- Modern contraceptive services and maternal and newborn health care are essential for protecting the health of Pakistani women, their families and communities.
- Based on data from 2017, women in Pakistan have an estimated 3.8 million unintended pregnancies each year, most of which result from unmet need for modern contraception.
- About 52% of married women of reproductive age (15–49) who want to avoid a pregnancy are not using a modern contraceptive method. If all unmet need for modern contraception were met, there would be 3.1 million fewer unintended pregnancies annually, 2.1 million fewer induced abortions and nearly 1,000 fewer maternal deaths.
- Pakistan is currently spending US$81 million per year on contraceptive services. Serving the full unmet need for modern contraception would require an additional US$92 million per year, for a total of US$173 million, based on public-sector health care costs.
- At current levels of contraceptive use, providing maternal and newborn health care to all women who have unintended pregnancies, at the standards recommended by the World Health Organization, would cost an estimated US$298 million.
- If all women wanting to avoid a pregnancy used modern contraceptives and all pregnant women and their newborns received the recommended care, the country would save US$152 million, compared with a scenario in which only maternal and newborn health care were increased. Punjab would see the largest savings (US$109 million).
- The combined investments would be cost-effective: For every additional dollar spent on expanding modern contraceptive use, the country would save more than US$2.50 on maternal and newborn care.
- Provincial governments, the federal government, the private sector and international development partners must all increase their investment in modern contraceptive services to fully meet the need for modern contraception.
Adding It Up: Costs and Benefits of Meeting the Contraceptive and Maternal and Newborn Health Needs of Women in Pakistan

Author(s)
Aparna Sundaram, Rubina Hussain, Zeba A. Sathar, Sabahat Hussain, Emma Pliskin and Eva WeissmanReproductive rights are under attack. Will you help us fight back with facts?
Key Points
Introduction
Access to reproductive health services, including maternal and newborn health care and contraceptive services, is essential for protecting the health of Pakistani women and their children. Maternal and newborn health care greatly improves women’s health outcomes during pregnancy and delivery, in addition to improving the health of their newborns, while contraceptive use enables women and their husbands to have the number of children they want, when they want them.
Receiving needed maternal and newborn care can mean the difference between life and death for pregnant women and newborns, and appropriate services can also prevent the short- and long-term effects of pregnancy-related injuries, infection and disabilities.1 Since the health of mothers and their newborns are inextricably linked, preventing death and disability requires implementing many of the same interventions for both woman and child, such as antenatal care, skilled assistance during delivery and access to emergency obstetric care.
However, providing a comprehensive package of maternal and newborn health services* can be costly for a middle-income country like Pakistan. One way to manage the costs of providing such care to all women who need it is to reduce the number of unintended pregnancies—i.e., pregnancies experienced by women who want to postpone or stop childbearing. This also allows women to have the number of children they want and to time their pregnancies as desired. Reducing unintended pregnancies depends in part on whether couples have access to modern contraceptive methods† and elect to use them. In Pakistan, the use of modern methods among all married women of reproductive age (15–49) increased from 9% in 1990–1991 to 26% in 2012–2013.2,3 Contraceptive use remains at that still fairly low level: According to the most recent Pakistan Demographic and Health Survey (PDHS) in 2017–2018, 25% of married women were using a modern method of contraception.4 Substantial unmet need for modern methods persists (experienced by 17% of all married women in 2017–2018), contributing to high unintended pregnancy levels and the health risks they entail, such as increased risk of maternal death and disability.
In this report, we discuss the need for and costs and benefits of expanding sexual and reproductive health services in Pakistan in two key areas: modern contraceptive services and maternal and newborn health care. Estimates are presented at both the national and subnational levels (see box).
Results are estimated for women aged 15–49 and their newborns needing these services. We show the current levels of services provided and the health benefits that accrue from current services, as well as the savings that would accrue if the public health sector were to meet 100% of service needs. We estimate the costs of current services and of fulfilling the unmet need for services, based on public-sector costs for services, including the cost savings that would result from meeting all needs for contraceptive services and maternal and newborn health care simultaneously. These analyses are described in the Methods section.
The Pakistan national government has committed to ensuring universal access to sexual and reproductive health care and to investing in the expansion of contraceptive services, as part of its commitments to the Family Planning 2020 (FP2020) global partnership and as a signatory to the United Nations’ Sustainable Development Goals.5–7 These commitments are also reinforced by the recommendations made by the Council of Common Interests based on the Supreme Court of Pakistan’s 2018 task force on population growth.8 The findings presented in this report provide evidence to help policymakers and donors gauge how much increased investment in reproductive health services is required, and how increased service provision will reduce unintended pregnancy, maternal mortality and morbidity in Pakistan.
The Pakistan Context
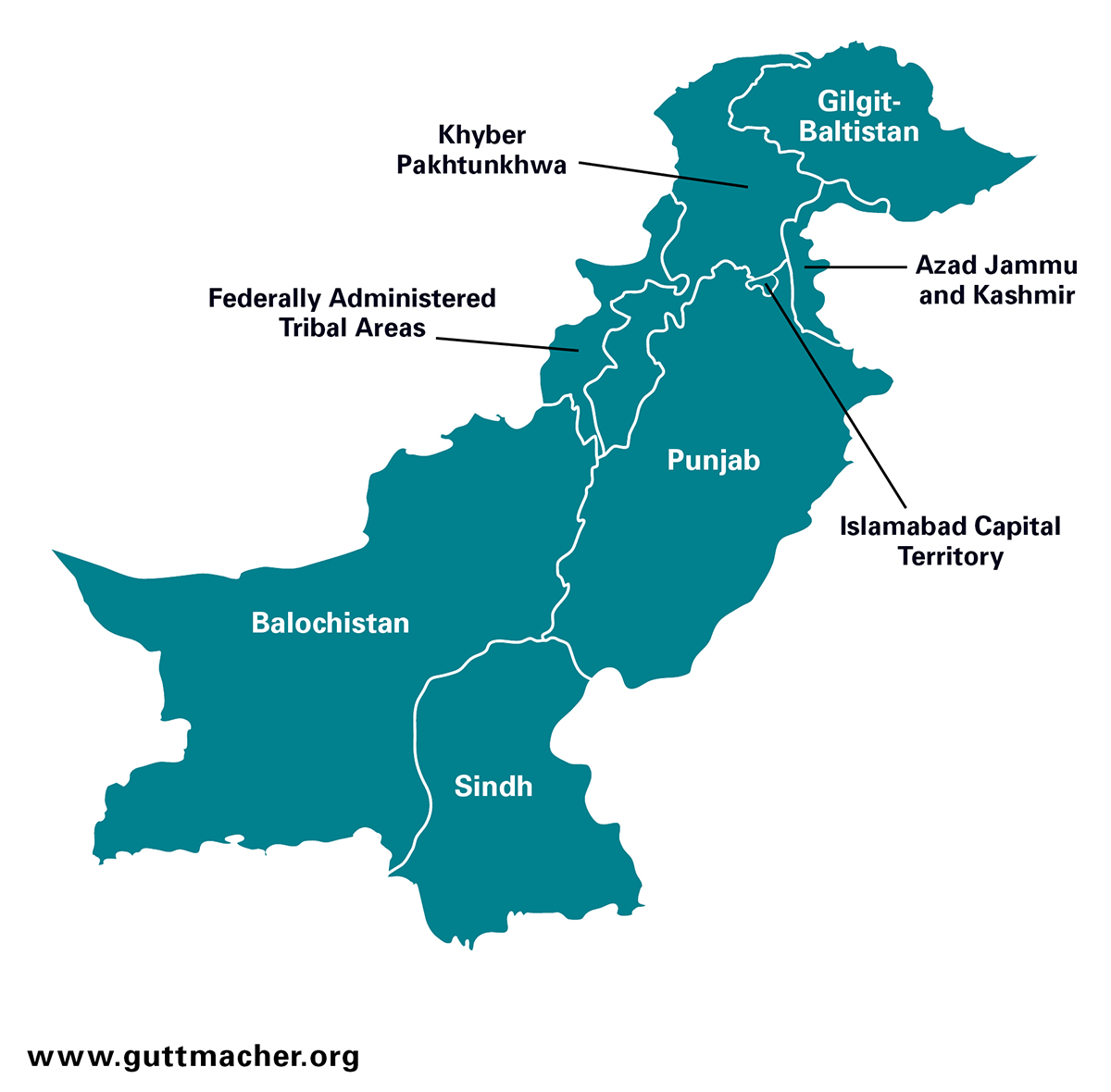
Pakistan is the sixth most populous country in the world, with a population of 213 million.9,10 This culturally and ethnically diverse country has a mostly agrarian, though rapidly urbanizing, population. Pakistan is divided into four provinces: Balochistan, Khyber Pakhtunkhwa, Punjab and Sindh; two regions: Azad Jammu and Kashmir, and Gilgit-Baltistan; and two other administrative areas: the former Federally Administered Tribal Areas (FATA) and Islamabad Capital Territory (ICT).4 For the purposes of this report, all of these administrative units will be referred to as regions when described together.
