In India, induced abortion is legal up to 20 weeks’ gestation, yet there are no state-level representative data on the health care services available to women seeking an abortion or care for complications following an abortion. This fact sheet examines the provision of these vital services in Tamil Nadu.
Overview of the study
Between March and August of 2015, a team of researchers surveyed a sample of health facilities in six Indian states (Assam, Bihar, Gujarat, Madhya Pradesh, Tamil Nadu and Uttar Pradesh) as part of a study to generate high-quality data on the availability of induced abortion and postabortion care and the incidence of abortion and unintended pregnancy in India.
The study team randomly selected 70% of each state’s districts, and identified and sampled public, private and NGO facilities within these districts. In the public sector, district hospitals, subdivisional hospitals and community health centers (CHCs) were sampled using lists obtained from the Ministry of Health and Family Welfare (MOHFW). A portion of the primary health centers (PHCs) that are administratively linked to the sampled CHCs were also sampled. In addition, the study team listed and sampled public facilities not listed by MOHFW (urban public facilities), as well as private and NGO facilities (hospitals, medical colleges, maternity and nursing homes, and clinics) that offer induced abortion or postabortion services: In rural areas, facilities located in the catchment areas of a subsample of CHCs were listed, and in urban areas, facilities located within a sample of urban wards were listed. At each sampled facility, trained investigators conducted an in-person interview using a structured questionnaire with a senior professional knowledgeable about the provision of abortion-related services (typically the director or head of the facility or of the department responsible for obstetrics and gynecology). The study and its protocols were approved by the Institutional Review Boards of the three institutions conducting the study.
In Tamil Nadu, 23 of 32 districts were sampled for inclusion in the study. A total of 391 public facilities (including 125 that reported providing any abortion-related service) completed the survey, as did 285 private facilities and seven NGO facilities that provide abortion-related services. These represent all 2,261 public facilities operating in the Tamil Nadu (including 459 that provide abortion-related services), as well as the 2,776 private and NGO facilities offering abortion or postabortion care in the state. Our analysis differentiates facilities according to ownership (public or private) and type (grouped into categories that generally correspond to facility capacity*). Because NGOs make up a very small proportion of our sample, they were combined with private facilities in this analysis. Detailed distributions in tables and figures do not always sum to 100 because of rounding.
Public and private facilities offering abortion-related services
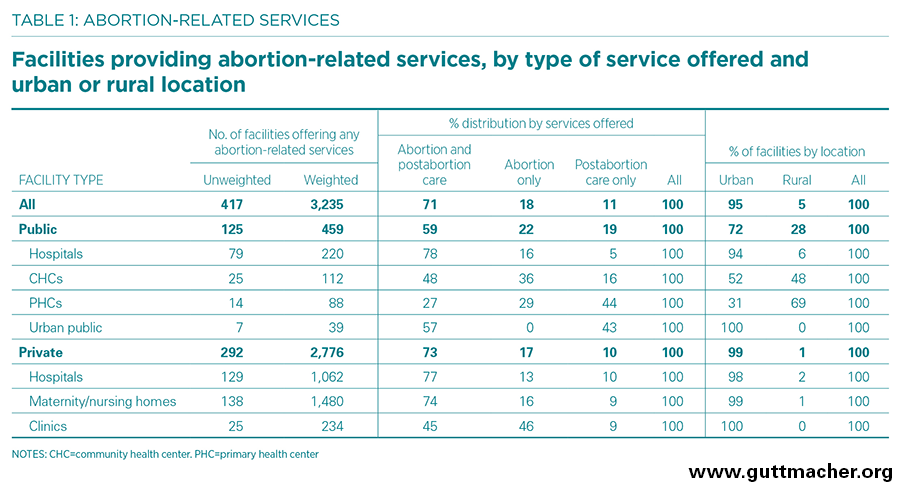
- An estimated 3,235 facilities in Tamil Nadu provide abortion-related services (induced abortion, postabortion care or both; Table 1). Of these, 459 are public and 2,776 are private (including NGOs).
