Background
The COVID-19 pandemic in the United States has quickly reshaped the American social landscape, including people’s intimate lives. This report provides an initial look at newly collected data on the emerging impact of the pandemic on women’s sexual and reproductive health (SRH) and reproductive autonomy in the United States. It focuses on the following indicators:
- Childbearing preferences
- Contraceptive use
- Access to contraception and other SRH services
- Telemedicine for contraceptive care
- Exposure to intimate partner violence (IPV)
The pandemic has changed the social and economic realities of people’s lives. The nearly universal imposition of stay-at-home requirements begun in mid-March 2020, the numerous restrictions remaining thereafter and the widespread uptake of social distancing have led to growing economic and social insecurity. Further, existing social inequities mean that the burden of the pandemic has not been experienced equally. For example, COVID-related mortality has been greater among people of color.1 Women are more likely than men to have lost their jobs, and women of color have thus far experienced the most job losses.2,3 The large increase in overall unemployment has meant that many people have lost their work-related health insurance, resulting in reduced access to health care.4
Anecdotal reports and press accounts have described the impact of the pandemic on women’s SRH and well-being. Social distancing and the disruption caused by the pandemic have created physical and economic barriers to contraception and other SRH services. The changing economic and social environment may be shifting people’s fertility preferences or patterns of contraceptive use. Concerns have surfaced about women’s exposure to IPV* and about inadequate access to IPV services during the pandemic.6,7 IPV, particularly acts of sexual violence and reproductive control, disproportionately impacts women of reproductive age and can compromise women’s health and autonomy.8
Previous large-scale disruptions have affected women’s reproductive lives. For example, during the 2008 Great Recession, women reported difficulties affording contraception or other SRH care,9 and household unemployment was associated with an increased likelihood of IPV.10 Further, that event helped shift women’s fertility preferences and set in motion declines in national fertility rates.11,12 Similarly, prior natural disasters in the United States, such as Hurricane Katrina, have disrupted the availability of contraceptive methods and services and have led to increases in IPV and (at least) short-term declines in fertility.13–15 The impact of these prior disruptions suggests that the COVID-19 pandemic—with its unprecedented and severe economic, social and physical challenges—will also have major consequences for reproductive health goals and behaviors, access to care and far beyond.
In this report, we examine new data collected from cisgender women in the United States on how they feel that the COVID-19 pandemic has influenced their SRH. We also examine women’s reports of pandemic-related economic challenges and how these challenges intersect with their sexual and reproductive experiences. Across these analyses, we give particular attention to longstanding social and economic inequities experienced by women based on their race, ethnicity, sexual orientation or income level. To understand the scope and magnitude of these initial impacts of the COVID-19 crisis, we compare them directly with the SRH challenges observed as part of the social and economic instability following the 2008 Great Recession.
Findings
This analysis is based on a national internet-based survey conducted by the Guttmacher Institute over the week of April 30–May 6, 2020. The respondents were 2,009 cisgender women aged 18–49 who had ever engaged in penile-vaginal sex. All differences discussed in the text are statistically significant at the p<.05 level. Additional information about the survey and methods of analysis is detailed in the Appendix.
Fertility preferences
Individuals’ fertility preferences are shaped in part by the broader socioeconomic context. Pandemic-related worries about finances and job stability, as well as general unease about the future, may be shifting how women feel about having children.
- More than 40% of women reported that because of the COVID-19 pandemic, they changed their plans about when to have children or how many children to have. Changes in fertility preferences were more common among women without any children than among those with children (45% vs. 38%).
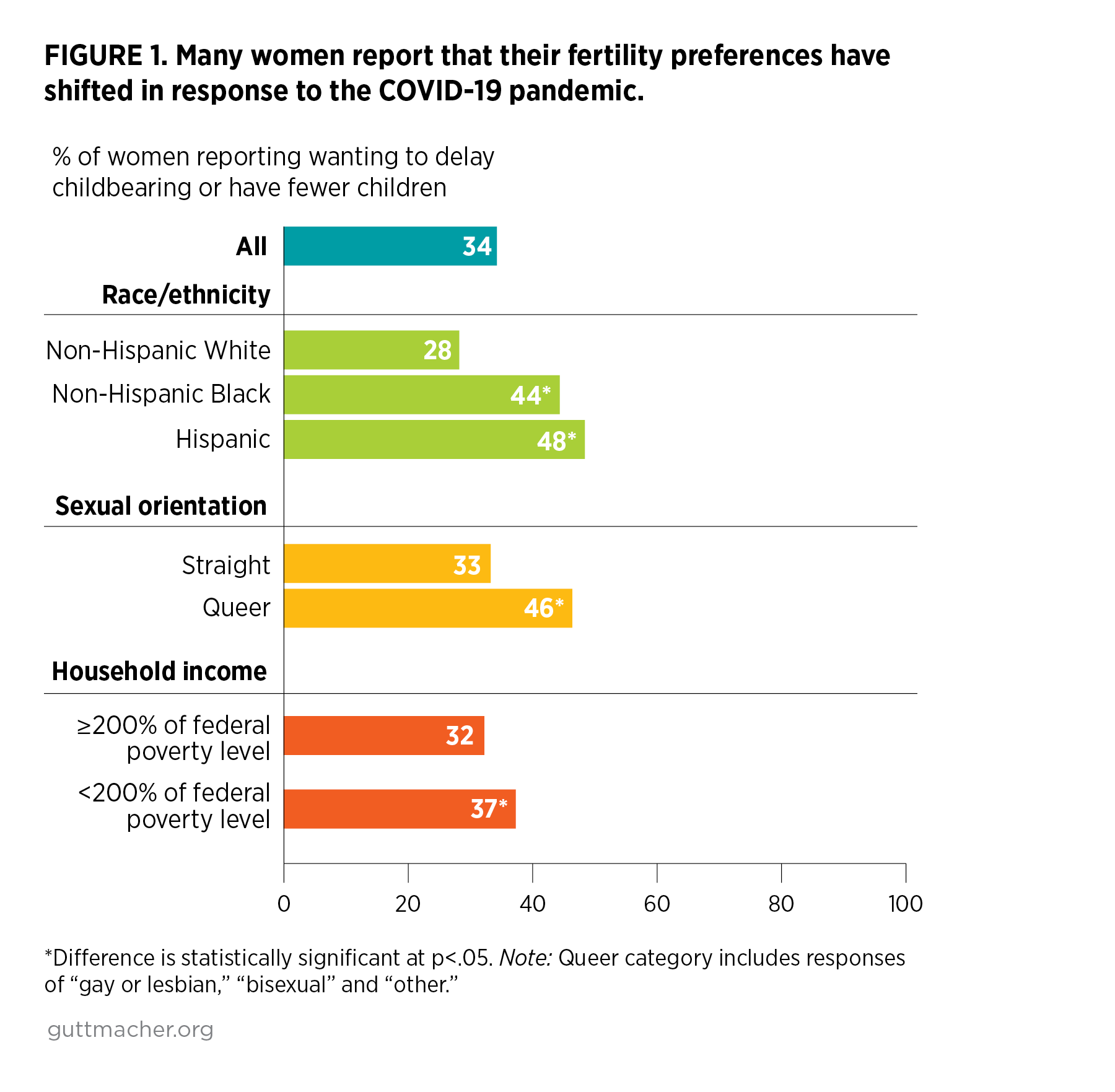
- Overall, one-third of women (34%) wanted to get pregnant later or wanted fewer children because of the pandemic (Figure 1).†
- Sharp disparities were seen in these changing fertility preferences, and women belonging to groups already experiencing systemic health and social inequalities reported the greatest change.