Punjab is the most populous region with approximately 110 million people, followed by Sindh (48 million people) and Khyber Pakhtunkhwa (31 million).9 Women of reproductive age (15–49) constitute nearly one-quarter of the total population, and the majority of women live in rural areas in all regions except Sindh and ICT, where about half of women live in urban areas.9,11
The sociodemographic characteristics of women vary widely across regions. Nationally, a little more than one-third of women aged 15–49 have had at least some secondary education, ranging from 5% in FATA to 58% in ICT. About a quarter of Pakistan’s population is classified as living below the poverty level, according to the Pakistan Planning Commission,12 with wide variance by province. Balochistan has the highest proportion (41% of the population); the lowest proportions are in Azad Jammu and Kashmir (18%) and Punjab (21%).
Methods
This report is part of the ongoing Adding It Up project by the Guttmacher Institute, international organizations and a number of country-specific organizations, including the Population Council, Pakistan. The methods used in our analysis are based on the Adding It Up methodologies published in 2016 and 2018;13,14 they are described briefly here and in more detail in the Methodology Appendix (download above). This report uses a range of sources to provide context regarding the current state of reproductive health in Pakistan. We also conduct original analyses to estimate current use of and need for modern contraceptive services and maternal and newborn health care, as well as the costs and benefits of providing these services.
We estimate the benefits of expanded modern contraceptive services in terms of reductions in unintended pregnancies, maternal deaths, disability-adjusted life years (DALYs)‡ and abortions, most of which are unsafe. In addition to providing these estimates for the current level of modern contraceptive use, we discuss the costs and benefits of two hypothetical scenarios of contraceptive use: a scenario in which no women use modern contraceptives and an ideal scenario in which all women who need modern contraception use it (i.e., 100% of unmet need is satisfied). In the first scenario, maternal and newborn health care is held constant at current levels, and in the other scenario, need for these services is fully met. We define women with an unmet need for modern contraception as those who want to avoid pregnancy but are using either traditional methods (i.e., withdrawal, periodic abstinence and folk methods—which typically have high failure rates) or no method.§ We define women who want to avoid a pregnancy as those who are able to become pregnant, but who want to postpone their next birth for two or more years, or who want to stop childbearing altogether.**
Next, the report provides estimates of the costs of expanding maternal and newborn health care to all women who need it, as well as the costs and savings associated with simultaneously expanding modern contraceptive services and maternal and newborn health care.†† We estimate current costs, as well as costs under three hypothetical scenarios: a scenario in which no women use modern contraception and maternal and newborn health care is provided at the current level; a scenario in which maternal and newborn care is provided to all women who need it and modern contraceptive services remain at current levels; and an ideal scenario in which both modern contraceptive services and maternal and newborn health care are provided to all women who need them.
All analyses are based on the costs of care in the public sector, under the assumption that the government has a mandate to provide these services; we make no assumption about who pays for care or what proportion of the total is paid directly by individuals. In reality, the costs could be higher if a large proportion of women seek these services in the private sector, where costs are highly variable; the costs presented in this report may therefore be considered to be minimum estimates.
Unless otherwise noted, the data were calculated using the following methods and sources. All estimates concerning women in need of contraceptive and maternal and newborn health care services are for married women of reproductive age (15–49) in 2017 and are shown for the country as a whole and for each region; they are broken down according to women’s socioeconomic status, as measured by the 2017–2018 PDHS.4 Where necessary, we projected estimates to 2017 from the most recent available data. The national and regional numbers of women of reproductive age were estimated using data from the 2017 Pakistan Population and Housing Census and the proportions of women who were married, in each wealth quintile and living in each region, were obtained from the 2017–2018 PDHS and applied to the total number of women of reproductive age.4,9 Numbers of women who desire to avoid pregnancy and use contraception were also calculated using data from the 2017–2018 PDHS.
We calculated numbers of unintended pregnancies in each region at current levels of contraceptive use, as well as for the hypothetical scenarios, using contraceptive use failure rates and pregnancy rates for nonusers from the 2017–2018 PDHS and other sources.11,13–17 Pregnancy intendedness and pregnancy outcomes were estimated using calculations of data from three key sources: the 2017–2018 PHDS (to obtain regional number of births and their status as either planned or unplanned), a 2012 national abortion incidence study (to arrive at regional abortion estimates) and a clinical study estimating miscarriage.11,18,19 The number of pregnancy-related deaths was projected to 2017 using the most recent province-level estimates of the maternal mortality ratio (MMR) from the 2006–2007 PDHS and results from the regression model used by the World Health Organization (WHO), United Nations Children’s Fund (UNICEF) and United Nations Population Fund (UNFPA).20–22 As estimates of the MMR and abortion incidence were unavailable for some regions, we used national estimates for Azad Jammu and Kashmir, the former Federally Administered Tribal Areas (FATA) and Gilgit-Baltistan; for Islamabad Capital Territory (ICT), Punjab’s MMR and the national abortion estimate were used. National estimates of pregnancy-related DALYs among women were obtained from the Institute for Health Metrics and Evaluation.23
Costs of contraceptive services and maternal and newborn health care were estimated using an ingredients-based costing method: For each contraceptive method or health care intervention, we combined the direct costs (in 2017 U.S. dollars) of drugs, supplies and materials, labor and hospitalization, with the indirect costs (also known as programs and systems costs, which include management, infrastructure, communications and outreach) to arrive at an annual cost of protection against unintended pregnancy for each woman receiving pregnancy-related medical care.14,24 Direct costs of contraceptives were taken from UNFPA’s Reproductive Health Interchange database, drug and supply costs came from international prices in the UNICEF Supply Catalogue, and the cost of labor (salaries for different categories of medical professionals) was based on derivations from estimates used in the Essential Package of Health Services for Primary Health Care accepted by most of the provinces.25–31
Maternal and Newborn Services
Survey data show improvements over time in some areas of maternal health care use, such as an increase in antenatal care overall and a rise in the number of births taking place in health facilities, but a large proportion of pregnant women in Pakistan still do not receive the maternal and newborn care they need.1,2,4 Only half of pregnant women in 2017–2018 obtained the recommended minimum of four antenatal care visits with a health care professional.‡‡11 About two-thirds of recent births (69%) in that timeframe were delivered in a health facility and 72% of births were delivered by a skilled birth attendant, compared with 53% and 57%, respectively, in 2012–2013.32 These components of care are crucial for preventing and managing the health complications that could arise during pregnancy and delivery.
One consequence of inadequate coverage of pregnancy-related care is its contribution to high maternal mortality: In 2015, there were 178 maternal deaths per 100,000 live births nationally, and maternal mortality ranged widely across provinces.22,33 In 2017, there were an estimated 10,000 maternal deaths in Pakistan.49 Maternal mortality is likely to be disproportionately high among disadvantaged women—those who are poor, live in rural areas or have little education—because they tend to have poor access to adequate health care.34,35 A national maternal mortality estimate is expected later in 2019, and there is reason to believe it will be lower than previous estimates due to the rise in skilled birth attendance.2,4,20
For every woman who dies from complications of pregnancy and childbirth, many others will suffer illness and disability from these complications. In addition to the personal costs related to pain and ill-health, such morbidity has a wide range of potential social and economic ramifications, including impinging on a mother’s ability to care for her newborn or other members of her family, and limiting her participation in the workforce. Maternal death and morbidity resulted in an estimated 1,144,000 DALYs in Pakistan in 2017.23
Unsafe abortions—meaning those that are carried out by individuals without the necessary skills, or in an environment that does not conform to the minimum medical standards, or both—carry a high risk of complications that endanger women’s health and lives. These complications account for an estimated 6% of maternal deaths in Southern Asia as a whole.36 Unlike other Southern Asian countries such as India and Nepal, induced abortion is highly restricted by law in Pakistan.18,37,38 Abortion is legally allowed only to save the life of a woman or to provide her with "necessary treatment."18,39 A recent study on abortion incidence in Pakistan estimated that there were 2.25 million abortions in 2012, most of which were unsafe.18 More than a quarter of these abortions resulted in complications that were treated in a health facility, and many other complications went untreated. According to the study, about 712,000 Pakistani women in 2012 were treated for postabortion complications, the vast majority of which could have been prevented.
For women who carry their pregnancies to term, the health care they receive during pregnancy directly affects the health of their newborns.1,40 Pakistan’s neonatal mortality rate fell from 55 deaths in the first 28 days of life of life per 1,000 live births in 2012–2013 to 42 deaths per 1,000 in 2017–2018; however, it is well above the overall Southern Asia median rate of 28 and far higher than most developed nations.2,4,41 In Pakistan and globally, the majority of newborn deaths are due to severe infections, asphyxia and preterm births, all of which are preventable.2,4,42
In Pakistan, many maternal and newborn care interventions have been designed and implemented over the past decade, but much more needs to be done to protect women and their newborns, given gaps in receipt of services.43–48 Expanding such care would reduce women’s exposure to the substantial risks inherent in pregnancy and childbearing. Preventing unintended pregnancies would reduce these risks even further.
