Corrected May 3, 2019. See note below.
- Modern contraceptive services and maternal and newborn health care are essential for promoting the well-being of women and their babies. Contraceptive use enables women and their partners to plan the number and timing of their children, and access to maternal and newborn care greatly improves women’s chances of having a healthy pregnancy and delivering a healthy newborn.
- Providing a comprehensive package of maternal and newborn care that includes antenatal, delivery, postnatal, HIV-related and postabortion services is costly and can pose a challenge for low-income countries. One way to manage such costs is to reduce the number of unintended pregnancies—those that occur among women who want to postpone pregnancy or stop childbearing altogether.
Need for Modern Contraception
- As of 2017, women in Nepal have an estimated 1.2 million pregnancies each year, of which 539,000 (or 45%) are unintended. Nearly a quarter of these unintended pregnancies end in unplanned births and two-thirds end in induced abortion (and the remainder end in miscarriage).
- About 44% of women aged 15–49 who want to avoid a pregnancy have an unmet need for modern contraception, meaning they are not using contraceptives at all or are using a traditional method. Most unintended pregnancies result from unmet need for modern contraception.
- Unmet need is substantial in every province of Nepal. It is highest in Gandaki Pradesh (experienced by 52% of women wanting to avoid a pregnancy) and lowest in Province 2 (38%).
Need for Maternal and Newborn Health Care
- Many pregnant women in Nepal do not receive the maternal and newborn care they need to prevent and manage health complications that may arise during pregnancy and delivery.
- According to recent data, 64% of pregnant women obtain the recommended minimum of four antenatal care visits, and 61% of births are assisted by a skilled birth attendant. Only 27% of women who experience serious medical complications during pregnancy or delivery receive the care that they or their newborns need.1
- Maternal mortality in Nepal, estimated at 239 maternal deaths per 100,000 live births in 2016,2 is higher than average for the Southern Asia region.3 This mortality ratio translates to the death of approximately 1,600 women each year.
Costs of Satisfying Unmet Needs
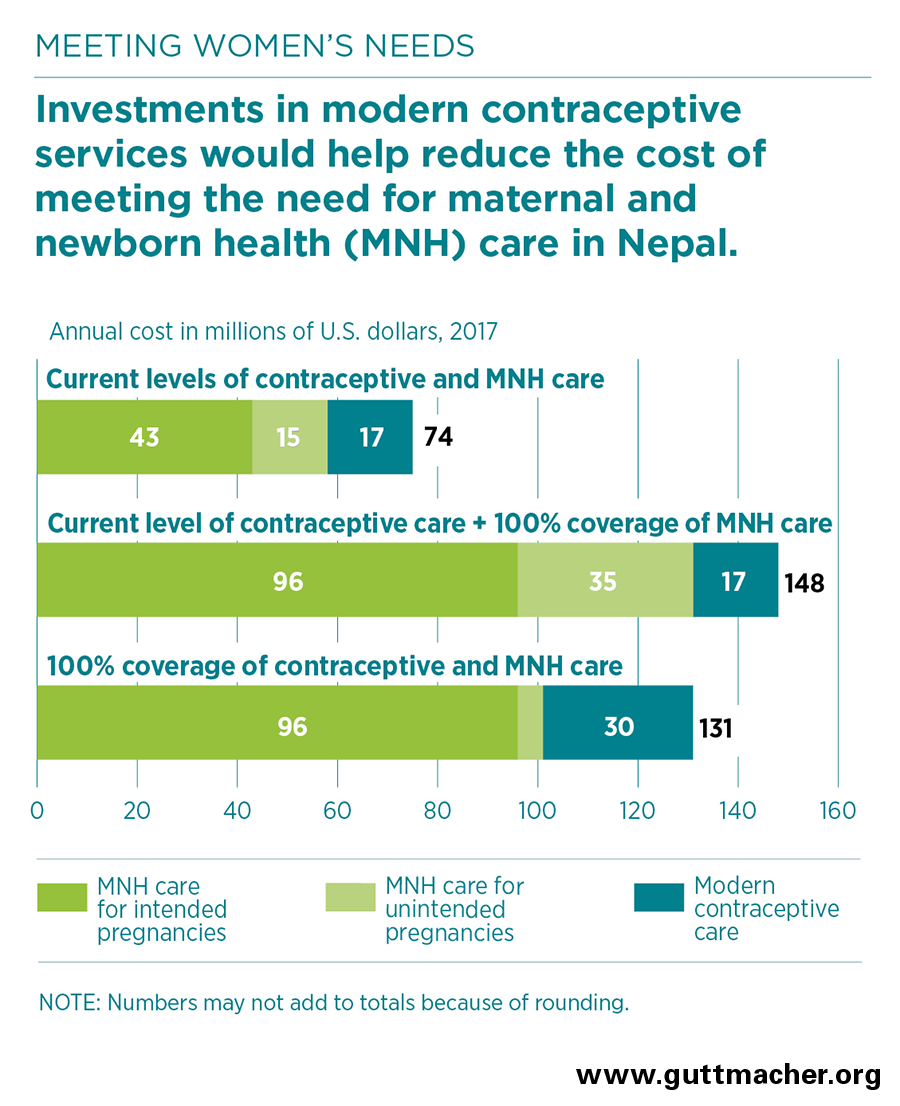
- Satisfying all women’s need for modern contraception would increase the annual cost of services from an estimated $17 million (in 2017 U.S. dollars) to $30 million. This total would include contraceptive commodities, staff salaries, health infrastructure upgrades, contraceptive counseling, communication activities, and improvements to programs and systems.