- Black women (44%) and Hispanic women (48%) were more likely than White women (28%) to state that because of the pandemic, they wanted to have children later or wanted fewer children.
- Queer‡ women (46%) were more likely than straight women (33%) to report such a change in fertility preferences.
- Lower-income women§ (37%) were more likely than higher-income women (32%) to report this change.
- In contrast, 17% of women wanted to have a child sooner or wanted to have more children because of the coronavirus pandemic.
Access to contraception and SRH services
During the pandemic, women’s access to contraception and other SRH services—as well as their ability to pay for these services—has been constrained. Access to in-person health care has been severely limited, and people may have avoided seeking out available services because of fears that they or a family member would be exposed to COVID-19 as a result.
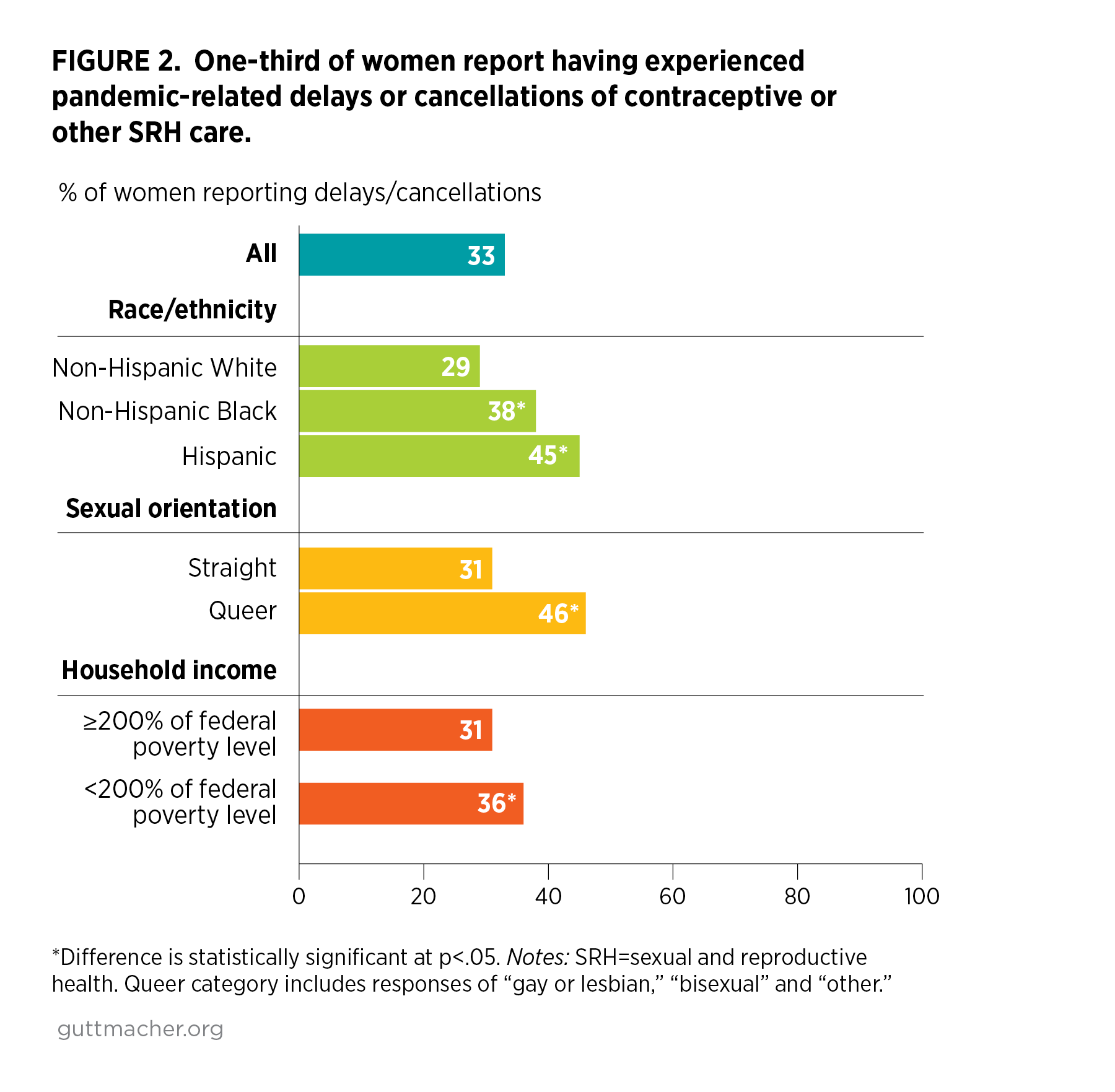
- One in three women (33%) reported that because of the pandemic, they had had to delay or cancel visiting a health care provider for SRH care, or had had trouble getting their birth control (Figure 2).
- Such barriers to timely care were more common among Black (38%) and Hispanic (45%) women than among White women (29%), and more common among queer women (46%) than among straight women (31%).
- Lower-income women were also more likely than higher-income women to report having experienced delays or being unable to get contraceptive or SRH care because of the pandemic (36% vs. 31%).