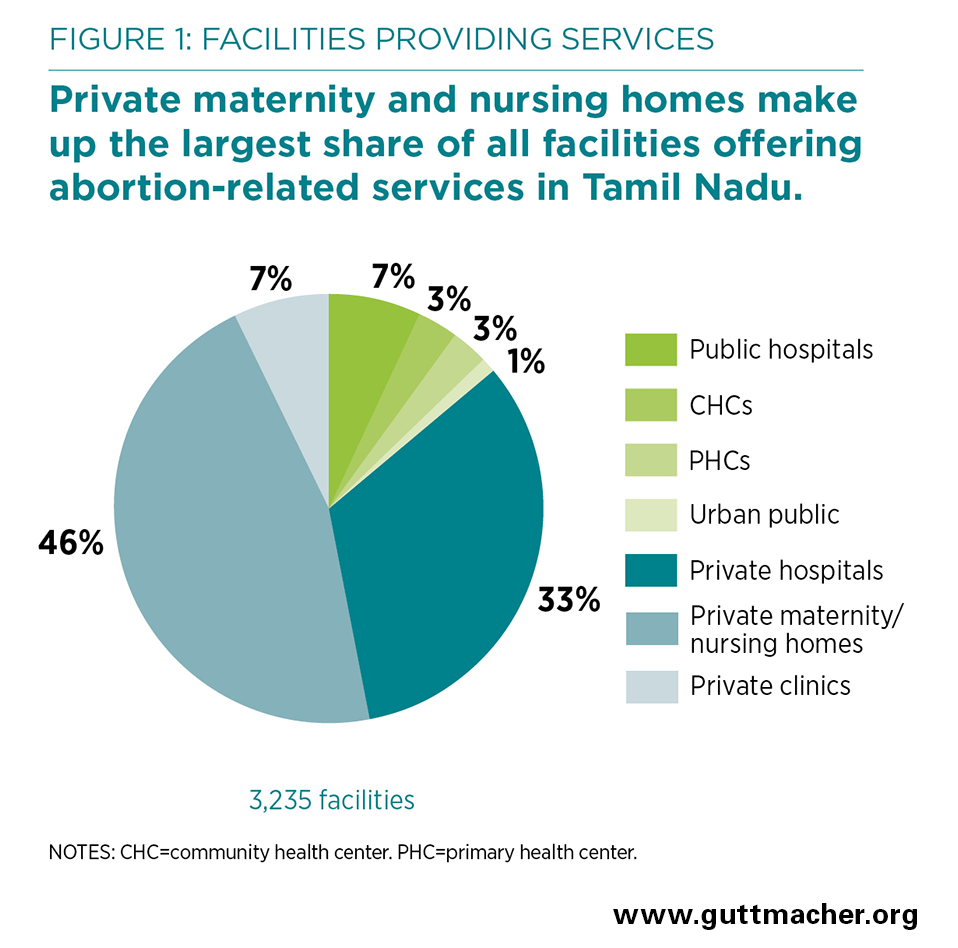
- Private maternity and nursing homes make up the largest share of all facilities offering abortion-related services, accounting for 46%, followed by private hospitals which account for 33% (Figure 1).
- Among facilities offering any such services, 71% offer both abortion and postabortion care, 11% offer only postabortion care, and 18% offer only abortion.
- About three-quarters of public hospitals (78%), private hospitals (77%) and private maternity and nursing homes (74%) that offer any abortion-related services provide both types of care.
- In contrast, among urban public facilities and primary health centers (PHCs) that offer any abortion-related services, 43-44% provide only postabortion care.
- Most facilities offering abortion or postabortion care (95%) are located in urban areas. The large majority (86%) of these urban facilities are privately owned.
- In rural areas, on the other hand, the facilities offering abortion-related services are primarily public (79%).
- Among private facilities offering induced abortion, 74% report that they are certified under the Medical Termination of Pregnancy Act to provide this service.