Unintended Pregnancy
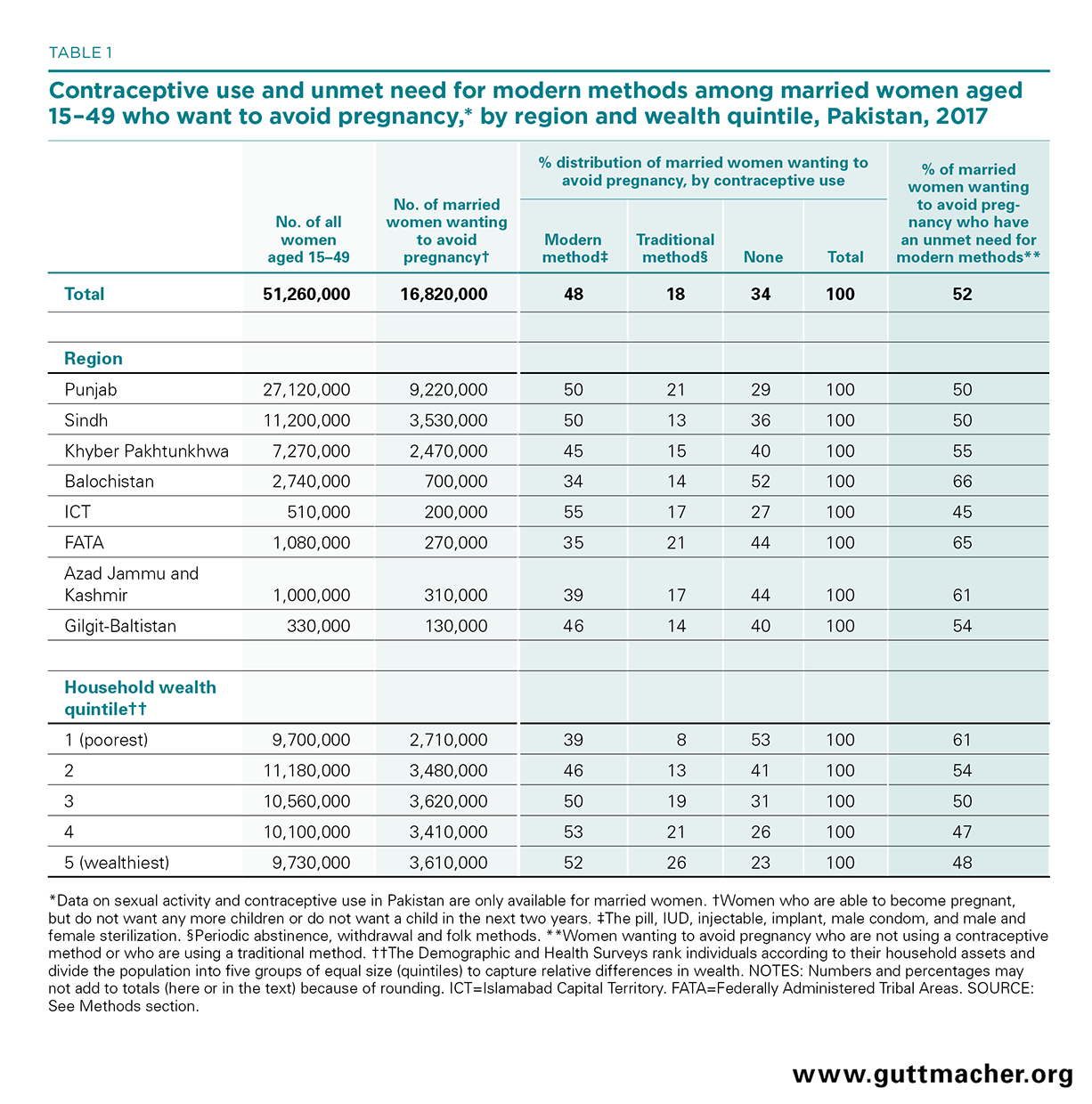
About 16.8 million married women of reproductive age (15–49) in Pakistan want to avoid a pregnancy (Table 1)—that is, they are able to become pregnant but want to either delay childbearing for at least two years or stop having children.
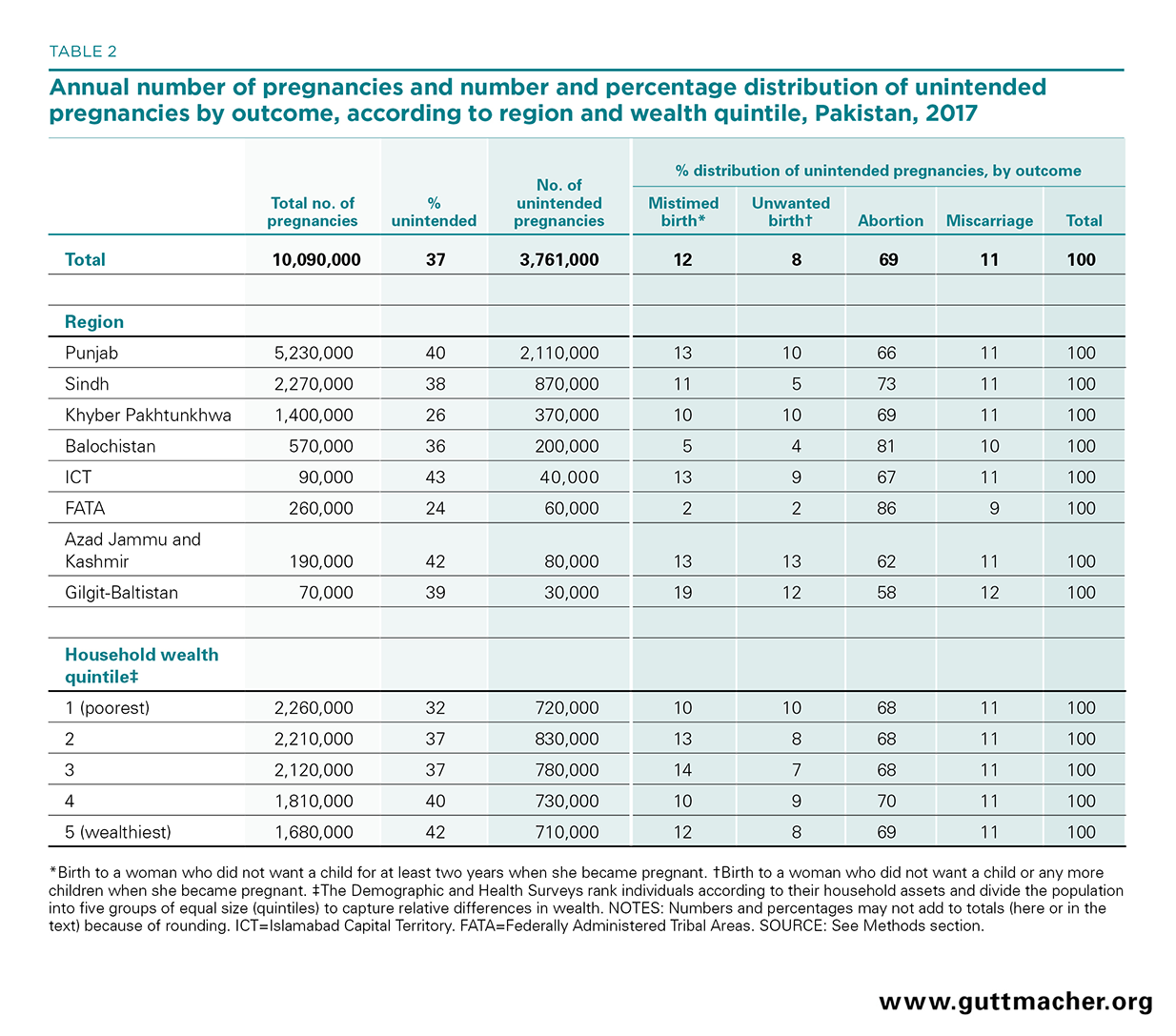
An estimated 10.1 million pregnancies occur each year in Pakistan, and 3.8 million (37%) of them are unintended, according to the most recent data (Table 2).49 One-fifth (20%) of these unintended pregnancies end in unplanned births, and more than two-thirds (69%) end in induced abortion. Pakistani women report wanting an average of 2.9 children but end up having 3.6; this translates to an average of 0.7 children per woman whose births were mistimed or unwanted.4
The proportion of pregnancies that are unintended varies by region, from 24% in FATA to 43% in ICT.49 The proportion of unintended pregnancies that are terminated also varies across regions, from 58% in Gilgit-Baltistan to 86% in FATA. At least one-third of pregnancies are unintended across all socioeconomic levels nationally.