- If contraceptive services were to stay at current levels, providing all 1.2 million pregnant women each year with a comprehensive package of maternal and newborn health care would cost $131 million—about one-fourth of which would cover care for women with unintended pregnancies. This represents more than a doubling of the current cost of care.
Benefits of Meeting Reproductive Health Needs
- Because having an abortion or carrying an unintended pregnancy to term is more expensive than supporting women to prevent unintended pregnancies in the first place, expanding modern contraceptive services and maternal and newborn care simultaneously would result in cost savings compared with expanding maternal and newborn services alone.
- For every additional U.S. dollar spent on expanding modern contraceptive use, the country would save $2 on maternal and newborn health care.
- Providing modern contraceptive services and the recommended maternal and newborn health care services to all women who need them would cost $131 million: $30 million for contraceptive services and $101 million for maternal and newborn care. The country would save nearly $17 million because of the unintended pregnancies that would be averted.
- Under this scenario of fully meeting women’s needs for these services, Province 2 would see the largest cost savings ($5 million), while other provinces would save between $0.8 million and $4 million each.
- If all unmet need for modern contraception were met, unintended pregnancies would be reduced by 87%, or 469,000 annually, and unplanned births, abortions and miscarriages would decline by the same proportion. Fully meeting women’s need for contraception would reduce maternal deaths by nearly 300 annually, and even more women’s lives would be saved if all need for maternal and newborn health care were met.1
Moving Forward
- An effective strategy for managing the cost of full maternal and newborn health care coverage while also reducing maternal and infant death and disability is to lower women’s exposure to the risks of unintended pregnancy and childbirth in the first place.
- Various stakeholders share responsibility for meeting the demand for modern contraceptives: local and provincial governments, the national government, the private sector and international development partners.
- Improving publicly funded services—through increased investment and quality enhancements—is especially important for reaching disadvantaged populations. Such investments would improve the health of women and their babies and also have wider, social and economic benefits, such as reduced poverty and hunger and gains in women’s empowerment and education.4
NOTE:
Changes were made in the calculation of cost estimates in Adding It Up: Costs and Benefits of Meeting the Contraceptive and Maternal and Newborn Health Needs of Women in Nepal, based on a revised unit cost of gauze from $2.67 to $0.04. These corrections do not change the study’s summary findings or conclusions.