Many women reported feeling increased worry about their ability to pay for and obtain contraception and other SRH services because of the pandemic.** These impacts have been unevenly distributed, and the pandemic appears to be perpetuating existing inequities, although telemedicine offers a new means for some women to obtain birth control.
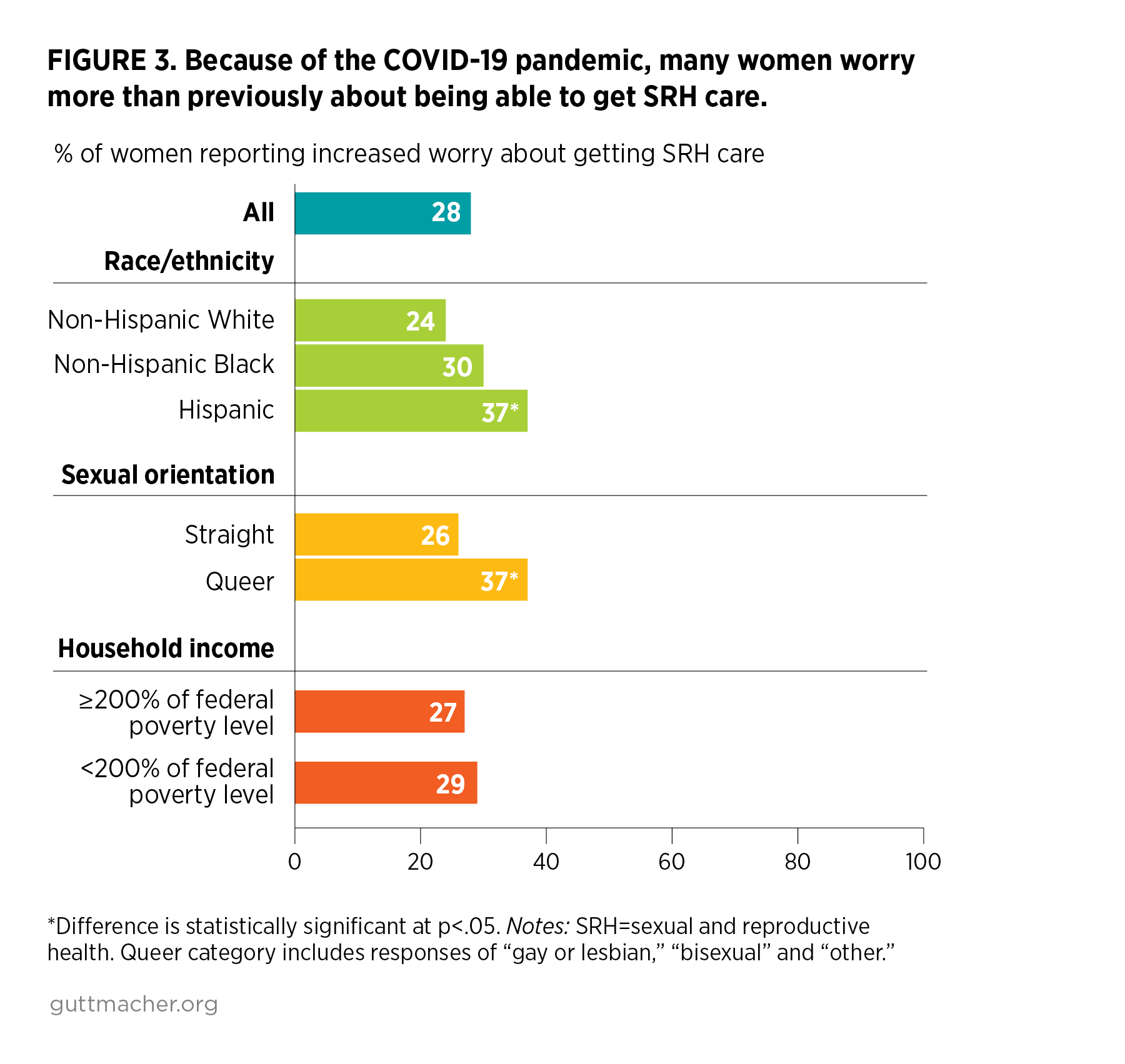
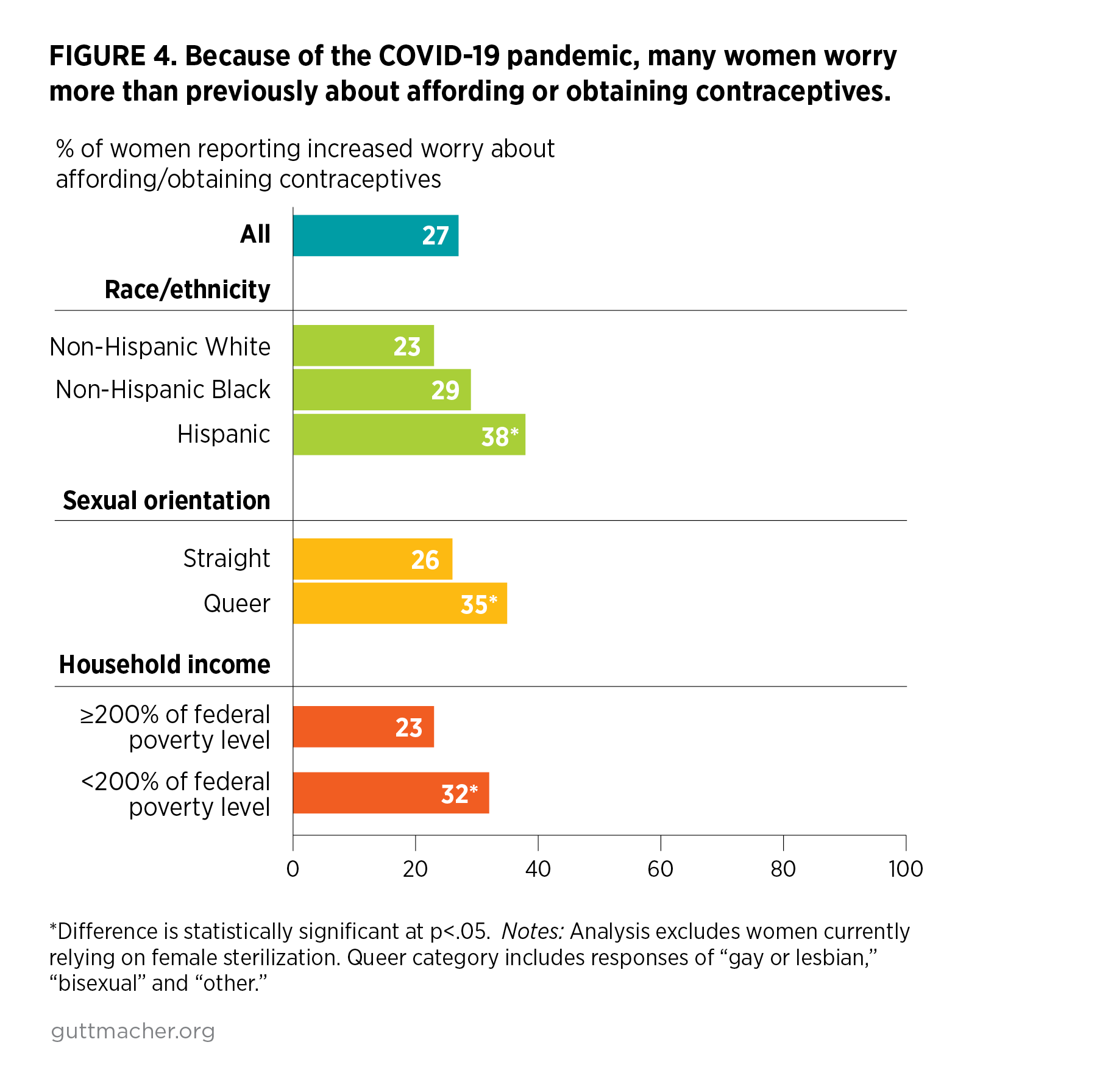
- About one-quarter (28%) of women said they worry more than they used to about being able to get needed SRH care because of the COVID-19 pandemic (Figure 3). In addition, 27% of women reported that because of the pandemic, they worry more than they used to about their ability to afford or obtain a contraceptive method specifically (Figure 4).
- Hispanic women and queer women were more likely than White and straight women, respectively, to report increased worry about each type of concern.
- For both measures, more than one-third of Hispanic and queer women reported increased worry.
- Lower-income women were more likely than higher-income women to report a pandemic-related increase in worry about affording or obtaining contraception (32% vs. 23%).
- Telemedicine has helped to fill in some new SRH service gaps. For example, among women using the pill, 24% reported that, because of the pandemic, they had switched to a telemedicine appointment with their health care provider to have their prescription refilled.
Attitudes toward contraception††
Many women’s attitudes toward contraception have changed because of the pandemic. For some women, the crisis appears to have promoted a shift to more effective contraceptive methods and more consistent use.
- One-third (34%) of women agreed with the statement "Because of the COVID-19 (coronavirus) pandemic, I am more careful than I used to be about using contraception every time I have sex."
- This increased attention to the consistency of contraceptive use was more common among women who reported wanting to delay childbearing or have fewer children because of the pandemic (49%) than among women wanting more children or those whose childbearing preferences did not change (26%).
- The proportion intending to use contraceptives more consistently was also greater among Black women (44%) and Hispanic women (43%) than among White women (30%).
- Twenty-three percent of women reported thinking more about getting a longer-acting contraceptive method (an IUD, implant, injectable or shot) because of the pandemic.