In many cases, a woman’s likelihood of experiencing an unintended pregnancy depends on whether she and her husband use a modern contraceptive method and whether they do so correctly and consistently.15,50,51 The most effective modern methods are sterilization, long-acting reversible methods (e.g., IUDs and implants) and injectables. Following those are other hormonal contraceptives, such as the pill, and then condoms; these modern methods are more effective than traditional methods, such as periodic abstinence and withdrawal.15
The majority (77%) of unintended pregnancies are among women not using contraceptives, and 14% are among women using traditional methods (not shown).49 Only 9% of unintended pregnancies are due to failure of a modern method. Among married women with unmet need for contraception (i.e., those who want to avoid pregnancy but are not using a modern or traditional contraceptive method), the most commonly cited reasons for not using any method are personal opposition (29%), infrequent or no sexual activity (26%), fear of side effects or health risks (25%), husband, family member’s or other person’s opposition (17%), and breast-feeding or postpartum amenorrhea (16%).11 Few women mentioned factors directly related to availability of services as their reason for not using contraception. These results make clear that strategies to help Pakistani women achieve their fertility desires will likely entail more than simply making contraception available; extensive improvements in the quality of contraceptive services are needed. These include: increased numbers of providers and outreach workers, improved training for providers, provision of nonjudgmental care, accurate information and education about contraceptive methods and pregnancy risk, personalized counseling, follow-up care and support for switching methods.
Modern Contraceptive Use
About one-third (36%) of all married Pakistani women who want to avoid a pregnancy prefer to wait at least two years before having a child and about two-thirds (64%) prefer to stop childbearing altogether (not shown).49 However, only 48% of married women who want to avoid pregnancy are using a modern contraceptive method (Table 1). About 18% of those wanting to avoid pregnancy rely on a traditional method (mostly withdrawal and periodic abstinence) and 34% use no method at all. Taken together, 52% of married women who want to avoid pregnancy are not using a modern method, meaning they have an unmet need for modern contraception.
The proportion of married women wanting to avoid a pregnancy who have an unmet need for modern contraception varies by geographic area but is substantial in all regions of Pakistan. It is highest in Balochistan (66%), followed by FATA (65%), Azad Jammu and Kashmir (61%), and Khyber Pakhtunkhwa (55%). About half of women wanting to avoid pregnancy have an unmet need in Punjab and Sindh, and 45% in ICT. Although the proportion of married women wanting to avoid pregnancy and using no contraceptive method is highest among the poorest women (53%) nationally, the proportion using traditional methods is highest among the wealthiest women (26%). Overall, unmet need for modern contraception is higher among the poorest women (61%) compared with the wealthiest (48%).
Female sterilization and condoms are the most commonly used contraceptive methods in Pakistan, accounting for 71% of all modern method use among married women (data not shown).4 Ten percent of modern method users rely on injectables, 9% on IUDs, 7% on the pill, and 2% on the implant.
Among married women who want to avoid a pregnancy, 48% are using modern methods. A substantially higher proportion of those who wish to stop childbearing altogether use a modern method, compared with those who wish to space their births (57% vs. 33%). The desire to limit childbearing is reflected by the relatively high level of reliance on female sterilization among contraceptive users.
Benefits of Increased Contraceptive Use
Comparisons between scenarios of contraceptive use among married women wanting to avoid pregnancy can show the extent to which current modern contraceptive services are preventing unintended pregnancies. Such comparisons can also demonstrate the extent to which unmet need for modern contraception might decline—and the incidence of unintended pregnancy along with it—as investment in modern contraception increases.
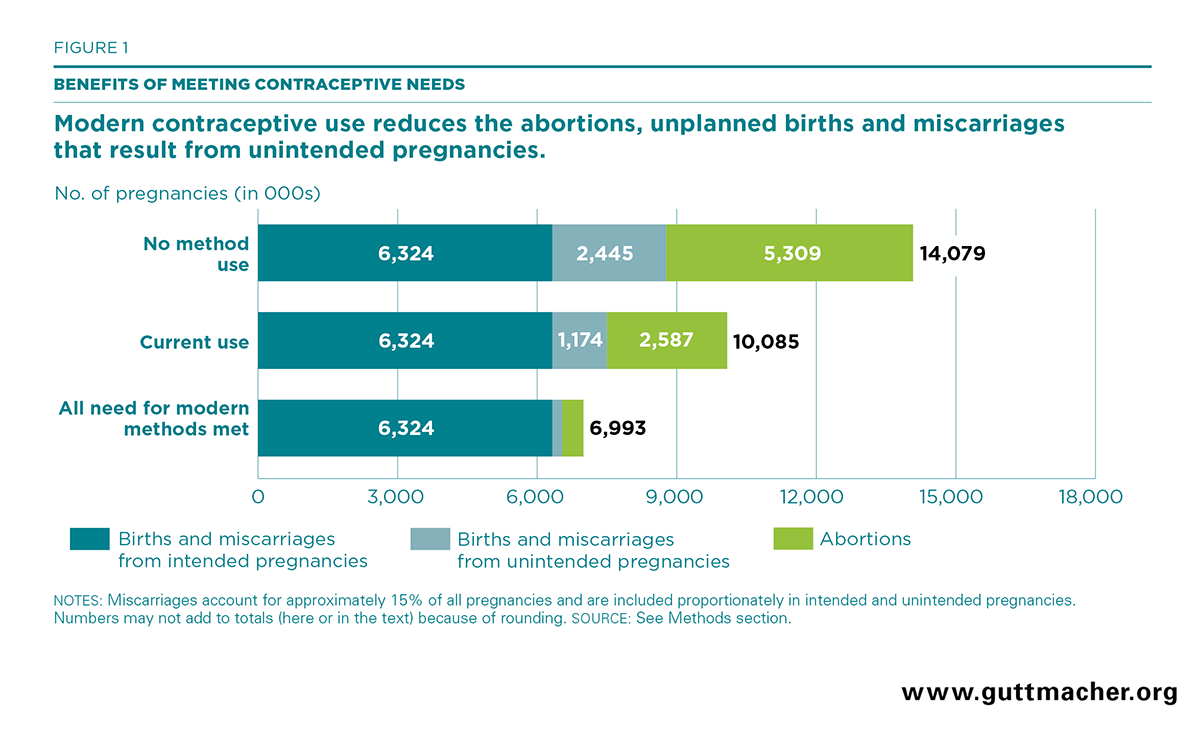
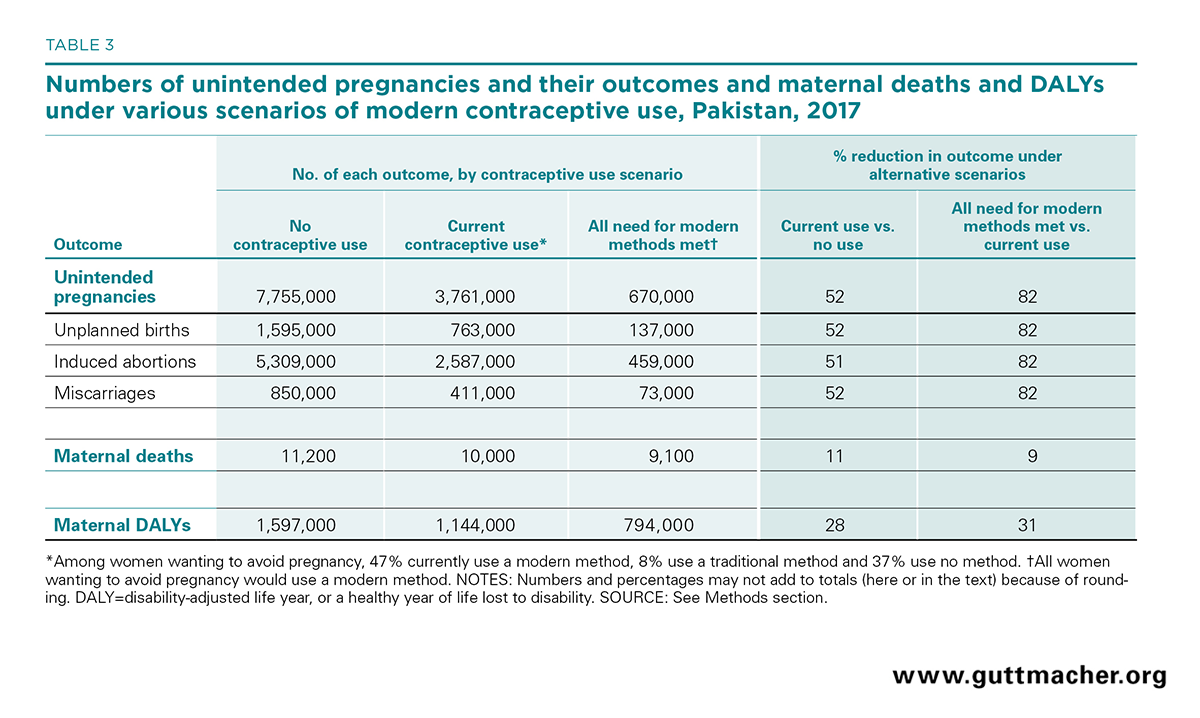
At the 2017–2018 level of modern contraceptive use, Pakistani women have roughly 3.8 million unintended pregnancies annually; approximately 1.2 million end in unplanned birth or miscarriage and 2.6 million end in induced abortion (Figure 1 and Table 3). We calculated the outcomes of a hypothetical scenario in which no women use modern contraceptives, in order to determine the impact that current contraceptive use has on preventing unintended pregnancies. Without any contraceptive use, there would be approximately 7.8 million unintended pregnancies in Pakistan each year. Using current estimates of birth wantedness and abortion rates, we estimate that out of those hypothetical unintended pregnancies, 2.4 million would likely end in unplanned birth or miscarriage and 5.3 million would end in abortion, and a large proportion of these abortions would likely be unsafe.18 Thus, the current level of modern contraceptive use already yields considerable benefits by averting an estimated 4.0 million unintended pregnancies and 2.7 million abortions each year.
