Why preventing unintended pregnancy is critical
- Improving adolescents’ sexual and reproductive health, including preventing unintended pregnancy, is essential to their social and economic well-being.
- Complications of pregnancy and childbirth continue to lead to preventable deaths and ill-health among 15–19-year-old women in developing regions.1
- Adolescent childbearing is associated with lower educational attainment among mothers, and it can perpetuate a cycle of poverty from one generation to the next.1
- Roughly half of pregnancies among adolescents aged 15–19 in developing regions are unintended,1 and about half of these end in abortions,2–8 most of which are unsafe.
Adolescents’ need for contraception
- Among the 253 million women aged 15–19 in developing regions, 14% (36 million) need contraception because they are married, or are unmarried and sexually active, and do not want a child for at least two years.
- Of these 36 million adolescents, 43% (16 million) are using modern contraceptives. The most common methods are male condoms and the pill, followed by injectables.
- The other 57% (20 million) are not using a modern method; these adolescent women have an unmet need for modern contraception. Among these women, 85% are using no method at all, and the remainder use traditional methods, which are less effective than modern methods.
- Unmet need is much higher among adolescents than among all women aged 15–49 who want to avoid pregnancy (57% versus 24%). Younger adolescents aged 15–17 also generally have higher unmet need than those aged 18–19.1
- In Africa and Asia, nearly two-thirds (62% and 64%, respectively) of sexually active adolescents wanting to avoid pregnancy experience unmet need. In Latin America and the Caribbean, that proportion is 38%.
- Young women often report several reasons for not using contraceptives despite not wanting a pregnancy: infrequent sex; not being married; concerns about contraceptive side effects; breast-feeding or not having resumed menstruation after a birth; and their own, their partners’ or others’ opposition to contraception.9
Cost of meeting contraceptive needs
- Based on 2017 estimates, the annual cost of providing contraceptive services to the 16 million women aged 15–19 who currently use modern contraceptives is $276 million.
- Service costs include direct costs for contraceptives, related supplies and health worker salaries, as well as the indirect costs of management functions, construction and maintenance of facilities, information and education activities, and other types of program support.
- If services were improved for the 16 million adolescent women currently using modern contraceptives, costs would increase from $276 million to $417 million. Examples of improvements that would benefit adolescents include better contraceptive counseling and follow-up, consistent availability of a range of modern methods and providers who are trained to work with adolescents.
- If the 20 million adolescent women with unmet need were to use the same mix of modern methods as current users and receive improved services, total costs for current and new users would be $889 million each year, an increase of $613 million annually.
- A large portion of the cost increase ($379 million out of $613 million) would be for Africa because much unmet need is concentrated in this region, and health systems there are greatly in need of strengthening.
- The annual cost per user would average $25 for developing regions as a whole, ranging from $15 in Asia to $27 in Latin America and the Caribbean and $35 in Africa. Put differently, the annual cost per capita in developing regions would be 14 cents.
Benefits of meeting all contraceptive need
- Increased use of modern contraceptives by adolescents wanting to avoid pregnancy would prevent unintended pregnancies, save lives and improve health.
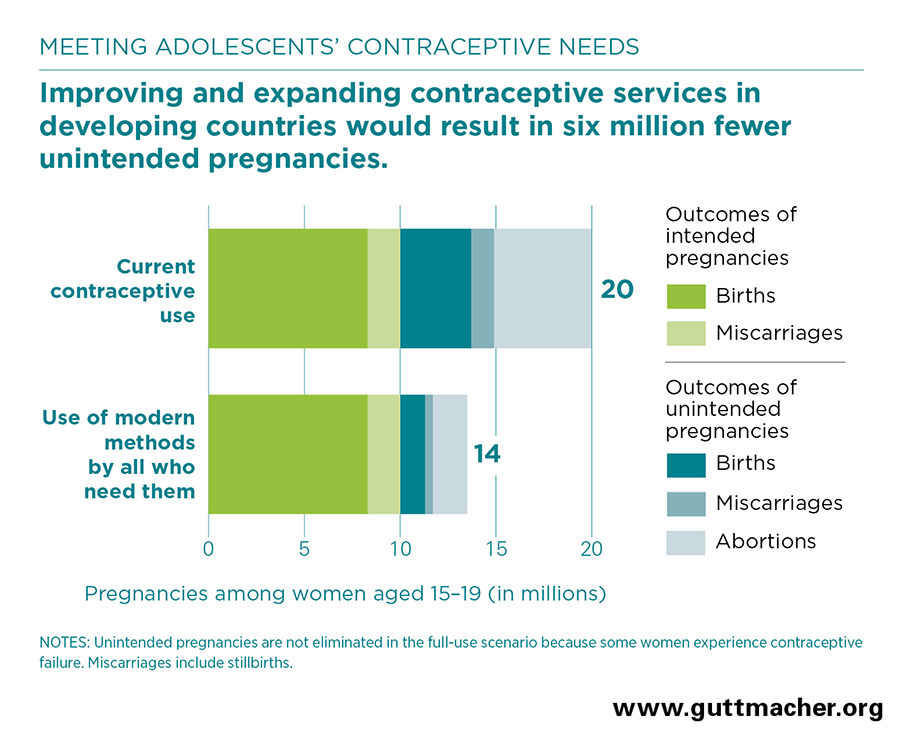
- If all adolescent women who need modern contraceptives were to use them, unintended pregnancies would decrease by six million per year (63%), and total pregnancies would decrease from 20 million to 14 million. This would result in 2.4 million fewer unplanned births; 2.9 million fewer abortions, of which 1.9 million would have been unsafe; and 763,000 fewer miscarriages and stillbirths from unintended pregnancies.
- Maternal deaths—those due to complications of pregnancy and childbearing—among women aged 15–19 would drop by 6,000 from the current level of 28,000 per year10 to 22,000. Most of the deaths averted would be in Africa (4,300), the region with the world’s highest maternal mortality.
Recommendations
- Meeting adolescent women’s contraceptive needs requires policies and practices to end child marriage, prevent sexual abuse and coercion, increase girls’ education, empower girls and women, and provide comprehensive sexuality education and high-quality contraceptive services.
- Boosting the level of education girls receive increases their ability to make autonomous decisions. Studies show that sexually active adolescents who are in school are more likely than those not in school to use contraceptives.1
- Engaging young men in sexual and reproductive health programs can also help bring about more gender-equitable attitudes.
- Adolescents need access to medically accurate and complete sexual and reproductive health information before they are sexually active. This information should be age-, developmentally and culturally appropriate. Policies and programs, including comprehensive sexuality education, should be put in place to address this need.
- The most effective approaches to providing sexual and reproductive health services to youth include a combination of health worker training; facility improvements geared toward welcoming adolescents and protecting their privacy; and information dissemination through schools, communities and the media.1
- The counseling provided with contraceptive methods must be strengthened. All adolescents need correct information about the likelihood of pregnancy, choices of contraceptive methods, information about possible side effects, and support in switching methods when desired.
- Contraceptive services must be provided in a way that protects young women’s rights to voluntary, informed and confidential contraceptive choice.