Availability of abortion-related services in the public sector
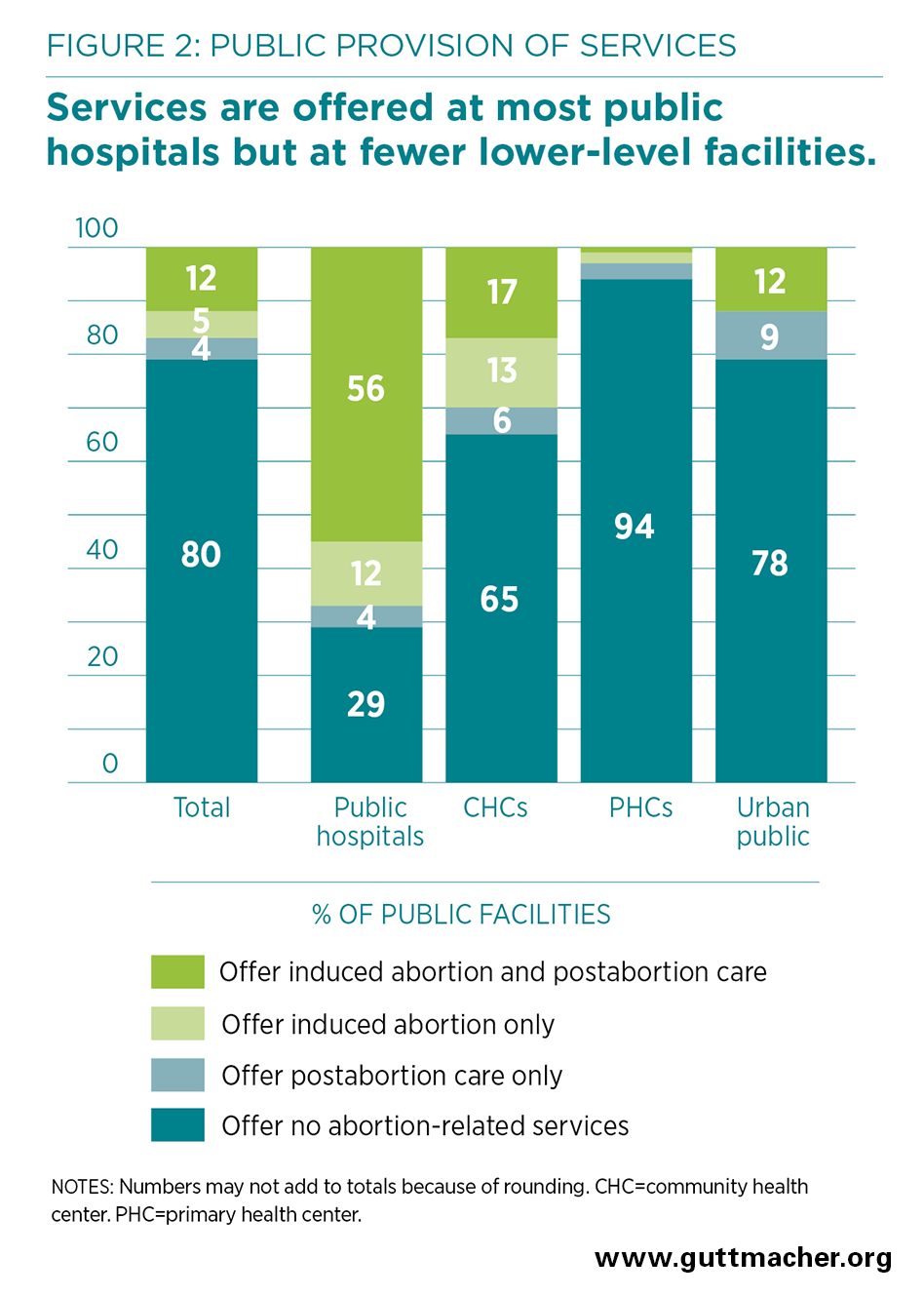
- Only 20% of all public facilities in Tamil Nadu offer any type of abortion-related services (Figure 2). Twelve percent of public facilities in the state offer both induced abortion and postabortion care, 4% offer only postabortion care and 5% offer only abortion. Eighty percent of public facilities offer neither service.
- Public provision of abortion-related services varies by facility type: Nearly three-quarters (71%) of hospitals, 35% of community health centers (CHCs) and 22% of urban public facilities offer abortion, postabortion care or both, whereas only 6% of PHCs do so.
- Seventeen percent of public facilities in Tamil Nadu provide induced abortion—67% of hospitals, 30% of CHCs, 3% of PHCs and 12% of urban public facilities—and some of these facilities also offer postabortion care (56% of hospitals, 17% of CHCs, 12% of urban public facilities and 2% of PHCs offer both).
- Overall, 16% of public facilities provide postabortion care, and a fairly small proportion offer only postabortion care: 4% of hospitals, 6% of CHCs, 3% of PHCs and 9% of urban public facilities.
- Viewed another way, the data show that a large majority (83%) of public facilities—33% of hospitals, 70% of CHCs, 97% of PHCs and 88% of urban public facilities—do not offer abortion.
Reasons for not offering abortion
- Among facilities whose abortion-related services are restricted to postabortion care, the reasons reported for not offering induced abortion vary according to whether facilities are public or private.
- Public facilities offering only postabortion care commonly cite lack of trained staff (75%) and lack of equipment or supplies (54%) as reasons for not offering abortion.