Because childbirth carries health risks and unsafe abortion is prevalent, the pregnancies prevented by the current level of contraceptive use in turn prevent 1,200 maternal deaths and the loss of 453,000 years of healthy life among women in Pakistan each year. This represents an 11% reduction in maternal deaths and a 28% reduction in DALYs, compared with the hypothetical scenario in which no modern methods are used.
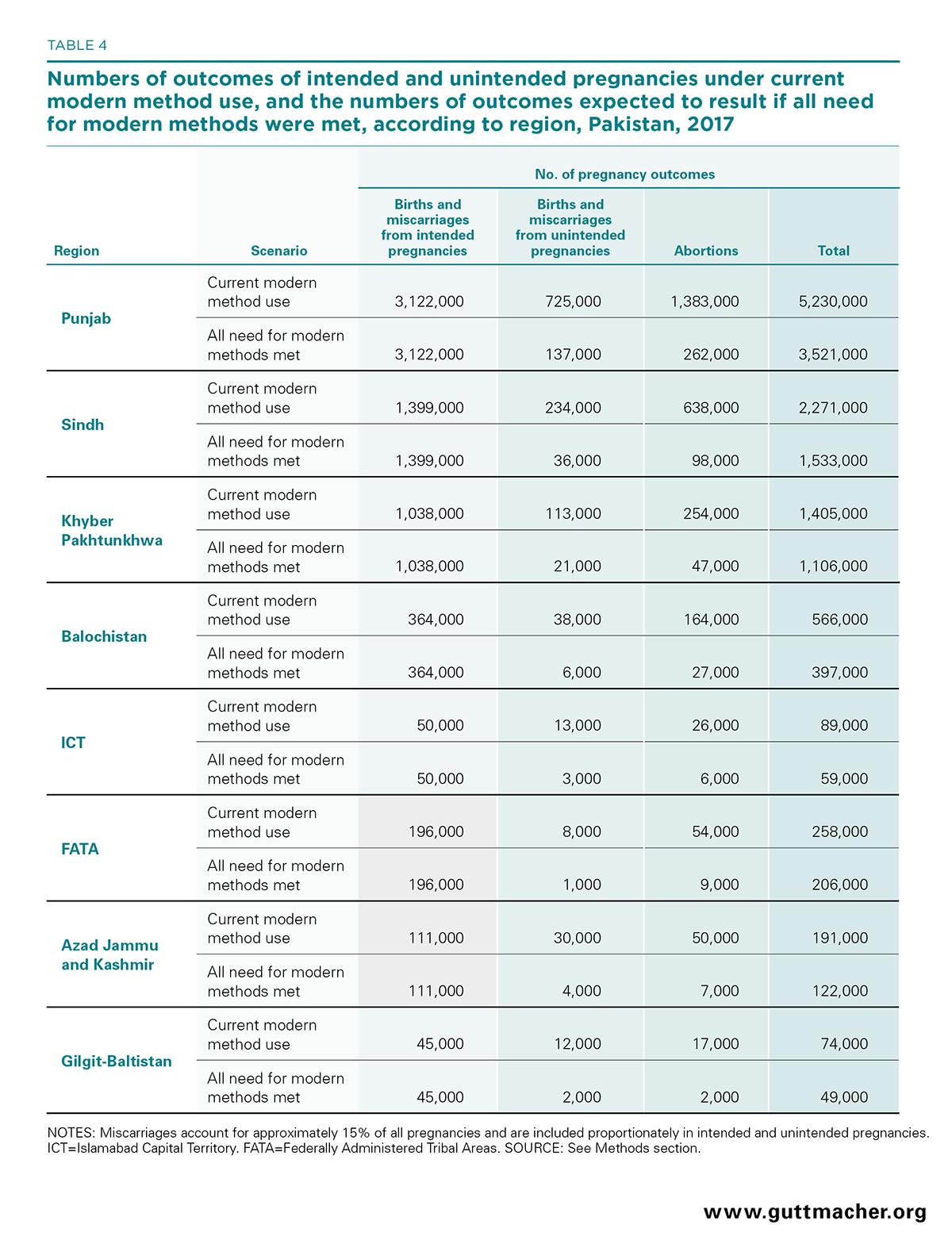
We expect that proportionally greater health benefits will accrue as larger proportions of women who want to avoid a pregnancy begin using a modern contraceptive method. Under a hypothetical scenario in which all unmet need for modern contraception is fulfilled, the number of unintended pregnancies per year would drop to just 670,000—the number that would be expected to occur as a result of method failure. This would result in 3.1 million fewer unintended pregnancies than currently occur, a reduction of 82%. In absolute numbers, the drop in unintended pregnancies would be largest in Punjab (1.7 million; Table 4), and the percentage reduction would range from 77% in ICT to 86% in both Gilgit-Baltistan and Azad Jammu and Kashmir. Compared with current levels, this scenario would result in an 82% reduction in the national annual numbers of unplanned births, abortions and miscarriages, a decline of nearly 1,000 in the number of maternal deaths, and the prevention of 350,000 DALYs. The number of induced abortions would decline by 2.1 million, the majority of which would likely be unsafe. These outcomes could dramatically improve the well-being of women and their families throughout the country.
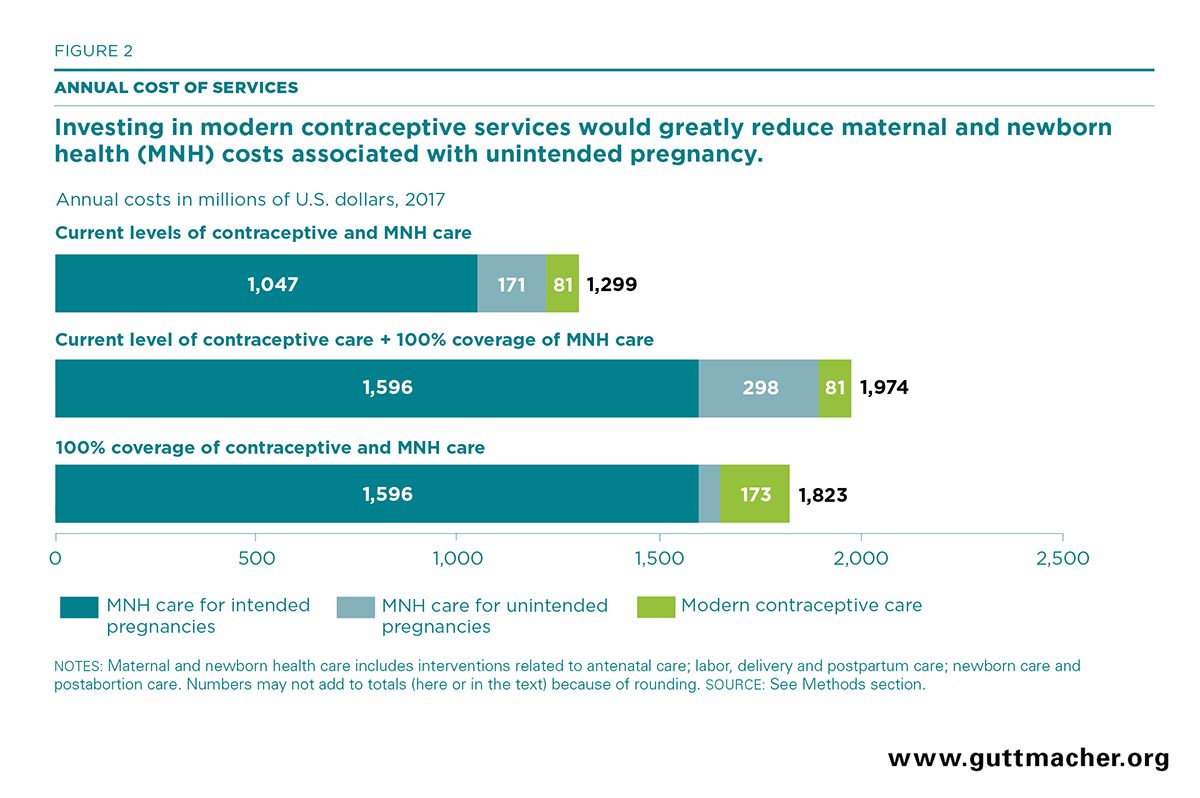
Fully meeting the need for modern contraception would require large investments in improving the country’s health infrastructure, training health care providers and providing outreach services. It would increase the annual cost of providing modern contraceptive services from the current estimate of $81 million to $173 million (Figure 2), a total that includes both direct and indirect costs, including contraceptive commodities, staff salaries, health infrastructure upgrades, contraceptive counseling and communication activities for behavior change.49
Need for and Costs of Improved Coverage of Maternal and Newborn Health Care
Maternal and newborn health care is necessary to protect and enhance the health of women and their babies throughout pregnancy, delivery and the postpartum period, and WHO has established internationally accepted standards for such care. We have used these standards to gauge the adequacy of current maternal and newborn health care in Pakistan and to estimate the costs of fulfilling unmet need for such care. It is beyond the scope of this report to estimate the benefits to women and newborns of different scenarios of maternal and newborn health service provision, but a related analysis estimated that by providing all pregnant women with recommended maternal health care, Pakistan would reduce maternal deaths by 76%.52
Coverage of maternal and newborn health care varies widely across Pakistan’s regions. The proportion of pregnant women who make four or more antenatal care visits is lowest (23%) in Balochistan, which is one of the poorest provinces, and highest (80%) in ICT (not shown).§§11 The proportion of women whose most recent birth took place in a health facility ranges from 37% in Balochistan to 88% in ICT. For the country as a whole, only 27% of women who experience serious medical complications during pregnancy or delivery are estimated to have received the care that they or their newborns need.49 Fewer than 40% of newborns have their first postnatal checkup in the first two days after birth in Balochistan, Gilgit-Baltistan and FATA (34–39%), while three-quarters receive such essential care in Sindh (75%) and ICT (77%).4 Similarly, fewer than 30% of women in Balochistan and FATA have their first postpartum checkup within two days of delivery, compared with 73% in ICT.11
Bringing the full package of recommended maternal and newborn health care (a wide array of interventions related to antenatal care; labor, delivery and postpartum care; newborn care and postabortion care) to all women who need it would require significant financial investments. Based on 2017 amounts, the total cost of providing this package of care in Pakistan is an estimated $1.2 billion (Figure 2), which includes both direct and indirect costs. The largest proportion of the total costs are for labor and delivery care (65%), while antenatal care accounts for 19%, postabortion care for 13% and newborn care for 3%.
