted a variety of measures relating to pregnancy and birth. Four states adopted requirements aimed at expanding access to treatment services. Maine adopted a measure to include HIV testing as part of routine prenatal care; Oklahoma enacted a law requiring a woman to have an HIV test when she delivers, if she has not already received one as part of prenatal care. Colorado and Kentucky enacted legislation allocating funding for substance abuse prevention and treatment for pregnant women (see Substance Abuse During Pregnancy).
Five additional states took other, related steps. Four states (AL, NY, NC and PA) adopted provisions allowing a woman who had a miscarriage to obtain a “certificate of stillbirth” from the state. North Carolina enacted legislation permitting injury to a fetus to be considered homicide or assault; the measure specifically exempts medical care, including abortion, and events resulting from actions by the woman. Tennessee, which already had a fetal homicide statute, expanded it to apply to injury to a fetus throughout pregnancy, not just after viability.
Environmental Exposure to Reproductive Toxins
Eight states took a variety of steps to limit exposure to specific substances that have been shown to adversely affect reproductive health:
- California, Delaware and Maryland enacted provisions banning the use of Bisphenol A (BPA) in bottles and cups used by infants and children; including these states, eight states have banned the use of BPA in products designed for children and infants. Connecticut adopted a requirement that prohibits the use of BPA in paper used to print receipts by retailers.
- Maryland enacted a provision curtailing the use of a widely used flame retardant in products manufactured or sold in the state.
- Maine adopted a provision increasing access to lead screening at sites providing education or health care to low-income children. In an attempt to reduce exposure to lead and mercury, Illinois mandated that 50% of all electronic devices sold in the state must be recycled or reused.
- Illinois, New York and Vermont expanded the list of items that are prohibited from containing mercury. New York mandated environmental testing for mercury as part of the approval process for new power plants or other facilities to generate electricity.