- This interest was more common among women expressing concerns about reduced access to contraceptives (53%) than among women without these concerns (13%).
Intimate partner violence
Economic crises and stress are recognized as contributing factors to IPV,10,16 and the confinement, increased stressors and uncertainty of the pandemic may have exposed some women to IPV. Further, stay-at-home orders and social distancing have made it harder for people experiencing IPV to obtain support and resources.
- Sixteen percent of women reported having experienced IPV in 2020 thus far.‡‡ Overall, they reported that a current or former partner exhibited the following specific behaviors (multiple responses were allowed):
- Humiliated or emotionally abused them (11%)
- Forced them to engage in any kind of sexual activity (5%)
- Kicked, hit, slapped or otherwise physically harmed them (6%)
- Made them feel afraid (10%)
- Among women who reported IPV in early 2020, one in three (33%) indicated having trouble or being unable to seek services in response to the violence they experienced.
Economic impact of the COVID-19 pandemic
Many respondents found themselves facing financial difficulties as a result of the pandemic; these may contribute to the impact of the crisis on women’s access to care and their fertility desires. The fact that sizable proportions of women reported COVID-related economic challenges is especially notable because surveys were completed in early May 2020, while the pandemic and its consequences were still unfolding.
- More than half of respondents (52%) said that they or someone in their household had lost their job or had had their work hours reduced because of the pandemic.
- About one in three women (32%) reported that they were financially worse off at the end of April 2020 than they had been a year before.
- Compared with women who were not financially worse off than they had been a year ago, those who were worse off were more likely to report delays or inability to get contraceptives or other SRH care (42% vs. 29%).
- Women whose finances had worsened were also more likely than other women to report wanting to delay childbearing or have fewer children because of the pandemic (39% vs. 32%).
- Among women with children, 41% agreed with the statement "Because of the COVID-19 (coronavirus) pandemic, I worry more about being able to take care of my children." This worry was more common among women who reported being financially worse off than among those who were not worse off (55% vs. 35%).