In the absence of increased investment in contraception, providing maternal and newborn health care that meets WHO standards for all pregnant women would cost $1.894 billion annually: $1.596 billion for care for women with intended pregnancies and $298 million for those with unintended pregnancies.49 This scenario represents an additional $675 million compared with current costs. The largest cost increase, $219 million, would be in Punjab, followed by Khyber Pakhtunkhwa and Sindh, which would increase by $179 million and $130 million, respectively (not shown). This would place a serious financial burden on a country whose resources are already constrained.
Investing in Modern Contraception and Maternal and Newborn Health Care
The contraceptive use scenarios discussed above assume that current levels of maternal and newborn health care remain constant; likewise, the scenarios describing the costs of maternal and newborn care assume contraceptive care (and therefore unintended pregnancy) remain constant. By preventing unintended pregnancies, modern contraceptive use reduces the need for care related to abortion or to carrying those pregnancies to term. Thus, an increase in modern contraceptive services reduces the overall costs associated with maternal and newborn care. Therefore, simultaneously expanding both modern contraceptive services and maternal and newborn care would result in cost savings compared with expanding either set of services alone.
Under an ideal scenario in which both modern contraceptive services and maternal and newborn care are provided to all women in Pakistan who need them, the cost of both types of services combined would be $1.823 billion: $173 million for full modern contraceptive care and $1.649 billion for full maternal and newborn health care (Figure 2). This is equivalent to an average cost of $8.55 per capita to fully meet needs for both of these services.
In comparison, it would cost almost $2 billion in a hypothetical scenario in which modern contraceptive services remained at current levels but maternal and newborn health care was expanded to serve all women in need: $81 million for current contraceptive care plus $1.894 billion for full maternal and newborn care. Investing in both services simultaneously would result in a savings of nearly $152 million. Although the cost for contraceptive services is higher in the ideal scenario than in a scenario in which only care for pregnant women and newborns is expanded, the savings associated with averting unintended pregnancies more than covers that cost. In short, the cost of averting an unintended pregnancy is much lower than the cost of maternal and newborn health care associated with that pregnancy, such that every additional dollar spent on modern contraceptives services lowers the cost of maternal and newborn care by $2.66.
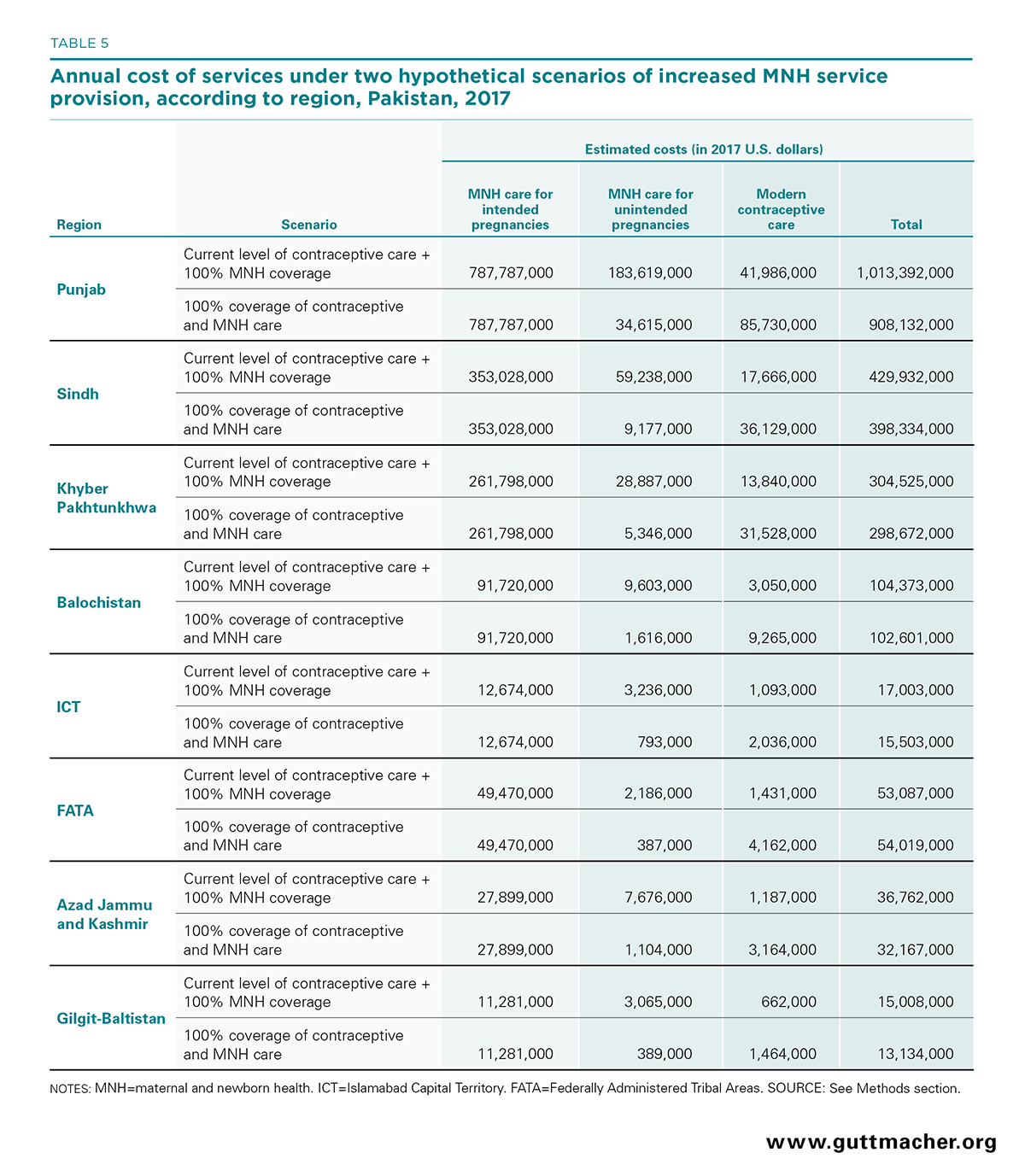
Almost all of the regions would also see cost savings from simultaneous investment in both sets of services as compared with investing only in contraceptive care. Costs would be highest in Punjab, which is expected given its population size: Fully providing both maternal and newborn care and modern contraceptive services would be $908 million, but the cost of providing full maternal and newborn care would be $1.0 billion if modern contraceptive coverage remained at current levels, yielding a cost savings of $105 million (Table 5). The cost savings of investing in both sets of services (rather than just maternal and newborn health care) would vary between $1.5 million and $33 million for the other regions except FATA, where there would be a slight cost increase.