- In contrast, private facilities offering only postabortion care most commonly report lack of trained staff (37%), religious or social reasons (33%) and lack of certification (32%) as grounds for not offering the procedure; few private facilities report lack of equipment or supplies (8%).
- Among all public facilities not offering abortion—including those that offer no abortion-related services, as well as those offering only postabortion care—the most prevalent reasons reported for not doing so are the same as those reported by public facilities offering only postabortion care: lack of trained staff (77%) and lack of equipment or supplies (37%).
- Reasons are similar across all types of public facilities. Among all public hospitals not offering abortion, lack of trained staff is the main reason cited (84%), followed by lack of equipment or supplies (26%). CHCs and PHCs cite lack of trained staff (76–78%), equipment or supplies (29–39%) and space (16–27%) as the main reasons for not providing abortions.
Types of abortion procedures offered
- Among the public and private facilities that provide induced abortion, 79% offer both medical methods of abortion (MMA)† and surgical methods, 15% offer only MMA, and 6% offer only surgical methods.
- Facilities offering abortion report using the following specific methods: MMA using combipacks containing misoprostol and mifepristone (offered by 89%); MMA using only misoprostol (75%); manual vacuum aspiration (MVA) or electric vacuum aspiration (EVA) procedures (49%); dilatation and evacuation or dilatation and curettage (77%).
- Nearly four-fifths of private facilities (79%) and public facilities (78%) that offer abortion use both MMA and surgical methods.
- Sizable proportions of lower-level public facilities that offer abortion report that provision is limited to surgical methods (33% of CHCs, 34% of PHCs and 25% of urban public facilities), while the majority of private clinics (67%) offer only MMA.
Vacuum aspiration equipment and training
- In Tamil Nadu, nearly all facilities that offer abortion using MVA or EVA (95–97%) have functional equipment available at least some of the time and at least one provider trained in the procedure.
- A similar proportion (93–95%) of facilities offering these procedures have a trained provider and have functional equipment available all or most of the time when it is needed. This proportion is lowest among private clinics offering MVA (56%).
Gestation at which abortion services are offered
- In India, abortion is legal up to 20 weeks’ gestation; for abortions performed between 12 and 20 weeks, authorization by two doctors is required. Pregnancies beyond 20 weeks may be terminated only to save a woman’s life.
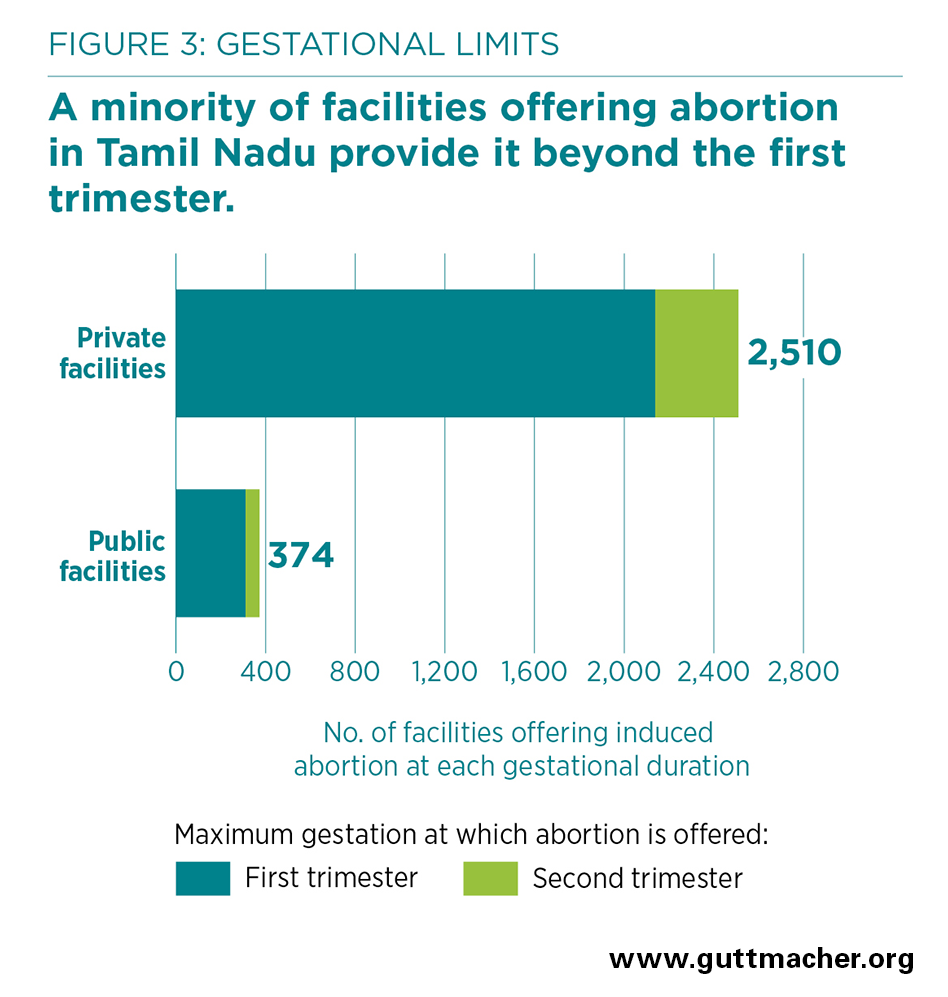
- However, the large majority of facilities providing induced abortion in Tamil Nadu—85%—offer procedures during the first trimester only (at or before 12 weeks); 23% of facilities restrict provision to the first seven weeks of pregnancy. All CHCs, PHCs, urban public facilities and private clinics that offer abortion do so only in the first trimester.