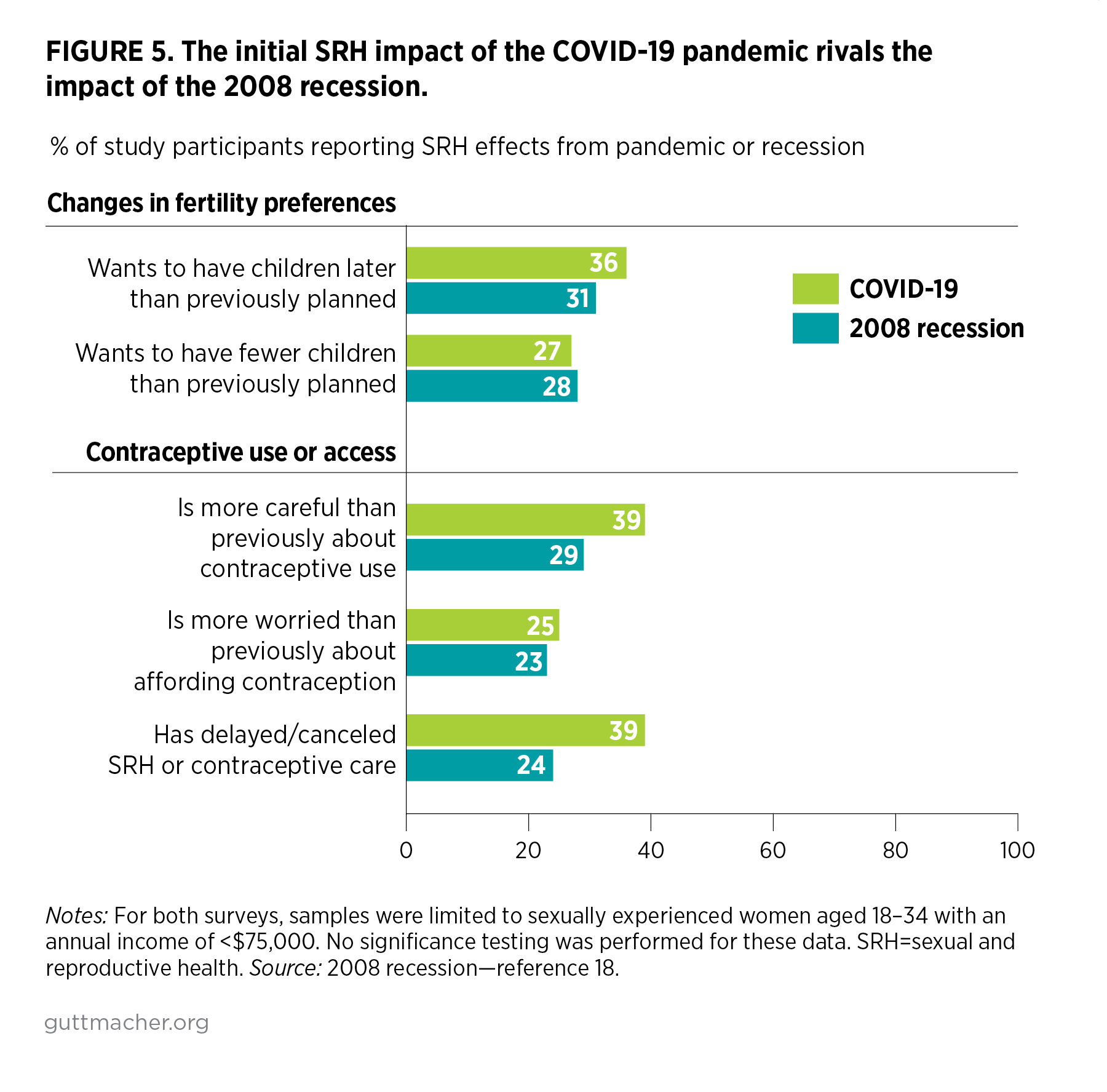
Comparing the initial SRH impact of the pandemic with the 2008 recession
Few societal events could rival the COVID-19 pandemic for its effects on people’s lives, but the 2008 Great Recession also had a major economic and social impact on the United States. Here, we compare findings from a 2009 Guttmacher Institute survey examining how the 2008 recession had affected women’s lives and SRH18 to findings from this new 2020 survey on COVID-19, to provide context for understanding the initial impacts of the pandemic. The recession survey was limited to women aged 18–34 with household incomes below $75,000, so for the purpose of comparison in this section of the report, we have reduced our 2020 study sample to a similar group. We were unable to test differences between the two studies for statistical significance.
Comparing the two surveys shows that in many ways, the magnitude of the impact of the COVID-19 crisis on women’s SRH already rivals that of the 2008 recession, even just a few months into the pandemic.
- The COVID-19 pandemic and the 2008 recession resulted in fairly similar proportions of women shifting their fertility preferences in favor of delaying childbearing or having fewer children (Figure 5).
- Some 39% of women said they were being more careful than they used to be about their contraceptive use as a result of the pandemic, whereas 29% of women reported such a shift in response to the 2008 recession.
- Similar proportions of women reported increased worry about being able to afford their birth control as a result of the pandemic (25%) and as a result of the recession (23%).
- A higher proportion of women reported delays in access or inability to get contraception or other SRH care because of the COVID-19 pandemic than because of the recession (39% vs. 24%).
Discussion
We found clear indications that the COVID-19 pandemic has already had rapid and broad impacts on women’s sexual and reproductive health (SRH) experiences, even as the full effects of the crisis continue to unfold. This snapshot documents how, in just the few months since the United States entered the crisis,19 the disruption of this pandemic has created logistic and economic barriers to accessing contraception and other SRH services and has spurred significant changes in women’s fertility and contraceptive preferences and behaviors. Importantly, the pandemic is compounding existing social inequities by disproportionately affecting Hispanic and Black women, queer women and poorer women.
Since at least mid-March, in-person health care has been severely limited, with providers needing to limit hours and curtailing in-person visits. Women reported having had to delay or cancel SRH care and expressed concerns about their ability to afford or obtain contraceptives. Even once all stay-at-home restrictions are lifted, women may not seek out needed SRH services, due to fears that doing so may expose them or a family member to COVID-19, and providers may continue to provide reduced in-person care. The uneven public health response to the pandemic at the federal, state and local levels might prolong this fear or uncertainty. These disruptions in needed care could result in continued barriers to obtaining desired contraceptives, increases in pregnancies among women who wanted to avoid them and delayed identification and treatment of cervical cancer and STIs. All of these outcomes carry negative health, social and economic consequences.
With substantial job losses and broad economic uncertainty, more than one in three women reported that because of the pandemic, they want to delay having a child or limit future births. Even with many women reporting that they have increased their consistent use of contraceptives, these changing fertility preferences, combined with barriers to obtaining contraceptives, suggest that the number of women who will need to access abortion care may increase. Yet as of May 12, 2020, at least 11 states had attempted to exploit the pandemic by banning or restricting abortion access as "nonessential health care,"20 contradicting leading medical experts’ statements asserting that abortion remains an essential and time-sensitive health service during the COVID-19 crisis.21 These restrictions, coupled with the logistic and economic challenges associated with obtaining care during the pandemic, create new barriers to abortion services.