Benefits for Poor Women
Poorer women stand to gain more than wealthier women from improved coverage of modern contraceptive services. If unmet need for modern contraception were fully satisfied while maintaining current levels of maternal and newborn care, there would be a 91% decline in unintended pregnancies among women from the poorest households in Pakistan, compared with a 74% decline among women from the wealthiest households.49
Need for Additional Funding
Pakistan is one of the focus countries of the FP2020 partnership, which supports the rights of women and girls to decide freely whether, when and how many children they wish to have.53 At the London Family Planning Summit in 2012, the Pakistan government committed to the partnership that it would address the policy, financing, delivery, social and cultural barriers to women’s full access to contraceptive information, services and supplies.54,55
As part of this partnership, the Pakistan government committed to increasing the contraceptive prevalence rate to 50% and expenditures on family planning to $2.50 per capita, both by 2020. Current expenditures on family planning for 2017–2018 have been estimated at $1.09 per capita, according to a recent study.56 The government has also committed to improving the mix of contraceptives available to women, expanding the use of long-acting reversible methods, and improving counseling services and information provided to women, men and other community gatekeepers to reduce unmet need among those women who cite spousal or religious opposition as a reason for nonuse. In addition, the government has committed to improving the public procurement and logistics system to ensure uninterrupted availability of contraceptives.57
Achieving significant improvements in maternal and newborn health care coverage and reductions in maternal mortality will require greater investments in health care infrastructure. In 2013–2014, the National Health Accounts for Pakistan estimated that the country was spending about $40 per capita on health services. In 2015–2016, this estimate had increased to about $45 per capita, with greater contributions to both maternal and family planning expenditures.58 Current data on spending for maternal and newborn care is not available, but overall budgets on health care have increased, which may mean that the share of expenditures on maternal and newborn health care also has increased.59
As the results in this report show, an effective strategy for reducing maternal and infant death and disability is to empower couples to plan the size of their families by expanding modern contraceptive services, so they can have the number of children they want, when they want them,. As women and couples increasingly desire to have smaller families, the demand for modern contraceptive services will only grow. The responsibility for fulfilling this demand will have to be shared by various stakeholders, including provincial governments, the federal government, the private sector and international development partners.
Improving access to contraceptive services should entail a multifaceted approach. Recent research shows that many women who do not use contraceptives cite concerns about health and side effects, have personal or partner opposition, or do not feel they are at risk of an unintended pregnancy.60 In addition to making family planning easily available, stakeholders should ensure that women have access to comprehensive services that include contraceptive counseling to help women understand their pregnancy risk and possible method-related side effects, as well as dispel any misinformation or myths regarding contraception. Comprehensive services should also provide women with their choice of a wide range of contraceptive methods, help them identify one or more that meets their needs and preferences, and facilitate switching for women who are unsatisfied with their method. Improving publicly funded family planning—by increased investment, continuous quality improvements and adoption of client-based strategies—is especially important for meeting the needs of those who are the most economically disadvantaged.61
Urgent action is needed to implement the 2018 Council of Common Interests (CCI) recommendations on specific actions to improve contraceptive service provision.8 This is essential for closing the gap in unmet need for modern contraception in the country. The CCI’s recommendations also highlight the need to decrease maternal and infant death and disability by reducing unintended pregnancies and promoting maternal and infant health care and contraceptive services, particularly through the public health system as a cost-efficient source of care. Improving access to both contraceptive and maternal and newborn health services and improving the quality of these services would enable Pakistan to achieve the CCI’s recommendations and national FP2020 goals more quickly.
Investment in these services promotes women’s health and rights and the health of their children, and it also saves money. Overall, every additional dollar spent on contraceptive services would reduce required expenditure on maternal and newborn care by more than $2.50. The benefits of improved quality of life and lives saved would be an incalculable gain to Pakistani women and their families.
FOOTNOTES
*Antenatal, labor, delivery, postpartum and newborn care, and care for women who experience stillbirth, miscarriage, ectopic pregnancy or induced abortion.
†Sterilization, injectables, long-acting reversible methods (implants and IUDs), standard days method, pills, condoms and other supply methods.
‡DALYs are a measure of the number of years of healthy life lost as a result of premature death and disability. One DALY equals one lost year of healthy life. The measure was developed to provide comparable estimates of the burdens of premature death and disability attributable to different causes across contexts.
§Our definition of unmet need differs from the standard definition used by the DHS in that DHS defines women using traditional methods as having their contraceptive needs met. Our definition also differs from the DHS definition in that we present unmet need only among women who want to avoid pregnancy, not among all married women.
**Information on sexual activity, contraceptive use and pregnancy desires among unmarried women in Pakistan is not available; therefore, our analyses of contraceptive use and needs are based on the behaviors of married women as measured in the 2017–2018 PDHS, and all married women are assumed to be sexually active. The level of sexual activity among unmarried women is likely to be very low, based on information available for the subregion of South Asia.14 Because unmarried women’s share of total pregnancies will be very small, all pregnancies are included in the analyses and in the results presented.
††This report considers all pregnancies in Pakistan in calculating costs and benefits of the health care that women need.
‡‡WHO recently updated its basic antenatal care guidance, recommending that pregnant women have at least eight contacts with an antenatal care provider. Because Pakistan has not yet adopted these revised recommendations, and because what constitutes a "contact" is not yet clearly defined, we continue to reference the previous recommendation, which required that women receive four antenatal care visits to fully meet the standard of essential health care.
§§The proportion of women who had four antenatal care visits, the proportion who delivered in a health facility and the proportion who had their first postpartum checkup within two days of delivery are measured from the last birth occurring in the three years preceding the 2017–2018 PDHS.
Suggested Citation
Sundaram A et al., Adding It Up: Costs and Benefits of Meeting the Contraceptive and Maternal and Newborn Health Needs of Women in Pakistan, New York: Guttmacher Institute, 2019, http://www.guttmacher.org/report/adding-it-up-meeting-contraceptive-mnh-needs-pakistan.
Acknowledgments
This report was written by Aparna Sundaram, Rubina Hussain and Emma Pliskin of the Guttmacher Institute; Zeba Sathar and Sabahat Hussain of the Population Council, Islamabad, Pakistan; and Eva Weissman, independent consultant. It was edited by Chris Olah and Haley Ball. The authors are grateful for contributions provided by the following Guttmacher colleagues: Suzette Audam, Ann Biddlecom, Kate Castle, Jacqueline E. Darroch, Ayana Douglas-Hall, Susheela Singh and Elizabeth Sully; and Population Council colleagues: Ali Mir, Gul Rashida and Maqsood Sadiq. They also thank the external reviewers, Afeef Mahmood and Hanid Mukhtar, as well as the Government of Pakistan and the Technical Resource Facility for sharing data.
This report has been made possible by UK Aid from the UK Government. The views expressed are those of the authors and do not necessarily reflect the positions and policies of the UK Government. The Guttmacher Institute gratefully acknowledges the unrestricted funding it receives from many individuals and foundations—including major grants from the William and Flora Hewlett Foundation and the David and Lucile Packard Foundation—which undergirds all of the Institute’s work.
REFERENCES
1. United Nations Children’s Fund (UNICEF), The State of the World’s Children 2009, New York: UNICEF, 2008, https://www.unicef.org/sowc09/docs/SOWC09-FullReport-EN.pdf.
2. National Institute of Population Studies (NIPS) and ICF, Pakistan Demographic and Health Survey 2012–13, Islamabad, Pakistan and Calverton, MD, USA: NIPS and ICF, 2013, http://dhsprogram.com/publications/publication-FR290-DHS-Final-Reports.cfm.
3. NIPS and ICF, Pakistan Demographic and Health Survey 1990–1991, Islamabad, Pakistan and Calverton, MD, USA: NIPS and ICF, 1992, https://dhsprogram.com/publications/publication-fr29-dhs-final-reports.cfm.
4. NIPS and ICF, Pakistan Demographic and Health Survey 2017–18, Islamabad, Pakistan and Rockville, MD, USA: NIPS and ICF, 2019, https://dhsprogram.com/pubs/pdf/FR354/FR354.pdf.
5. United Nations Population Fund (UNFPA), Population Situation Analysis of Pakistan, Islamabad, Pakistan: UNFPA, 2016, https://www.fp2030.org/resources/resources-unfpa-population-situation-analysis-pakistan.
6. UNDP Support to the Implementation of the 2030 Agenda for Sustainable Development, New York: United Nations Development Programme, 2016, http://www.undp.org/content/undp/en/home/librarypage/sustainable-development-goals/undp-support-to-the-implementation-of-the-2030-agenda.html.
7. Population Council, Pakistan, Pakistan 2017: Progress and Commitments in Family Planning, Population Council, 2017.
8. Law and Justice Commission of Pakistan and Ministry of National Health Services, Regulations and Coordination, Government of Pakistan, National Symposium on Alarming Population Growth: A Call for Action, Islamabad, Pakistan: UNFPA and Population Council, 2018.
9. Pakistan Bureau of Statistics, Pakistan Population Census 2017, 2018.
10. Population Division, United Nations (UN) Department of Economic and Social Affairs, World Population Prospects: The 2017 Revision, World population 2017 wallchart, 2017.