- Among the 2,510 private facilities offering abortion, 15% provide services during the second trimester of pregnancy (Figure 3). Among the 374 public facilities offering such care, 17% provide second-trimester procedures.
- Abortion provision beyond the first trimester is similarly low in urban and rural areas (15% and 18%, respectively).
Consent for abortion procedures
- Providers are required to obtain a woman’s consent before performing an abortion, and 84% of facilities report this is commonly done.
- Consent is not legally required from anyone other than the woman obtaining the procedure, unless she has a mental illness or is a minor. However, the vast majority of facilities (92%) routinely seek the consent of the woman’s husband or partner. Twenty-three percent report commonly asking for consent from married women’s in-laws, and 8% report commonly asking the parents of unmarried women.
Turning away abortion seekers
- Overall, an estimated 16% of women seeking induced abortion from facilities offering abortion in Tamil Nadu were turned away—18% of women seeking abortion from private facilities and 4% seeking abortion from public facilities.
- Half (51%) of facilities offering induced abortion report having turned away one or more women seeking an abortion in the last year. Among these facilities, the most common group of reasons for turning away abortion seekers was related to capacity to provide needed abortion services—including that the pregnancy was too far along for the facility or that the facility lacked a trained provider (67% of facilities that turned away any abortion seekers reported one or both of these reasons).
- Facilities also report turning away some women who could have been served. One-fifth (22%) of facilities that turned away women seeking abortion did so for one or more of the following reasons: the woman was "too young," had no children or was unmarried. A small proportion of facilities that turned away abortion seekers (6%) did so because the woman’s husband or partner had not consented to the procedure
Accessibility of postabortion care
- Seventy-six percent of facilities providing postabortion care services (including the majority of facilities of every type) offer care 24 hours a day, seven days a week.
- Availability of around-the-clock postabortion services is similarly high among facilities providing this care in rural areas (80%) and urban areas (76%). In rural areas, care is available 24-7 at all public hospitals, 88% of CHCs and 57% of PHCs.
- Sixty-five percent of facilities offering postabortion care services provide both outpatient and inpatient care. However, 25% of public facilities and 21% of private facilities offer outpatient services only, indicating that they may not have the capacity to treat severe complications.
- The majority of PHCs (61%), urban public facilities (57%) and private clinics (68%) offer outpatient services only.
Contraceptive care offered
- Nearly all facilities in Tamil Nadu that offer abortion-related care report providing information about family planning to the vast majority of women seeking induced abortion or postabortion care services.
- Although many of these facilities cover the correct use of methods (70%), information on what methods are available (51%), and the advantages and disadvantages of different methods (47%), only a small minority provide information on what to do in case of method failure or incorrect use (8%).
- All facilities that offer abortion or postabortion care also provide contraceptives. These facilities report that, on average, seven out of 10 women seeking abortion-related services adopt a contraceptive method. Although contraceptive uptake is roughly comparable across most types of facilities (61–86%), it is somewhat lower among women attending PHCs (44%) and private clinics (47%).
- Nineteen percent of facilities (21% of public facilities and 18% of private facilities) that offer induced abortion report that at least some women are required to adopt contraception as a condition of receiving an abortion.