Barriers to abortion may result in an increase in births from unintended pregnancies. Still, a COVID-related baby boom is unlikely;22 instead, the economic and social instability of the pandemic is likely to contribute to ongoing declines in childbearing in the United States.23 Reports of similar shifts in fertility preferences because of COVID-19 have also been identified recently in the United Kingdom, Germany, France, Spain and Italy, suggesting that declines in fertility may be widespread.24
Stay-at-home orders, growing economic insecurity and disruptions to the health care system have made the COVID-19 pandemic a unique experience for most people living in the United States. While the broad social and economic disruptions of the COVID-19 pandemic differentiate it from other recent crises, the immediate short-run SRH impact is in some ways comparable to the longer-run impacts of the 2008 recession. Given that we are only at the early stages of this crisis, continued job and insurance losses will likely create ongoing economic challenges that will further affect SRH.
The social impact of the COVID-19 health crisis and its economic consequences cannot be disentangled clearly. The emerging recession and the slow pace of economic recovery will likely compound the pandemic's impact on SRH. Health insurance is key to obtaining SRH care, and as more people lose their jobs, they will also lose their insurance, further disrupting access to care. Longer-term monitoring of individuals’ experiences with SRH care will be important for identifying needs and prioritizing new approaches. Access to SRH care, including contraception, is a key component of reproductive autonomy and justice in allowing women to control if and when to have a child.25 Supporting the goals of reproductive justice will mean focusing on responses to the pandemic that prioritize communities that have already borne the brunt of existing structural, societal, economic and health inequities.26–28
While our study findings focus on individual experiences, changes in the health care system are needed to better serve women as the challenges of the pandemic continue to unfold. Further expansion and adoption of innovative approaches to SRH services, such as telemedicine or provision of contraceptives by mail, may ultimately increase access to SRH care. Indeed, a shift to telemedicine has helped maintain access to contraceptive care for some women thus far. However, regardless of the mode of health care delivery, the economic barriers created by the loss of health insurance and reductions in household income must also be addressed, to avoid compounding existing disparities.
Policy experts have identified ways in which SRH services can be supported as essential health care. In addition to broadening access to SRH care through telemedicine, these include protecting and expanding access to comprehensive health insurance coverage and increasing funding for the Title X national family planning system in response to the likely growing numbers of the uninsured and increased demand for publicly funded SRH services.29,30 Increased support for community-level services, such as hotlines, counseling and emergency housing, to better help those experiencing IPV is also needed, as many women who experienced IPV in recent months reported that they were unable to seek help.
Although this report provides revealing data on the early impact of the pandemic on women’s SRH needs and experiences, it could not address all of the important SRH issues or the needs of all users of SRH services. For example, we focused on cisgender women, while recognizing that individuals of all genders need access to SRH services. Greater COVID-19–related barriers to care among queer women and women of color highlight the need for provision of inclusive and culturally aware care. Adolescents represent another group with distinct SRH needs not examined here; for them, stay-at-home orders and other barriers to in-person care limit access to private and confidential services.31 In addition, attention needs to be given to the health care needs of pregnant and parenting individuals,32 as well as to aspects of testing for and treatment of STIs that may not have been captured in this survey.33 Further, this study focused on examining individual-level impact and did not directly examine the impact of the pandemic on the struggling health care system.
Conclusion
Even in the short period covered by our survey, the COVID-19 pandemic has already had an impact on women’s sexual and reproductive lives. It has affected their ability to obtain needed SRH care and contraceptive services, raised their concerns about affording and accessing this care and shifted their fertility preferences. These effects have not been evenly distributed and tend to be felt by groups bearing the brunt of existing inequities. In this way, the pandemic has illuminated systemic failings that perpetuate health and social disparities. The impacts analyzed in this report are fairly immediate to the current conditions of the crisis; in the longer term, the pandemic is likely to have larger and more varied effects. While the spread of COVID-19 has created a health crisis, we can take steps to minimize the impact on SRH. The pandemic will have far-flung effects on individuals, providers and the health care system. Those looking to address barriers to care will have to acknowledge and work to improve care across all of these levels. Policymakers must recognize that SRH care is essential in people’s lives and cannot be overlooked, bargained away or exploited vis-à-vis the competing COVID-19 priorities. Protecting individuals’ ability to make decisions about their SRH, and supporting the health care system to meet these needs, is essential.
Appendix: Detailed Methodology
Study participants (n=2,009) were recruited via the Qualtrics online panel.34 The Qualtrics Panel is a subdivision of Qualtrics, a private research software company specializing in Web-based data collection that partners with more than 20 Web-based panel providers. Panelists receive an invitation to participate in the survey via email or social media accounts.35 Question items about COVID-19 were included in a larger survey measuring a range of sexual and reproductive health (SRH) experiences, the Guttmacher Survey of Reproductive Health Experiences (GSRHE). Average completion time for the entire survey was 14 minutes. The COVID-19 questions accounted for 31 of 127 survey items.
Eligible respondents were those who (1) identified as a cisgender woman (i.e., assigned female at birth and currently identifying as a woman), (2) were aged 18–49, (3) were residing in the United States and (4) reported ever having had penile-vaginal sex. Participants who matched the eligibility criteria and agreed to participate in a research study were asked to complete an online survey that included a module on SRH and the COVID-19 pandemic. Surveys were conducted in English.
Study procedures were approved by the Guttmacher Institute institutional review board. Participants could skip any survey questions and could end the survey at any time. The survey collected no identifying information, and, to maintain respondents’ confidentiality, Qualtrics did not share respondents’ IP addresses with the study team. Panelists who completed the survey received $1.07 or the equivalent in redeemable points directly from Qualtrics. This is a standard incentive used for Qualtrics panel surveys that collect data from the general population.
Quota sampling was used to ensure a diversity of respondents by race and ethnicity, region and age. The survey utilized an opt-in sample and was not designed to be fully representative of the national population. However, the survey sample broadly mirrors the regional and racial and ethnic breakdown of the United States, based on the 2010 Census. Qualtrics has been found to be more demographically representative than surveys recruited through other opt-in approaches.36
To minimize inattentive responses, eligible participants were excluded from the analysis if their survey was completed in less than five minutes (n=7) or more than 600 minutes (n=1). Those who completed fewer than 50% of survey questions (n=10) were excluded, to ensure data completeness. We also excluded from the study participants who provided nonsensical responses to open-ended questions (n=7).