11. NIPS and ICF, special tabulations of data from the Pakistan Demographic and Health Survey 2017–18.
12. Ministry of Planning, Development and Reform, National Poverty Report 2015–16, 2018.
13. Darroch J, Singh S and Weissman E, Adding It Up: The Costs and Benefits of Investing in Sexual and Reproductive Health 2014—Estimation Methodology, New York: Guttmacher Institute, 2016, https://www.guttmacher.org/report/adding-it-costs-and-benefits-investing-sexual-and-reproductive-health-2014-methodology.
14. Darroch JE, Adding It Up: Investing in Contraception and Maternal and Newborn Health, 2017—Estimation Methodology, New York: Guttmacher Institute, 2018, https://www.guttmacher.org/report/adding-it-up-investing-in-contraception-maternal-newborn-health-2017-methodology.
15. Trussell J, Contraceptive failure in the United States, Contraception, 2011, 83(5):397–404, doi:10.1016/j.contraception.2011.01.021.
16. Bradley S et al., Global contraceptive failure rates: Who is most at risk?, paper presented at the annual meeting of the Population Association of America, Chicago, IL, USA, Apr. 27–29, 2017.
17. Arévalo M, Jennings V and Sinai I, Efficacy of a new method of family planning: the Standard Days Method, Contraception, 2002, 65(5):333–338, doi:10.1016/S0010-7824(02)00288-3.
18. Sather Z et al., Induced abortions and unintended pregnancies in Pakistan, Studies in Family Planning, 2014, 45(4):471–491, doi:10.1111/j.1728-4465.2014.00004.x.
19. Leridon H, Human Fertility: The Basic Components, Chicago, IL, USA: University of Chicago Press, 1977.
20. NIPS and ICF, Pakistan Demographic and Health Survey 2006–07, Islamabad, Pakistan and Calverton, MD, USA: NIPS and ICF, 2008, http://dhsprogram.com/publications/publication-fr200-dhs-final-reports.cfm.
21. Say L et al., Maternal Mortality in 2005: Estimates Developed by WHO, UNICEF, UNFPA and the World Bank, Geneva: World Health Organization (WHO), 2008.
22. Maternal Mortality Measurement Resource, Regression models, http://www.maternal-mortality-measurement.org.uk/MMMResource_Tool_RegressionModels.html.
23. Institute for Health Metrics and Evaluation, Global Health Data Exchange, GBD results tool, deaths and DALYs (disability-adjusted life years), Pakistan, 2018, http://ghdx.healthdata.org/gbd-results-tool.
24. UNFPA Technical Division, Revised Cost Estimates for the Implementation of the Programme of Action for the International Conference on Population and Development: A Methodological Report, New York: UNFPA, 2009, https://www.unfpa.org/sites/default/files/resource-pdf/Revised_Costing_ICPD.pdf.
25. UNFPA Procurement Services, Reproductive Health Interchange, https://www.unfpaprocurement.org/rhi-home.
26. UNICEF Supply Catalogue, https://supply.unicef.org/.
27. Sathar Z, Population Council, Islamabad, Pakistan, personal communication, February 2018.
28. Ministry of Finance, Revision of of Basic Pay Scales & Allowances of Civil Servants of the Federal Government (2017), Islamabad, Pakistan: Government of Pakistan, 2017.
29. Technical Resource Facility (TRF), A Report on Costing Essential Package of Health Services Primary Health Care Facilities in Sindh, Pakistan: TRF, 2014.
30. TRF, A Report on Costing Essential Package of Health Services Primary Health Care Facilities in Punjab, Pakistan: TRF, 2012.
31. TRF, A Report on Costing Essential Package of Health Services Primary Health Care Facilities in Khyber Pakhtunkhwa, Pakistan: TRF, 2012.
32. NIPS and ICF, special tabulations of data from the Pakistan Demographic and Health Survey 2012–13.
33. WHO et al., Trends in Maternal Mortality: 1990 to 2015: Estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division, Geneva: WHO, 2015, http://www.who.int/reproductivehealth/publications/monitoring/maternal-mortality-2015/en/.
34. Ronsmans C and Graham WJ, Maternal mortality: who, when, where, and why, Lancet, 2006, 368(9542):1189–1200, doi:10.1016/S0140-6736(06)69380-X.
35. Karlsen S et al., The relationship between maternal education and mortality among women giving birth in health care institutions: Analysis of the cross sectional WHO Global Survey on Maternal and Perinatal Health, BMC Public Health, 2011, 11(1):606, doi:10.1186/1471-2458-11-606.
36. Say L et. al., Global causes of maternal death: a WHO systematic analysis, Lancet Global Health, 2014, 2(6):e323–e333, doi:10.1016/S2214-109X(14)70227-X .
37. Puri M et al., Abortion incidence and unintended pregnancy in Nepal, International Perspectives on Sexual and Reproductive Health, 2016, 42(4):197–209, doi:10.1363/42e2116.
38. Singh S et al., The incidence of abortion and unintended pregnancy in India, 2015, Lancet Global Health, 2018, 6(1):e111–e120, doi:10.1016/S2214-109X(17)30453-9.
39. United Nations Population Division, Abortion Policies: A Global Review, New York: UN, 2002.
40. Lawn JE et al., Newborn survival in low resource settings—Are we delivering?, BJOG, 2009, 116(Suppl. 1):49–59, doi:10.1111/j.1471-0528.2009.02328.x.
41. UN Inter-agency Group for Child Mortality Estimation, Levels & Trends in Child Mortality: Report 2015, New York: UNICEF, 2015, https://resourcecentre.savethechildren.net/library/levels-trends-child-mortality-report-2015.
42. Bhutta ZA et al., Interventions to address maternal, newborn, and child survival: What difference can integrated primary health care strategies make?, Lancet, 2008, 372:972–989.
43. Health Department of Sindh, MNCH Program, 2018, https://www.sindhhealth.gov.pk/MNCH-Program.
44. Khan S, National Maternal, Newborn and Child Health Program, NWFP, Peshawar, Pakistan: Government of Khyber Pakhtunkhwa.
45. Health Department of Sindh, LHW Program, 2018, https://www.sindhhealth.gov.pk/LHW-Program.
46. Directorate General of Health Services, Government of the Punjab, National Programme for Family Planning and Primary Health Care, 2015, https://dghs.punjab.gov.pk/family_planning_primary_health_care.
47. Expanded Program on Immunization, Ministry of National Health Services, Regulations and Coordination, Government of Pakistan, 2018, http://www.epi.gov.pk/.
48. Directorate General of Health Services, Government of the Punjab, Malaria Control Program, https://dghs.punjab.gov.pk/rollback_malaria.
49. See Methods section and online methodology (see pdf attachment at top right).
50. Polis CB et al., Typical-use contraceptive failure rates in 43 countries with Demographic and Health Survey data: summary of a detailed report, Contraception, 2016, 94(1):11–17, doi:10.1016/j.contraception.2016.03.011.
51. Sundaram A et al., Contraceptive failure in the United States: Estimates from the 2006–2010 National Survey of Family Growth, Perspectives on Sexual and Reproductive Health, 2017, 49(1):7–16, doi:10.1363/psrh.12017.
52. Special tabulations of data from Guttmacher Institute, Adding it up: the costs and benefits of investing in sexual and reproductive health, Fact Sheet, 2017, https://www.guttmacher.org/fact-sheet/adding-it-up-contraception-mnh-2017.
53. Scoggins S and Bremner J, FP2020: The Way Ahead, 2016–2017, Family Planning 2020 (FP2020), 2017, http://2016-2017progress.familyplanning2020.org/en.
54. Family Planning 2020 Commitment: Government of Pakistan, Family Planning Summit for Safer, Healthier and Empowered Futures, London, UK, 2017, https://www.familyplanning2020.org/sites/default/files/Govt_Pakistan_FP2020_Commitment_2017_0.pdf.
55. Pakistan FP2020 Commitment, London Summit on Family Planning, 2012.
56. Razzaq S, Family Planning Expenditures in Pakistan 2017–18: Netherlands Interdisciplinary Demographic Institute and UNFPA Survey Results, 2018.
57. FP2020, 2016 FP2020annual commitment update questionnaire response: Pakistan, http://www.familyplanning2020.org/sites/default/files/FP2020_2016_Annual_Commitment_Update_Questionnaire-Pakistan_DLC.pdf.
58. Akhtar S, National Health Accounts Pakistan 2015–16, Pakistan Bureau of Statistics, 2018.
59. Ministry of Finance, Government of Pakistan, Pakistan Economic Survey 2017–18, 2018, http://www.finance.gov.pk/survey_1718.html.
60. Sedgh G, Ashford L and Hussain R, Unmet Need for Contraception in Developing Countries: Examining Women’s Reasons for Not Using a Method, New York: Guttmacher Institute, 2016, https://www.guttmacher.org/report/unmet-need-for-contraception-in-developing-countries.
61. Cleland J et al., Family planning: the unfinished agenda, Lancet, 2006, 368(9549):1810–1827, doi:10.1016/S0140-6736(06)69480-4.
Additional Downloads
- Methodology Appendix adding-it-up-pakistan-methodology-appendix.pdf
Topic
Global