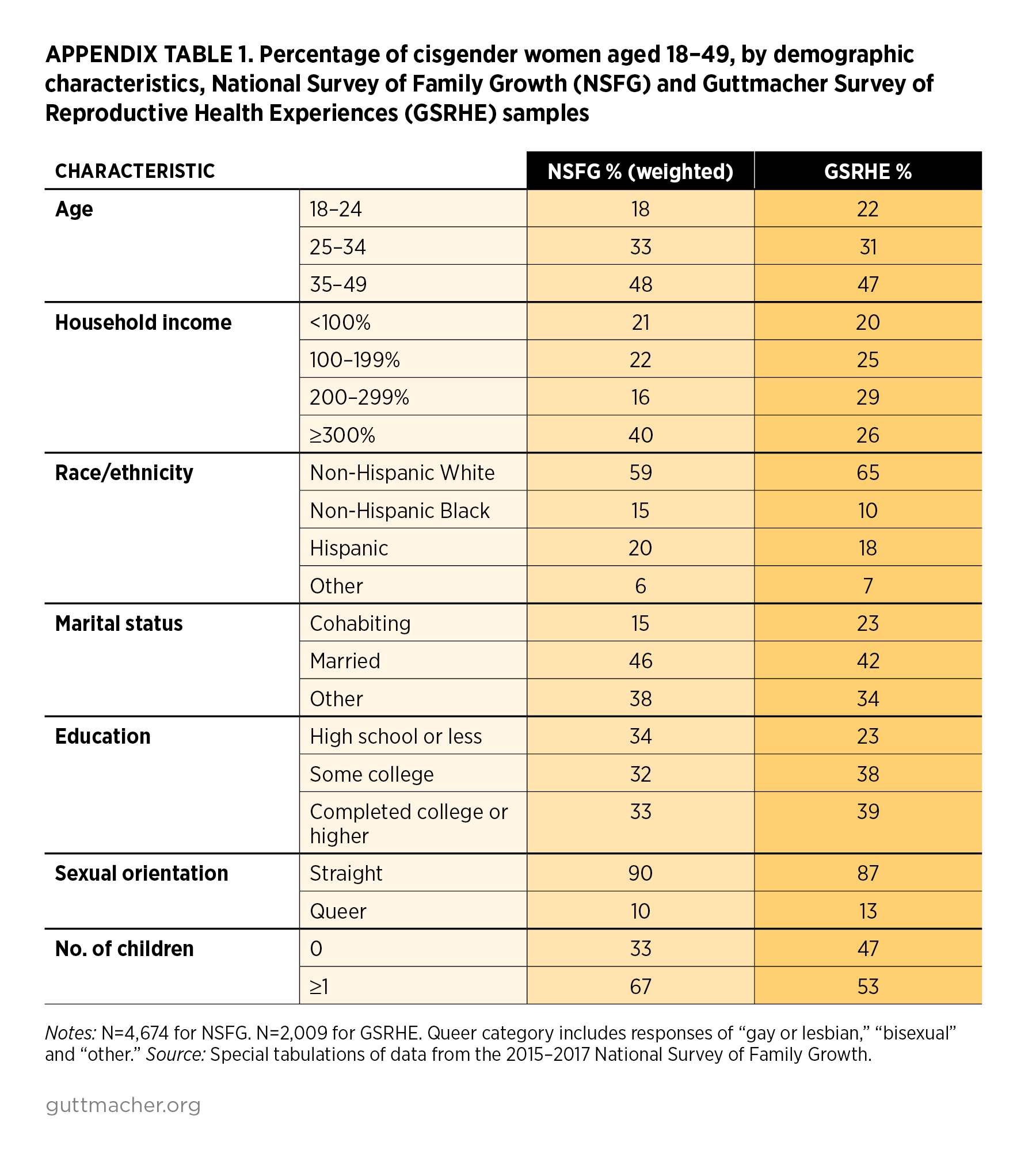
Appendix Table 1 compares the GSRHE to a similarly defined sample of respondents from the 2015–2017 National Survey of Family Growth (NSFG). The GSRHE sample appears similar to that of the NSFG in terms of age, poverty status, race and ethnicity, marital status and sexual orientation. On the other hand, the GSRHE sample is more highly educated than the NSFG sample and has a higher proportion of childless women.
Data were analyzed using Stata 16.0. We estimated bivariate logistic regression analyses for differences between subgroups; all differences presented in the text of this report were statistically significant at the p<.05 level, while statistically significant differences between subgroups are demarcated in the accompanying figures. The exception to this is the comparison of impacts of the 2008 recession and the COVID-19 pandemic, as complete standard errors were not available from the published recession findings. Because quotas for race/ethnicity and region were set to mirror the U.S. Census population, we did not weight data in our analyses.
Footnotes
*The U.S. Centers for Disease Control and Prevention defines IPV as behaviors perpetrated by a person's spouse or romantic partner that include physical violence, sexual violence or psychological/emotional violence.5
†Women could report more than one change in their fertility preferences.
‡Respondents were asked to report their sexual orientation from the following responses: heterosexual or straight, gay or lesbian, bisexual and other. We combined all responses other than "heterosexual or straight" into a single "queer" category.
§Defined as those with a household income less than 200% of the 2019 federal poverty level ($25,750 for a household of four).
**Analysis of survey questions about increased worry related to obtaining and paying for contraception excluded women currently relying on female sterilization.
††These measures excluded women currently relying on female sterilization.
‡‡IPV behaviors were assessed using questions developed from the HARK screening tool recommended by the U.S. Preventive Services Task Force.17
References
1. Hooper MW, Nápoles AM and Pérez-Stable EJ, COVID-19 and racial/ethnic disparities, JAMA, 2020, doi:10.1001/jama.2020.8598.
2. Ewing-Nelson C, After a full month of business closures, women were hit hardest by April’s job losses, Fact Sheet, Washington, DC: National Women’s Law Center, 2020, https://nwlc-ciw49tixgw5lbab.stackpathdns.com/wp-content/uploads/2020/0….
3. Gupta AH, Why some women call this recession a "shecession," New York Times, May 9, 2020, https://www.nytimes.com/2020/05/09/us/unemployment-coronavirus-women.ht….
4. Garrett B and Gangopadhyaya A, How the COVID-19 recession could affect health insurance coverage, May 4, 2020, https://www.rwjf.org/en/library/research/2020/05/how-the-covid-19-reces….
5. Saltzman L et al., Intimate Partner Violence Surveillance Uniform Definitions and Recommended Data Elements: Version 1.0, Atlanta: National Center for Injury Prevention and Control, Centers for Disease Control and Prevention, 2002.
6. Fetters A and Khazan O, The worst situation imaginable for family violence, The Atlantic, May 8, 2020, https://www.theatlantic.com/family/archive/2020/05/challenge-helping-ab….
7. Domestic violence has increased during coronavirus lockdowns, The Economist, April 22, 2020, https://www.economist.com/graphic-detail/2020/04/22/domestic-violence-h….
8. Hasstedt K and Rowan A, Understanding intimate partner violence as a sexual and reproductive health and rights issue in the United States, Guttmacher Policy Review, 2016, 19:37–45, https://www.guttmacher.org/gpr/2016/07/understanding-intimate-partner-v….
9. Gold RB, Recession taking its toll: family planning safety net stretched thin as service demand increases, Guttmacher Policy Review, 2010, 13(1):5.
10. Schneider D, Harknett K and McLanahan S, Intimate partner violence in the great recession, Demography, 2016, 53(2):471–505, doi:10.1007/s13524-016-0462-1.
11. Schneider D, The Great Recession, fertility, and uncertainty: evidence from the United States, Journal of Marriage and the Family, 2015, 77(5):1144–1156, doi:10.1111/jomf.12212.
12. Hartnett CS and Gemmill A, Recent trends in U.S. childbearing intentions, Demography, forthcoming.
13. Ellington SR et al., Contraceptive availability during an emergency response in the United States, Journal of Women’s Health, 2013, 22(3):189–193, doi:10.1089/jwh.2012.4178.
14. Stone L, Short-run fertility responses to mortality events: a look to the past, Applied Demography, 2020, 32(1):18–20.
15. Schumacher JA et al., Intimate partner violence and Hurricane Katrina: predictors and associated mental health outcomes, Violence and Victims, 2010, 25(5):588–603.
16. Conger RD et al., Linking economic hardship to marital quality and instability, Journal of Marriage and the Family, 1990, 52(3):643–656, doi:10.2307/352931.
17. United States Preventive Services Taskforce, Screening for intimate partner violence, elder abuse, and abuse of vulnerable adults, JAMA, 2018, 320(16):1678–1687, doi:10.1001/jama.2018.14741.
18. Guttmacher Institute, A Real-Time Look at the Impact of the Recession on Women’s Family Planning and Pregnancy Decisions, 2009, https://www.guttmacher.org/report/real-time-look-impact-recession-women….
19. World Health Organization, Director-General’s opening remarks at the media briefing on COVID-19, 2020, https://www.who.int/dg/speeches/detail/who-director-general-s-opening-r….
20. Jones RK, Lindberg LD and Witwer E, COVID-19 abortion bans and their implications for public health, Perspectives on Sexual and Reproductive Health, 2020, 52(2), https://doi.org/10.1363/psrh.12139.
21. American College of Obstetricians and Gynecologists (ACOG), Joint statement on abortion access during the COVID-19 outbreak, news release, 2020, https://www.acog.org/en/News/News Releases/2020/03/Joint Statement on Abortion Access During the COVID 19 Outbreak.
22. Kearney MS and Monday PL, Half a Million Fewer Children? The Coming COVID Baby Bust, Washington, DC: Brookings Institution, 2020, https://www.brookings.edu/research/half-a-million-fewer-children-the-co….
23. Martin J et al., Births: final data for 2018, National Vital Statistics Reports, 2019, 68(13):47.
24. Luppi F, Arpino B and Rosina A, The impact of COVID-19 on fertility plans in Italy, Germany, France, Spain and UK, SocArXiv, 2020, doi:10.31235/osf.io/wr9jb.
25. Ross L and Solinger R, Reproductive Justice: An Introduction, first ed., Berkeley, CA: University of California Press, 2017, https://www.ucpress.edu/book/9780520288201/reproductive-justice.
26. Chalas E and Phipps MG, COVID-19 call to action for women’s health, Washington, DC: ACOG, 2020, https://www.acog.org/advocacy/-/media/7aa1e9b4d6a846b589b714116606a33f….
27. Hall KS et al., Centering sexual and reproductive health and justice in the global COVID-19 response, Lancet, 2020, 395(10231):1175–1177, doi:10.1016/S0140-6736(20)30801-1.
28. National Women’s Law Center, Promoting equitable access to health care in response to COVID-19, 2020, https://nwlc-ciw49tixgw5lbab.stackpathdns.com/wp-content/uploads/2020/0….
29. Ahmed Z et al., Nine things Congress must do to safeguard sexual and reproductive health in the age of COVID-19, Policy Analysis, New York: Guttmacher Institute, 2020, https://www.guttmacher.org/article/2020/04/nine-things-congress-must-do….
30. Nash E et al., Ten things state policymakers can do to protect access to reproductive health care during the COVID-19 pandemic, Policy Analysis, New York: Guttmacher Institute, 2020, https://www.guttmacher.org/article/2020/05/ten-things-state-policymaker….
31. Lindberg LD, Bell DL and Kantor LM, The sexual and reproductive health of adolescents and young adults during the COVID-19 pandemic, Perspectives on Sexual and Reproductive Health, 2020, https://onlinelibrary.wiley.com/doi/abs/10.1363/psrh.12151.
32. Rasmussen SA et al., Coronavirus disease 2019 (COVID-19) and pregnancy: what obstetricians need to know, American Journal of Obstetrics & Gynecology, 2020, 222(5):415–426, doi:10.1016/j.ajog.2020.02.017.
33. Frederiksen B, Gomez I and Salganicoff A, A look at online platforms for contraceptive and STI services during the COVID-19 pandemic, San Francisco: Kaiser Family Foundation, 2020, https://www.kff.org/coronavirus-covid-19/issue-brief/a-look-at-online-p….
34. Qualtrics, Online panels: get responses for surveys & research, Panels & Samples, no date, https://www.qualtrics.com/research-services/online-sample/.
35. ESOMAR, 28 questions to help buyers of online samples, 2012, https://www.esomar.org/what-we-do/code-guidelines/28-questions-to-help-….
36. Boas TC, Christenson DP and Glick DM, Recruiting large online samples in the United States and India: Facebook, Mechanical Turk, and Qualtrics, Political Science Research and Methods, 2020, 8(2):232–250, doi:10.1017/psrm.2018.28.